Dengue fever: Difference between revisions
No edit summary |
CSV import |
||
| Line 1: | Line 1: | ||
{{SI}} | |||
{{Infobox medical condition | |||
| name = Dengue fever | |||
| image = [[File:Denguerash.JPG|alt=Rash caused by dengue fever]] | |||
| caption = Rash caused by dengue fever | |||
| field = [[Infectious disease]] | |||
| synonyms = Breakbone fever, dandy fever | |||
| symptoms = [[Fever]], [[headache]], [[muscle pain]], [[joint pain]], [[skin rash]] | |||
| complications = [[Dengue hemorrhagic fever]], [[dengue shock syndrome]] | |||
| onset = 4–10 days after exposure | |||
| duration = 2–7 days | |||
| causes = [[Dengue virus]] spread by [[Aedes mosquito]] | |||
| risks = Living or traveling in tropical areas | |||
| diagnosis = [[Blood test]] | |||
| prevention = [[Mosquito control]], [[vaccine]] | |||
| treatment = Supportive care, [[intravenous fluids]], [[pain relief]] | |||
| frequency = 100–400 million cases per year | |||
| deaths = 40,000 per year | |||
}} | |||
== '''Alternate names''' == | == '''Alternate names''' == | ||
Dengue hemorrhagic fever; Dengue shock syndrome; Philippine hemorrhagic fever; Thai hemorrhagic fever; Singapore hemorrhagic fever; Hemorrhagic dengue; DF; Dengue virus infection | Dengue hemorrhagic fever; Dengue shock syndrome; Philippine hemorrhagic fever; Thai hemorrhagic fever; Singapore hemorrhagic fever; Hemorrhagic dengue; DF; Dengue virus infection | ||
== '''Definition''' == | == '''Definition''' == | ||
Dengue fever (DF), caused by dengue virus, is an arboviral disease characterized by an initial non-specific febrile illness that can sometimes progress to more severe forms manifesting capillary leakage and hemorrhage (dengue hemorrhagic fever, or DHF) and shock (dengue shock syndrome, or DSS). | Dengue fever (DF), caused by dengue virus, is an arboviral disease characterized by an initial non-specific febrile illness that can sometimes progress to more severe forms manifesting capillary leakage and hemorrhage (dengue hemorrhagic fever, or DHF) and shock (dengue shock syndrome, or DSS). | ||
[[File:Symptoms man - dengue.webm|Symptoms of Dengue|thumb]] | [[File:Symptoms man - dengue.webm|Symptoms of Dengue|left|thumb]] | ||
[[File:Dengue.jpg|Dengue|thumb]] | [[File:Dengue.jpg|Dengue|left|thumb]] | ||
<youtube> | <youtube> | ||
title='''{{PAGENAME}}''' | title='''{{PAGENAME}}''' | ||
| Line 16: | Line 33: | ||
height=600 | height=600 | ||
</youtube> | </youtube> | ||
== '''Epidemiology''' == | == '''Epidemiology''' == | ||
DF is found in the tropics worldwide, especially in Southeast Asia, the Pacific region, and the Americas, with 40% of the global population at risk. An estimated 50 to 100 million cases of DF, 500,000 hospitalizations, and 20,000 deaths occur yearly worldwide. | DF is found in the tropics worldwide, especially in Southeast Asia, the Pacific region, and the Americas, with 40% of the global population at risk. An estimated 50 to 100 million cases of DF, 500,000 hospitalizations, and 20,000 deaths occur yearly worldwide. | ||
== '''Cause''' == | == '''Cause''' == | ||
* Over 25 different viruses cause viral hemorrhagic fever. | * Over 25 different viruses cause viral hemorrhagic fever. | ||
* Dengue virus belongs to the [[Flaviviridae]] family, genus [[Flavivirus]]. Four distinct serotypes, with significant strain variation, are recognized. | * Dengue virus belongs to the [[Flaviviridae]] family, genus [[Flavivirus]]. Four distinct serotypes, with significant strain variation, are recognized. | ||
* Dengue is caused by one of any of four related viruses: Dengue virus 1, 2, 3, and 4. | * Dengue is caused by one of any of four related viruses: Dengue virus 1, 2, 3, and 4.  For this reason, a person can be infected with a dengue virus as many as four times in his or her lifetime. | ||
== '''Signs and symptoms''' == | == '''Signs and symptoms''' == | ||
* Mild symptoms of dengue can be confused with other illnesses that cause fever, aches and pains, or a rash. | * Mild symptoms of dengue can be confused with other illnesses that cause fever, aches and pains, or a rash. | ||
* Graphic of human body showing most common symptom of dengue is fever with any of the following: eye pain, headache, muscle pain, rash, bone pain, nausea/vomiting, joint pain | * Graphic of human body showing most common symptom of dengue is fever with any of the following: eye pain, headache, muscle pain, rash, bone pain, nausea/vomiting, joint pain | ||
The most common symptom of dengue is fever with any of the following: | The most common symptom of dengue is fever with any of the following: | ||
* Nausea, vomiting | * Nausea, vomiting | ||
| Line 36: | Line 48: | ||
* Any warning sign | * Any warning sign | ||
* Symptoms of dengue typically last 2–7 days. Most people will recover after about a week. | * Symptoms of dengue typically last 2–7 days. Most people will recover after about a week. | ||
== '''Transmission''' == | == '''Transmission''' == | ||
* Dengue viruses are spread to people through the bites of infected [[Aedes]] species mosquitoes ([[Aedes aegypti|Ae. aegypti]] or [[Aedes albopictus|Ae. albopictus]]). | * Dengue viruses are spread to people through the bites of infected [[Aedes]] species mosquitoes ([[Aedes aegypti|Ae. aegypti]] or [[Aedes albopictus|Ae. albopictus]]). | ||
| Line 43: | Line 54: | ||
* Mosquitoes that spread dengue, [[chikungunya]], and [[Zika virus|Zika]] bite during the day and night. | * Mosquitoes that spread dengue, [[chikungunya]], and [[Zika virus|Zika]] bite during the day and night. | ||
* Mosquitoes become infected when they bite a person infected with the virus. Infected mosquitoes can then spread the virus to other people through bites. | * Mosquitoes become infected when they bite a person infected with the virus. Infected mosquitoes can then spread the virus to other people through bites. | ||
'''From mother to child''' | '''From mother to child''' | ||
* A pregnant woman already infected with dengue can pass the virus to her fetus during pregnancy or around the time of birth. | * A pregnant woman already infected with dengue can pass the virus to her fetus during pregnancy or around the time of birth. | ||
| Line 49: | Line 59: | ||
* Because of the benefits of breastfeeding, mothers are encouraged to breastfeed even in areas with risk of dengue. | * Because of the benefits of breastfeeding, mothers are encouraged to breastfeed even in areas with risk of dengue. | ||
* Dengue in pregnancy | * Dengue in pregnancy | ||
* Rarely, dengue can be spread through blood transfusion, organ transplant, or through a needle stick injury. | * Rarely, dengue can be spread through blood transfusion, organ transplant, or through a needle stick injury. | ||
== '''Diagnosis''' == | == '''Diagnosis''' == | ||
Most state health departments and many commercial laboratories perform dengue diagnostic testing. | Most state health departments and many commercial laboratories perform dengue diagnostic testing. | ||
'''[[Nucleic acid amplification testing|Nucleic acid amplification tests]] (NAATs)''' | '''[[Nucleic acid amplification testing|Nucleic acid amplification tests]] (NAATs)''' | ||
* For patients with suspected dengue virus disease, NAATs are the preferred method of laboratory diagnosis. | * For patients with suspected dengue virus disease, NAATs are the preferred method of laboratory diagnosis. | ||
* NAATs should be performed on serum specimens collected 7 days or less after symptom onset. | * NAATs should be performed on serum specimens collected 7 days or less after symptom onset. | ||
* Laboratory confirmation can be made from a single acute-phase serum specimen obtained early ( | * Laboratory confirmation can be made from a single acute-phase serum specimen obtained early (≤7 days after fever onset) in the illness by detecting viral genomic sequences with rRT-PCR or dengue nonstructural protein 1 (NS1) antigen by immunoassay. | ||
* Presence of virus by rRT-PCR or NS1 antigen in a single diagnostic specimen is considered laboratory confirmation of dengue in patients with a compatible clinical and travel history. | * Presence of virus by rRT-PCR or NS1 antigen in a single diagnostic specimen is considered laboratory confirmation of dengue in patients with a compatible clinical and travel history. | ||
'''Serologic tests''' | '''Serologic tests''' | ||
* IgM antibody testing can identify additional infections and is an important diagnostic tool. However, interpreting the results is complicated by cross-reactivity with other [[Flavivirus|flaviviruses]], like [[Zika]], and determining the specific timing of infection can be difficult. | * IgM antibody testing can identify additional infections and is an important diagnostic tool. However, interpreting the results is complicated by cross-reactivity with other [[Flavivirus|flaviviruses]], like [[Zika]], and determining the specific timing of infection can be difficult. | ||
* Later in the illness ( | * Later in the illness (‚â•4 days after fever onset), [[IgM]] against dengue virus can be detected with MAC-[[ELISA]]. For patients presenting during the first week after fever onset, diagnostic testing should include a test for dengue virus ([[RT-PCR]] or NS1) and IgM. | ||
* For patients presenting >1 week after fever onset, IgM detection is most useful, although NS1 has been reported positive up to 12 days after fever onset . In the United States, both MAC-ELISA and RT-PCR are approved as in vitro diagnostic tests. | * For patients presenting >1 week after fever onset, IgM detection is most useful, although NS1 has been reported positive up to 12 days after fever onset . In the United States, both MAC-ELISA and RT-PCR are approved as in vitro diagnostic tests. | ||
* IgM in a single serum sample strongly suggests a recent dengue virus infection and should be presumed confirmatory for dengue if the infection occurred in a place where other potentially cross-reactive flaviviruses (such as Zika, West Nile, yellow fever, and Japanese encephalitis viruses) are not a risk. | * IgM in a single serum sample strongly suggests a recent dengue virus infection and should be presumed confirmatory for dengue if the infection occurred in a place where other potentially cross-reactive flaviviruses (such as Zika, West Nile, yellow fever, and Japanese encephalitis viruses) are not a risk. | ||
* PRNTs can resolve false-positive IgM antibody results caused by non-specific reactivity, and, in some cases, can help identify the infecting virus. However, in areas with high prevalence of dengue and Zika virus neutralizing antibodies, PRNT may not confirm a significant proportion of IgM positive results. PRNT testing is available through several state health departments and CDC. | * PRNTs can resolve false-positive IgM antibody results caused by non-specific reactivity, and, in some cases, can help identify the infecting virus. However, in areas with high prevalence of dengue and Zika virus neutralizing antibodies, PRNT may not confirm a significant proportion of IgM positive results. PRNT testing is available through several state health departments and CDC. | ||
'''Cross-reactive flaviviruses''' | '''Cross-reactive flaviviruses''' | ||
* If infection is likely to have occurred in a place where other potentially cross-reactive flaviviruses circulate, both molecular and serologic diagnostic testing for dengue and other flaviviruses should be performed. | * If infection is likely to have occurred in a place where other potentially cross-reactive flaviviruses circulate, both molecular and serologic diagnostic testing for dengue and other flaviviruses should be performed. | ||
| Line 73: | Line 78: | ||
* [[IgG]] antibody testing | * [[IgG]] antibody testing | ||
* IgG detection by ELISA in a single serum sample is not useful for diagnostic testing because it remains detectable for life after a dengue virus infection. | * IgG detection by ELISA in a single serum sample is not useful for diagnostic testing because it remains detectable for life after a dengue virus infection. | ||
== '''Treatment''' == | == '''Treatment''' == | ||
'''No treatment:''' No specific antiviral agents exist for dengue. | '''No treatment:''' No specific antiviral agents exist for dengue. | ||
| Line 80: | Line 84: | ||
* Fever should be controlled with [[acetaminophen]] and tepid sponge baths. | * Fever should be controlled with [[acetaminophen]] and tepid sponge baths. | ||
* Febrile patients should avoid mosquito bites to reduce risk of further transmission. | * Febrile patients should avoid mosquito bites to reduce risk of further transmission. | ||
'''Severe Dengue''' | '''Severe Dengue''' | ||
* For those who develop severe dengue, close observation and frequent monitoring in an intensive care unit may be required. | * For those who develop severe dengue, close observation and frequent monitoring in an intensive care unit may be required. | ||
