Angiomyolipoma

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Angiomyolipoma | |
|---|---|

| |
| Synonyms | Renal angiomyolipoma |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Often asymptomatic, possible abdominal pain, hematuria, or palpable mass |
| Complications | Retroperitoneal hemorrhage, renal failure |
| Onset | Typically in adulthood |
| Duration | Chronic |
| Types | Sporadic, associated with tuberous sclerosis complex |
| Causes | Genetic mutations, often associated with TSC1 or TSC2 genes |
| Risks | Tuberous sclerosis, female gender, pregnancy |
| Diagnosis | Ultrasound, CT scan, MRI |
| Differential diagnosis | Renal cell carcinoma, oncocytoma, liposarcoma |
| Prevention | None known |
| Treatment | Embolization, surgical resection, mTOR inhibitors |
| Medication | Sirolimus, everolimus |
| Prognosis | Generally good, but depends on size and symptoms |
| Frequency | Rare, but more common in patients with tuberous sclerosis |
| Deaths | N/A |
A benign tumor of the kidney
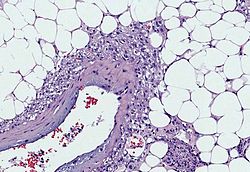

An angiomyolipoma is a benign tumor that is most commonly found in the kidney. It is composed of blood vessels, smooth muscle, and adipose tissue. Although angiomyolipomas are generally benign, they can sometimes lead to complications, particularly if they grow large or if they are associated with certain genetic conditions.
Pathophysiology[edit]
Angiomyolipomas are classified as hamartomas, which are benign, tumor-like malformations made up of an abnormal mixture of cells and tissues normally found in the area of the body where the growth occurs. The tumor is composed of three types of tissue: thick-walled blood vessels, smooth muscle cells, and fat cells. The presence of these components gives the tumor its name: "angio" refers to blood vessels, "myo" to muscle, and "lipoma" to fat.
Epidemiology[edit]
Angiomyolipomas are relatively rare, with an estimated prevalence of 0.3% to 3% in the general population. They are more common in women than in men and are often discovered incidentally during imaging studies for other conditions. Angiomyolipomas are also associated with tuberous sclerosis complex (TSC), a genetic disorder that causes non-malignant tumors to form in many different organs.
Clinical Presentation[edit]
Most angiomyolipomas are asymptomatic and are found incidentally during imaging studies such as ultrasound, CT scan, or MRI. However, larger tumors can cause symptoms such as flank pain, hematuria (blood in the urine), or even life-threatening retroperitoneal hemorrhage if they rupture. In patients with tuberous sclerosis, multiple angiomyolipomas may be present, and they may grow larger and cause more significant symptoms.
Diagnosis[edit]
The diagnosis of angiomyolipoma is typically made through imaging studies. On ultrasound, angiomyolipomas appear as echogenic (bright) lesions due to their high fat content. CT scans can confirm the presence of fat within the tumor, which is a key diagnostic feature. MRI can also be used to characterize the lesion and assess its composition.
Management[edit]
The management of angiomyolipoma depends on the size of the tumor and the presence of symptoms. Small, asymptomatic tumors may be monitored with periodic imaging studies. Larger tumors, or those causing symptoms, may require intervention. Options include embolization to reduce blood supply to the tumor, surgical resection, or nephron-sparing surgery. In some cases, mTOR inhibitors such as everolimus may be used, particularly in patients with tuberous sclerosis.
Prognosis[edit]
The prognosis for patients with angiomyolipoma is generally excellent, especially for those with small, asymptomatic tumors. However, larger tumors or those associated with tuberous sclerosis may require ongoing management to prevent complications.
Related pages[edit]
External links[edit]
| Tumors of the urinary and genital systems | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian