Acromegaly: Difference between revisions
No edit summary |
No edit summary |
||
| Line 1: | Line 1: | ||
== What is | == What is [[Acromegaly]]? == | ||
Acromegaly is a disorder that occurs when | '''Acromegaly''' is a rare [[endocrine disorder]] that occurs when the body produces excessive amounts of [[growth hormone]] (GH), usually due to a [[tumor]] in the [[pituitary gland]]. This leads to the overproduction of [[insulin-like growth factor 1]] (IGF-1), a hormone that stimulates the abnormal growth of [[bones]], [[cartilage]], [[soft tissues]], and internal [[organs]]. | ||
[[File:Acromegaly prognathism.JPEG|alt=Acromegaly prognathism|thumb|'''Acromegaly prognathism''']] | |||
In adults, acromegaly develops gradually and often goes unrecognized for years. Because the [[epiphyseal plates]] have already fused after [[puberty]], the condition does not cause increased height (as in [[gigantism]]), but rather a characteristic coarsening of facial features and enlargement of the hands, feet, and other body parts. | |||
[[File:Acromegaly prognathism.JPEG|alt=Acromegaly prognathism|thumb|'''Acromegaly prognathism''': A common craniofacial manifestation of the disorder.]] | |||
== How common is acromegaly? == | == How common is acromegaly? == | ||
Acromegaly is rare | Acromegaly is a rare condition, affecting an estimated 3 to 14 out of every 100,000 individuals globally. Because of its slow progression and non-specific symptoms, many cases remain undiagnosed for years, leading to a delay in treatment. | ||
== Who is more likely to develop acromegaly? == | |||
Acromegaly is most frequently diagnosed in [[middle-aged adults]], typically between the ages of 30 and 50, although it can occur at any age. It affects both [[men]] and [[women]] equally. | |||
In [[children]] and [[adolescents]], excess GH secretion before the closure of the [[growth plates]] results in [[gigantism]] rather than acromegaly. [[Gigantism]] leads to rapid and excessive linear growth and can be associated with similar complications due to elevated IGF-1 levels. | |||
== What are the complications of acromegaly? == | == What are the complications of acromegaly? == | ||
Without proper treatment, acromegaly can lead to serious [[comorbidities]] and even premature death due to its effects on multiple body systems. | |||
[[ | |||
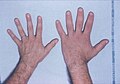
[[File:Acromegaly hands.JPEG|alt=Acromegaly hands|thumb|'''Acromegaly hands''': Soft tissue swelling and digital thickening are typical signs.]] | |||
'''Common complications include:''' | |||
* [[Type 2 diabetes mellitus]] | |||
* [[Hypertension]] (high blood pressure) | |||
* [[Cardiomyopathy]] and other forms of [[heart disease]] | |||
* [[Sleep apnea]] due to upper airway obstruction | |||
* [[Osteoarthritis]] and [[joint pain]] | |||
* [[Carpal tunnel syndrome]] | |||
* Enlargement of internal organs such as the [[heart]], [[liver]], and [[kidneys]] | |||
* Increased risk of [[colonic polyps]] and [[colorectal cancer]] | |||
Some | Some individuals may have genetic predispositions that result in [[multiple endocrine neoplasia]] or other tumor syndromes. Uncontrolled acromegaly increases [[morbidity]] and may reduce [[life expectancy]] if left untreated. | ||
However, with appropriate treatment—whether surgical, medical, or radiation therapy—GH and IGF-1 levels can be normalized, symptoms improve significantly, and [[life expectancy]] can return to near-normal levels. | |||
== What are the symptoms of acromegaly? == | == What are the symptoms of acromegaly? == | ||
Symptoms of acromegaly | Symptoms of acromegaly develop slowly and may not be noticed until years after GH overproduction begins. The condition affects both appearance and internal organ systems. | ||
* hands and feet | '''Common physical changes include:''' | ||
* | * Enlargement of [[hands]] and [[feet]] – often noticed by a change in ring or shoe size | ||
* | * Thickening of the [[skin]], which becomes coarse and oily | ||
* | * Prominent [[brow ridge]], [[prognathism]] (protruding jaw), and increased spacing between the [[teeth]] | ||
* Enlargement of the [[nose]], [[lips]], and [[tongue]] | |||
* voice | * Deepening of the [[voice]] due to [[vocal cord]] thickening | ||
* skin | * Presence of [[skin tags]] – small benign skin growths | ||
* Excessive [[sweating]] and [[body odor]] due to overactive [[sebaceous glands]] | |||
'''Other | '''Other symptoms may include:''' | ||
* Chronic [[headaches]] | |||
* [[Joint pain]] and [[arthralgia]] | |||
* [[Vision disturbances]] due to pressure on the [[optic chiasm]] | |||
* General [[fatigue]] and [[muscle weakness]] | |||
<gallery> | <gallery> | ||