* Prophylactic [[platelet]] transfusions in dengue patients are not beneficial and may contribute to fluid overload. | * Prophylactic [[platelet]] transfusions in dengue patients are not beneficial and may contribute to fluid overload. | ||
* Administration of [[corticosteroids]] has no demonstrated benefit and is potentially harmful to patients; corticosteroids should not be used except in the case of autoimmune-related complication (e.g., [[hemophagocytic lymphohistiocytosis]], immune [[Thrombocytopenic purpura|thrombocytopenia purpura]]). | * Administration of [[corticosteroids]] has no demonstrated benefit and is potentially harmful to patients; corticosteroids should not be used except in the case of autoimmune-related complication (e.g., [[hemophagocytic lymphohistiocytosis]], immune [[Thrombocytopenic purpura|thrombocytopenia purpura]]). | ||
== '''Prevention''' == | == '''Prevention''' == | ||
Prevent dengue by avoiding mosquito bites. | Prevent dengue by avoiding mosquito bites. | ||
Latest revision as of 18:16, 5 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Dengue fever | |
|---|---|
| Synonyms | Breakbone fever, dandy fever |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Fever, headache, muscle pain, joint pain, skin rash |
| Complications | Dengue hemorrhagic fever, dengue shock syndrome |
| Onset | 4–10 days after exposure |
| Duration | 2–7 days |
| Types | N/A |
| Causes | Dengue virus spread by Aedes mosquito |
| Risks | Living or traveling in tropical areas |
| Diagnosis | Blood test |
| Differential diagnosis | N/A |
| Prevention | Mosquito control, vaccine |
| Treatment | Supportive care, intravenous fluids, pain relief |
| Medication | N/A |
| Prognosis | N/A |
| Frequency | 100–400 million cases per year |
| Deaths | 40,000 per year |
Alternate names[edit]
Dengue hemorrhagic fever; Dengue shock syndrome; Philippine hemorrhagic fever; Thai hemorrhagic fever; Singapore hemorrhagic fever; Hemorrhagic dengue; DF; Dengue virus infection
Definition[edit]
Dengue fever (DF), caused by dengue virus, is an arboviral disease characterized by an initial non-specific febrile illness that can sometimes progress to more severe forms manifesting capillary leakage and hemorrhage (dengue hemorrhagic fever, or DHF) and shock (dengue shock syndrome, or DSS). File:Symptoms man - dengue.webm
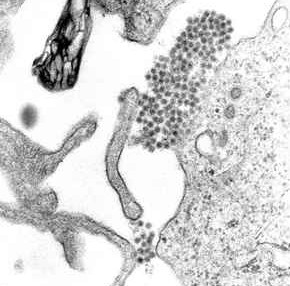
Epidemiology[edit]
DF is found in the tropics worldwide, especially in Southeast Asia, the Pacific region, and the Americas, with 40% of the global population at risk. An estimated 50 to 100 million cases of DF, 500,000 hospitalizations, and 20,000 deaths occur yearly worldwide.
Cause[edit]
- Over 25 different viruses cause viral hemorrhagic fever.
- Dengue virus belongs to the Flaviviridae family, genus Flavivirus. Four distinct serotypes, with significant strain variation, are recognized.
- Dengue is caused by one of any of four related viruses: Dengue virus 1, 2, 3, and 4.  For this reason, a person can be infected with a dengue virus as many as four times in his or her lifetime.
Signs and symptoms[edit]
- Mild symptoms of dengue can be confused with other illnesses that cause fever, aches and pains, or a rash.
- Graphic of human body showing most common symptom of dengue is fever with any of the following: eye pain, headache, muscle pain, rash, bone pain, nausea/vomiting, joint pain
The most common symptom of dengue is fever with any of the following:
- Nausea, vomiting
- Rash
- Aches and pains (eye pain, typically behind the eyes, muscle, joint, or bone pain)
- Any warning sign
- Symptoms of dengue typically last 2–7 days. Most people will recover after about a week.
Transmission[edit]
- Dengue viruses are spread to people through the bites of infected Aedes species mosquitoes (Ae. aegypti or Ae. albopictus).
- These mosquitoes typically lay eggs near standing water in containers that hold water, like buckets, bowls, animal dishes, flower pots, and vases.
- These mosquitoes prefer to bite people, and live both indoors and outdoors near people.
- Mosquitoes that spread dengue, chikungunya, and Zika bite during the day and night.
- Mosquitoes become infected when they bite a person infected with the virus. Infected mosquitoes can then spread the virus to other people through bites.
From mother to child
- A pregnant woman already infected with dengue can pass the virus to her fetus during pregnancy or around the time of birth.
- To date, there has been one documented report of dengue spread through breast milk.
- Because of the benefits of breastfeeding, mothers are encouraged to breastfeed even in areas with risk of dengue.
- Dengue in pregnancy
- Rarely, dengue can be spread through blood transfusion, organ transplant, or through a needle stick injury.
Diagnosis[edit]
Most state health departments and many commercial laboratories perform dengue diagnostic testing. Nucleic acid amplification tests (NAATs)
- For patients with suspected dengue virus disease, NAATs are the preferred method of laboratory diagnosis.
- NAATs should be performed on serum specimens collected 7 days or less after symptom onset.
- Laboratory confirmation can be made from a single acute-phase serum specimen obtained early (≤7 days after fever onset) in the illness by detecting viral genomic sequences with rRT-PCR or dengue nonstructural protein 1 (NS1) antigen by immunoassay.
- Presence of virus by rRT-PCR or NS1 antigen in a single diagnostic specimen is considered laboratory confirmation of dengue in patients with a compatible clinical and travel history.
Serologic tests
- IgM antibody testing can identify additional infections and is an important diagnostic tool. However, interpreting the results is complicated by cross-reactivity with other flaviviruses, like Zika, and determining the specific timing of infection can be difficult.
- Later in the illness (‚â•4 days after fever onset), IgM against dengue virus can be detected with MAC-ELISA. For patients presenting during the first week after fever onset, diagnostic testing should include a test for dengue virus (RT-PCR or NS1) and IgM.
- For patients presenting >1 week after fever onset, IgM detection is most useful, although NS1 has been reported positive up to 12 days after fever onset . In the United States, both MAC-ELISA and RT-PCR are approved as in vitro diagnostic tests.
- IgM in a single serum sample strongly suggests a recent dengue virus infection and should be presumed confirmatory for dengue if the infection occurred in a place where other potentially cross-reactive flaviviruses (such as Zika, West Nile, yellow fever, and Japanese encephalitis viruses) are not a risk.
- PRNTs can resolve false-positive IgM antibody results caused by non-specific reactivity, and, in some cases, can help identify the infecting virus. However, in areas with high prevalence of dengue and Zika virus neutralizing antibodies, PRNT may not confirm a significant proportion of IgM positive results. PRNT testing is available through several state health departments and CDC.
Cross-reactive flaviviruses
- If infection is likely to have occurred in a place where other potentially cross-reactive flaviviruses circulate, both molecular and serologic diagnostic testing for dengue and other flaviviruses should be performed.
- People infected with or vaccinated against other flaviviruses (such as yellow fever or Japanese encephalitis) may produce cross-reactive flavivirus antibodies, yielding false-positive serologic dengue diagnostic test results.
- IgG antibody testing
- IgG detection by ELISA in a single serum sample is not useful for diagnostic testing because it remains detectable for life after a dengue virus infection.
Treatment[edit]
No treatment: No specific antiviral agents exist for dengue. Supportive care is advised:
- Patients should be advised to stay well hydrated and to avoid aspirin (acetylsalicylic acid), aspirin-containing drugs, and other nonsteroidal anti-inflammatory drugs (such as ibuprofen) because of their anticoagulant properties.
- Fever should be controlled with acetaminophen and tepid sponge baths.
- Febrile patients should avoid mosquito bites to reduce risk of further transmission.
Severe Dengue
- For those who develop severe dengue, close observation and frequent monitoring in an intensive care unit may be required.
- Prophylactic platelet transfusions in dengue patients are not beneficial and may contribute to fluid overload.
- Administration of corticosteroids has no demonstrated benefit and is potentially harmful to patients; corticosteroids should not be used except in the case of autoimmune-related complication (e.g., hemophagocytic lymphohistiocytosis, immune thrombocytopenia purpura).
Prevention[edit]
Prevent dengue by avoiding mosquito bites.
- All four dengue viruses are spread primarily through the bite of an infected Aedes species (Ae. aegypti and Ae. albopictus) mosquito. These mosquitoes also spread chikungunya and Zika viruses.
- The mosquitoes that spread dengue are found in most tropical and subtropical regions of the world, including many parts of the United States.
- Ae. aegypti and Ae. albopictus bite during the day and night.
- A dengue vaccine is available for use in some parts of the world, including United States territories.
|
|
|
NIH genetic and rare disease info[edit]
Dengue fever is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Dengue fever
|


