Pelger–Huët anomaly
Genetic blood disorder with abnormal neutrophil nuclei
| Pelger–Huët anomaly | |
|---|---|
| Hypogranular neutrophil with a pseudo-Pelger-Huet nucleus in MDS.jpg | |
| Blood smear of a patient with myelodysplastic syndrome: red blood cells showing marked poikilocytosis (partly post-splenectomy) and a hypogranular neutrophil with a pseudo-Pelger–Huët nucleus. | |
| Synonyms | PHA, Pelger anomaly, Huët anomaly |
| Pronunciation | nl
|
| Complications | Generally benign in heterozygotes; potential immune dysfunction in homozygotes |
| Usual onset | Congenital |
| Duration | Lifelong |
| Types | Congenital Pelger–Huët anomaly, Pseudo–Pelger–Huët anomaly |
| Causes | Mutation in the lamin B receptor (LBR) gene |
| Risk factors | Family history of the disorder |
| Diagnosis | Peripheral blood smear, genetic testing |
| Differential diagnosis | Pseudo–Pelger–Huët anomaly, Myelodysplastic syndrome |
| Prevention | None |
| Treatment | Supportive; no specific treatment needed for congenital form |
| Medication | None |
| Prognosis | Excellent for heterozygous congenital form |
| Frequency | Rare |
| Deaths | None (for congenital form) |
Pelger–Huët anomaly (PHA) is a rare, benign genetic disorder affecting the white blood cells, primarily the neutrophils and eosinophils. It is classified as a type of laminopathy and results from mutations in the lamin B receptor (LBR) gene. The hallmark of PHA is the abnormal shape of the cell nucleus, which typically appears as bilobed, peanut-shaped, or dumbbell-shaped, rather than the usual multi-lobed (trilobed) configuration.
History[edit]
The condition was first described in 1928 by Dutch hematologist Karel Pelger, who noted the distinctive appearance of neutrophil nuclei. In 1931, Gauthier Jean Huët, a Dutch pediatrician, recognized the hereditary nature of this anomaly, leading to the eponymous naming of the disorder.
Pathophysiology[edit]
The lamin B receptor gene, located on chromosome 1q42.1, encodes an inner nuclear membrane protein involved in chromatin organization and nuclear envelope stability. Mutations in this gene disrupt the terminal differentiation of neutrophils, leading to characteristic nuclear hyposegmentation.
Genetics[edit]
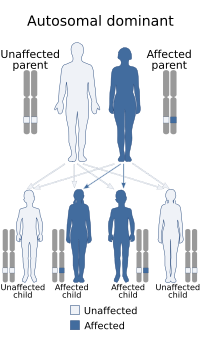
Pelger–Huët anomaly is inherited in an autosomal dominant pattern:
- Heterozygotes exhibit typical bilobed or hyposegmented nuclei in neutrophils but are clinically asymptomatic.
- Homozygotes may present with more pronounced nuclear abnormalities and can have mild hematological dysfunction, including altered neutrophil mobility and impaired chemotaxis.
Types[edit]
Congenital Pelger–Huët anomaly[edit]
The congenital form is inherited and considered benign. It is not associated with illness or increased susceptibility to infection in heterozygous carriers. The neutrophils in these individuals retain normal function despite abnormal nuclear morphology.
Pseudo–Pelger–Huët anomaly[edit]
This is an acquired form and may occur in association with:
- Myelodysplastic syndrome (MDS)
- Acute myeloid leukemia (AML)
- Chronic myelogenous leukemia (CML)
- HIV/AIDS
- After exposure to certain medications (e.g., chemotherapeutic agents, immunosuppressants)
This form can be an indicator of serious underlying pathology and requires further investigation.
Diagnosis[edit]
Diagnosis of Pelger–Huët anomaly includes:
- **Peripheral blood smear**: Neutrophils with bilobed or round nuclei and dense clumped chromatin.
- **Genetic testing**: Confirmation of LBR gene mutation if necessary.
- **Family history**: Important to distinguish congenital from acquired forms.
Differential diagnosis[edit]
- Pseudo–Pelger–Huët anomaly due to underlying hematologic disease
- Neutrophil dysplasia in myelodysplastic syndromes
- Left shift in infection or stress
Clinical significance[edit]
While Pelger–Huët anomaly is largely benign in congenital form, it is crucial to distinguish it from its pseudo-form to avoid misdiagnosis. Misinterpretation as immature granulocytes can lead to inappropriate clinical management.
Management[edit]
No treatment is required for the congenital form. Recognition of the anomaly prevents unnecessary diagnostic testing or treatment.
For the acquired (pseudo) form, management involves addressing the underlying disease or discontinuing the causative medication.
See also[edit]
External links[edit]
| Abnormal clinical and laboratory findings for blood tests (ICD-10 R70–R79, ICD-9 780–799) | ||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian