Intracranial pressure: Difference between revisions
No edit summary |
CSV import |
||
| Line 1: | Line 1: | ||
{{SI}} | |||
{{Infobox medical condition | |||
| name = Intracranial pressure | |||
| image = [[File:Brain_herniation_MRI.jpg|250px]] | |||
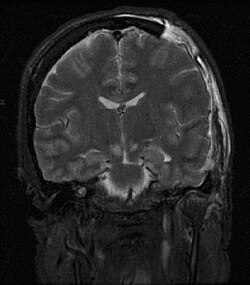
| caption = MRI showing brain herniation due to increased intracranial pressure | |||
| field = [[Neurology]] | |||
| synonyms = ICP | |||
| symptoms = [[Headache]], [[vomiting]], [[altered mental status]], [[papilledema]] | |||
| complications = [[Brain herniation]], [[cerebral ischemia]], [[death]] | |||
| onset = Sudden or gradual | |||
| duration = Variable | |||
| causes = [[Traumatic brain injury]], [[stroke]], [[brain tumor]], [[hydrocephalus]], [[meningitis]] | |||
| risks = [[Hypertension]], [[coagulopathy]], [[infection]] | |||
| diagnosis = [[Clinical examination]], [[CT scan]], [[MRI]], [[lumbar puncture]] | |||
| differential = [[Migraine]], [[tension headache]], [[subarachnoid hemorrhage]] | |||
| treatment = [[Osmotic therapy]], [[surgical decompression]], [[ventricular drain]] | |||
| medication = [[Mannitol]], [[hypertonic saline]], [[corticosteroids]] | |||
| prognosis = Depends on cause and treatment | |||
| frequency = Common in [[intensive care unit]] settings | |||
}} | |||
'''Intracranial pressure''' (ICP) is the pressure within the cranial cavity, the space inside the skull where the brain resides. This pressure is influenced by the volume of three main components: brain tissue, cerebrospinal fluid, and blood. Normal ICP ranges from 5 to 15 mmHg in a supine adult. Alterations in ICP can have profound effects on cerebral physiology, leading to serious complications or even death if not addressed promptly. | '''Intracranial pressure''' (ICP) is the pressure within the cranial cavity, the space inside the skull where the brain resides. This pressure is influenced by the volume of three main components: brain tissue, cerebrospinal fluid, and blood. Normal ICP ranges from 5 to 15 mmHg in a supine adult. Alterations in ICP can have profound effects on cerebral physiology, leading to serious complications or even death if not addressed promptly. | ||
[[File:ICP measurement.jpg|thumb|ICP measurement]] | [[File:ICP measurement.jpg|left|thumb|ICP measurement]] | ||
== Understanding Intracranial Pressure == <!--T:2--> | == Understanding Intracranial Pressure == <!--T:2--> | ||
The balance between the production and absorption of cerebrospinal fluid ([[Cerebrospinal fluid|CSF]]) and the blood flow to the brain primarily governs ICP. This delicate balance is guided by the Monro-Kellie doctrine, which postulates that the total volume of blood, CSF, and brain tissue remains constant in the rigid skull. Any increase in one of these components necessitates a decrease in one or both of the other two to maintain a normal ICP.<ref>{{cite journal |last1=Mokri |first1=Bahram |title=The Monro-Kellie hypothesis: applications in CSF volume depletion |journal=Neurology |volume=56 |issue=12 |pages=1746–1748 |year=2001 |pmid=11425944 |doi=10.1212/wnl.56.12.1746}}</ref> | The balance between the production and absorption of cerebrospinal fluid ([[Cerebrospinal fluid|CSF]]) and the blood flow to the brain primarily governs ICP. This delicate balance is guided by the Monro-Kellie doctrine, which postulates that the total volume of blood, CSF, and brain tissue remains constant in the rigid skull. Any increase in one of these components necessitates a decrease in one or both of the other two to maintain a normal ICP.<ref>{{cite journal |last1=Mokri |first1=Bahram |title=The Monro-Kellie hypothesis: applications in CSF volume depletion |journal=Neurology |volume=56 |issue=12 |pages=1746–1748 |year=2001 |pmid=11425944 |doi=10.1212/wnl.56.12.1746}}</ref> | ||
== Physiological Variations and Measurement of Intracranial Pressure == | |||
== Physiological Variations and Measurement of Intracranial Pressure == | ICP can vary physiologically due to changes in body position, respiration, and arterial pressure. However, pathological elevations or reductions in ICP can lead to serious health issues, including stroke, traumatic brain injury, hydrocephalus, or brain tumors.<ref>{{cite journal |last1=Kristiansson |first1=Helena |last2=Nissborg |first2=Erik |last3=Bartek |first3=Jiri |last4=Truvé |first4=K√•re |last5=Romner |first5=Bertil |title=Measuring elevated intracranial pressure through noninvasive methods: a review of the literature |journal=Journal of Neurosurgical Anesthesiology |volume=25 |issue=4 |pages=372–385 |year=2013 |pmid=23872804 |doi=10.1097/ANA.0b013e318293f5c2}}</ref> | ||
ICP can vary physiologically due to changes in body position, respiration, and arterial pressure. However, pathological elevations or reductions in ICP can lead to serious health issues, including stroke, traumatic brain injury, hydrocephalus, or brain tumors.<ref>{{cite journal |last1=Kristiansson |first1=Helena |last2=Nissborg |first2=Erik |last3=Bartek |first3=Jiri |last4=Truvé |first4= | |||
Measuring ICP is crucial in the diagnosis and management of these conditions. Direct invasive methods like ventriculostomy or intraparenchymal monitoring are the gold standard for accurate ICP measurement, although non-invasive methods are under development.<ref>{{cite journal |last1=Rabiei |first1=Katayoun |last2=Högberg |first2=Daniel |last3=Klein |first3=Christian |last4=Göthlin |first4=Jan |last5=Ng |first5=Michaela |last6=Wanecek |first6=Mikael |last7=Reinsfelt |first7=Bodil |title=Accuracy in the measurement of intracranial pressure: systematic review and meta-analysis |journal=Journal of Neurosurgery |volume=132 |issue=5 |pages=1479–1494 |year=2019 |pmid=31125970 |doi=10.3171/2019.2.JNS182507}}</ref> | Measuring ICP is crucial in the diagnosis and management of these conditions. Direct invasive methods like ventriculostomy or intraparenchymal monitoring are the gold standard for accurate ICP measurement, although non-invasive methods are under development.<ref>{{cite journal |last1=Rabiei |first1=Katayoun |last2=Högberg |first2=Daniel |last3=Klein |first3=Christian |last4=Göthlin |first4=Jan |last5=Ng |first5=Michaela |last6=Wanecek |first6=Mikael |last7=Reinsfelt |first7=Bodil |title=Accuracy in the measurement of intracranial pressure: systematic review and meta-analysis |journal=Journal of Neurosurgery |volume=132 |issue=5 |pages=1479–1494 |year=2019 |pmid=31125970 |doi=10.3171/2019.2.JNS182507}}</ref> | ||
== Consequences of Altered Intracranial Pressure == | == Consequences of Altered Intracranial Pressure == | ||
When ICP is either excessively high or low, it can lead to severe neurological impairment and may become life-threatening. Increased ICP can reduce cerebral blood flow, resulting in brain ischemia and neuronal death. In contrast, decreased ICP, though less common, can lead to conditions such as spontaneous intracranial hypotension, characterized by postural headaches.<ref>{{cite journal |last1=Mokri |first1=Bahram |title=Spontaneous low pressure, low CSF volume headaches: spontaneous CSF leaks |journal=Headache |volume=53 |issue=7 |pages=1034–1053 |year=2013 |pmid=23808994 |doi=10.1111/head.12149}}</ref> | When ICP is either excessively high or low, it can lead to severe neurological impairment and may become life-threatening. Increased ICP can reduce cerebral blood flow, resulting in brain ischemia and neuronal death. In contrast, decreased ICP, though less common, can lead to conditions such as spontaneous intracranial hypotension, characterized by postural headaches.<ref>{{cite journal |last1=Mokri |first1=Bahram |title=Spontaneous low pressure, low CSF volume headaches: spontaneous CSF leaks |journal=Headache |volume=53 |issue=7 |pages=1034–1053 |year=2013 |pmid=23808994 |doi=10.1111/head.12149}}</ref> | ||
== Treatment Strategies for Abnormal Intracranial Pressure == | |||
== Treatment Strategies for Abnormal Intracranial Pressure == | |||
The management of abnormal ICP is a critical aspect of neurocritical care. Treatment strategies for elevated ICP include sedation, hyperventilation, osmotherapy (using osmotic diuretics such as mannitol), and surgical interventions like decompressive craniectomy. On the other hand, treatments for low ICP typically involve addressing the underlying cause, such as repairing CSF leaks.<ref>{{cite journal |last1=Carney |first1=N. |last2=Totten |first2=A. M. |last3=O'Reilly |first3=C. |last4=Ullman |first4=J. S. |last5=Hawryluk |first5=G. W. |last6=Bell |first6=M. J. |last7=Bratton |first7=S. L. |last8=Chesnut |first8=R. |last9=Harris |first9=O. A. |last10=Kissoon |first10=N. |last11=Rubiano |first11=A. M. |last12=Shutter |first12=L. |last13=Tasker |first13=R. C. |last14=Vavilala |first14=M. S. |last15=Wilberger |first15=J. |last16=Wright |first16=D. W. |last17=Ghajar |first17=J. |title=Guidelines for the Management of Severe Traumatic Brain Injury, Fourth Edition |journal=Neurosurgery |volume=80 |issue=1 |pages=6–15 |year=2017 |pmid=27654000 |doi=10.1227/NEU.0000000000001432}}</ref> | The management of abnormal ICP is a critical aspect of neurocritical care. Treatment strategies for elevated ICP include sedation, hyperventilation, osmotherapy (using osmotic diuretics such as mannitol), and surgical interventions like decompressive craniectomy. On the other hand, treatments for low ICP typically involve addressing the underlying cause, such as repairing CSF leaks.<ref>{{cite journal |last1=Carney |first1=N. |last2=Totten |first2=A. M. |last3=O'Reilly |first3=C. |last4=Ullman |first4=J. S. |last5=Hawryluk |first5=G. W. |last6=Bell |first6=M. J. |last7=Bratton |first7=S. L. |last8=Chesnut |first8=R. |last9=Harris |first9=O. A. |last10=Kissoon |first10=N. |last11=Rubiano |first11=A. M. |last12=Shutter |first12=L. |last13=Tasker |first13=R. C. |last14=Vavilala |first14=M. S. |last15=Wilberger |first15=J. |last16=Wright |first16=D. W. |last17=Ghajar |first17=J. |title=Guidelines for the Management of Severe Traumatic Brain Injury, Fourth Edition |journal=Neurosurgery |volume=80 |issue=1 |pages=6–15 |year=2017 |pmid=27654000 |doi=10.1227/NEU.0000000000001432}}</ref> | ||
== Conclusion == | |||
== Conclusion == | |||
In conclusion, intracranial pressure plays a pivotal role in maintaining brain health. Careful monitoring and management of ICP are key to preventing and treating various neurological disorders. | In conclusion, intracranial pressure plays a pivotal role in maintaining brain health. Careful monitoring and management of ICP are key to preventing and treating various neurological disorders. | ||
== References == | == References == | ||
Latest revision as of 01:10, 8 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Intracranial pressure | |
|---|---|
| |
| Synonyms | ICP |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Headache, vomiting, altered mental status, papilledema |
| Complications | Brain herniation, cerebral ischemia, death |
| Onset | Sudden or gradual |
| Duration | Variable |
| Types | N/A |
| Causes | Traumatic brain injury, stroke, brain tumor, hydrocephalus, meningitis |
| Risks | Hypertension, coagulopathy, infection |
| Diagnosis | Clinical examination, CT scan, MRI, lumbar puncture |
| Differential diagnosis | Migraine, tension headache, subarachnoid hemorrhage |
| Prevention | N/A |
| Treatment | Osmotic therapy, surgical decompression, ventricular drain |
| Medication | Mannitol, hypertonic saline, corticosteroids |
| Prognosis | Depends on cause and treatment |
| Frequency | Common in intensive care unit settings |
| Deaths | N/A |
Intracranial pressure (ICP) is the pressure within the cranial cavity, the space inside the skull where the brain resides. This pressure is influenced by the volume of three main components: brain tissue, cerebrospinal fluid, and blood. Normal ICP ranges from 5 to 15 mmHg in a supine adult. Alterations in ICP can have profound effects on cerebral physiology, leading to serious complications or even death if not addressed promptly.

Understanding Intracranial Pressure[edit]
The balance between the production and absorption of cerebrospinal fluid (CSF) and the blood flow to the brain primarily governs ICP. This delicate balance is guided by the Monro-Kellie doctrine, which postulates that the total volume of blood, CSF, and brain tissue remains constant in the rigid skull. Any increase in one of these components necessitates a decrease in one or both of the other two to maintain a normal ICP.<ref>,
The Monro-Kellie hypothesis: applications in CSF volume depletion, Neurology, 2001, Vol. 56(Issue: 12), pp. 1746–1748, DOI: 10.1212/wnl.56.12.1746, PMID: 11425944,</ref>
Physiological Variations and Measurement of Intracranial Pressure[edit]
ICP can vary physiologically due to changes in body position, respiration, and arterial pressure. However, pathological elevations or reductions in ICP can lead to serious health issues, including stroke, traumatic brain injury, hydrocephalus, or brain tumors.<ref>,
Measuring elevated intracranial pressure through noninvasive methods: a review of the literature, Journal of Neurosurgical Anesthesiology, 2013, Vol. 25(Issue: 4), pp. 372–385, DOI: 10.1097/ANA.0b013e318293f5c2, PMID: 23872804,</ref>
Measuring ICP is crucial in the diagnosis and management of these conditions. Direct invasive methods like ventriculostomy or intraparenchymal monitoring are the gold standard for accurate ICP measurement, although non-invasive methods are under development.<ref>,
Accuracy in the measurement of intracranial pressure: systematic review and meta-analysis, Journal of Neurosurgery, 2019, Vol. 132(Issue: 5), pp. 1479–1494, DOI: 10.3171/2019.2.JNS182507, PMID: 31125970,</ref>
Consequences of Altered Intracranial Pressure[edit]
When ICP is either excessively high or low, it can lead to severe neurological impairment and may become life-threatening. Increased ICP can reduce cerebral blood flow, resulting in brain ischemia and neuronal death. In contrast, decreased ICP, though less common, can lead to conditions such as spontaneous intracranial hypotension, characterized by postural headaches.<ref>,
Spontaneous low pressure, low CSF volume headaches: spontaneous CSF leaks, Headache, 2013, Vol. 53(Issue: 7), pp. 1034–1053, DOI: 10.1111/head.12149, PMID: 23808994,</ref>
Treatment Strategies for Abnormal Intracranial Pressure[edit]
The management of abnormal ICP is a critical aspect of neurocritical care. Treatment strategies for elevated ICP include sedation, hyperventilation, osmotherapy (using osmotic diuretics such as mannitol), and surgical interventions like decompressive craniectomy. On the other hand, treatments for low ICP typically involve addressing the underlying cause, such as repairing CSF leaks.<ref>,
Guidelines for the Management of Severe Traumatic Brain Injury, Fourth Edition, Neurosurgery, 2017, Vol. 80(Issue: 1), pp. 6–15, DOI: 10.1227/NEU.0000000000001432, PMID: 27654000,</ref>
Conclusion[edit]
In conclusion, intracranial pressure plays a pivotal role in maintaining brain health. Careful monitoring and management of ICP are key to preventing and treating various neurological disorders.
References[edit]
<references />
See Also[edit]
- Monro-Kellie doctrine
- Cerebral blood flow
- Brain ischemia
- Spontaneous intracranial hypotension
- Neurocritical care
|
|
|
| Physiology of the nervous system | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| Diseases of the nervous system, primarily CNS (G04–G47, 323–349) | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|