File:Acromegaly hands.JPEG|alt=Acromegaly hands|'''Acromegaly hands''' | File:Acromegaly hands.JPEG|alt=Acromegaly hands|'''Acromegaly hands''' | ||
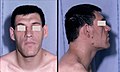
File:Acromegaly facial features.JPEG|alt=Acromegaly facial features|'''Acromegaly facial features''' | File:Acromegaly facial features.JPEG|alt=Acromegaly facial features|'''Acromegaly facial features''' | ||
File:Annals of surgery (1885) (14776157562).jpg|alt= | File:Annals of surgery (1885) (14776157562).jpg|alt=Historical illustration of acromegaly|'''Historical illustration of acromegaly''' | ||
</gallery> | </gallery> | ||
== What causes [[acromegaly]]? == | |||
Acromegaly is caused by chronic overproduction of [[growth hormone]] (GH), which in turn stimulates the liver to produce [[insulin-like growth factor 1]] (IGF-1). IGF-1 is responsible for the overgrowth of [[bones]], [[soft tissues]], and [[organs]], as well as metabolic disturbances. | |||
In over 90% of cases, the excess GH is produced by a [[pituitary adenoma]], a benign (noncancerous) [[tumor]] in the [[pituitary gland]]. These tumors may grow slowly over time, often remaining undetected until symptoms become pronounced. | |||
== Pituitary tumors == | |||
A [[pituitary adenoma]] that secretes GH is the most common cause of acromegaly. These tumors can vary in size: | |||
* '''Microadenomas''' – less than 10 mm in diameter | |||
* '''Macroadenomas''' – 10 mm or larger; more likely to compress nearby structures | |||
As the tumor enlarges, it may interfere with the function of the surrounding [[pituitary tissue]], leading to reduced production of other [[pituitary hormones]] such as: | |||
* [[Thyroid-stimulating hormone]] (TSH) – affecting [[metabolism]] | |||
* [[Adrenocorticotropic hormone]] (ACTH) – influencing [[cortisol]] levels | |||
* [[Luteinizing hormone]] (LH) and [[follicle-stimulating hormone]] (FSH) – impacting [[reproductive function]] | |||
* [[Prolactin]] – which may be overproduced, especially in tumors that co-secrete both GH and prolactin | |||
[[File:Pituitary pineal glands.jpg|alt=Pituitary and pineal glands|thumb|'''Pituitary and pineal glands''': Pituitary adenomas are the most common cause of acromegaly.]] | |||
Tumors may also compress the [[optic chiasm]], leading to: | |||
* [[ | * [[Bitemporal hemianopsia]] – loss of peripheral vision in both eyes | ||
* | * [[Headaches]] and [[nausea]] | ||
== Nonpituitary tumors == | |||
In rare cases, acromegaly is caused by tumors located outside the pituitary gland, known as '''ectopic sources''' of GH or [[growth hormone-releasing hormone]] (GHRH). These may include: | |||
* [[Pancreatic tumors]] | |||
* [[Lung tumors]] | |||
* [[Adrenal tumors]] | |||
* [[Hypothalamic hamartomas]] – in or near the [[hypothalamus]] | |||
These tumors may directly secrete GH or more commonly GHRH, which stimulates the pituitary to produce excess GH. | |||
[[ | |||
== Pathophysiology == | |||
When GH levels remain elevated over time, the liver continuously secretes IGF-1, leading to: | |||
* [[Hyperplasia]] of [[cartilage]] and [[connective tissue]] | |||
* Increased [[osteoblastic activity]] and [[periosteal bone growth]] | |||
* [[Soft tissue hypertrophy]] including the [[tongue]], [[larynx]], [[heart]], and [[kidneys]] | |||
* Altered metabolism of [[lipids]] and [[glucose]], contributing to [[insulin resistance]] and [[type 2 diabetes mellitus]] | |||
The changes are gradual but progressive, eventually affecting multiple [[organ systems]]. | |||
== How do doctors diagnose acromegaly? == | == How do doctors diagnose acromegaly? == | ||
The diagnosis of acromegaly is based on clinical evaluation, hormone testing, and imaging studies. | |||
=== Blood tests === | === Blood tests === | ||
* '''[[IGF-1 test]]''' – Since GH levels fluctuate throughout the day, a more reliable marker is the measurement of IGF-1, which remains elevated in patients with acromegaly. | |||
* '''[[Oral glucose tolerance test]] (OGTT)''' – Normally, ingestion of glucose suppresses GH secretion. In acromegaly, GH levels remain elevated despite the glucose load. | |||
=== Imaging studies === | |||
* '''[[Magnetic resonance imaging]] (MRI)''' – The gold standard for identifying [[pituitary tumors]]. MRI provides high-resolution images of the [[sella turcica]] and surrounding structures. | |||
* '''[[Computed tomography]] (CT)''' – Used when MRI is contraindicated (e.g., due to metallic implants or claustrophobia). CT can also help locate nonpituitary tumors in the [[chest]], [[abdomen]], or [[pelvis]]. | |||
[[File:Acromegaly pituitary macroadenoma.JPEG|alt=Acromegaly pituitary macroadenoma|thumb|'''Pituitary macroadenoma''' on MRI – a common cause of acromegaly.]] | |||
=== Additional tests === | |||
* [[Visual field testing]] – to assess for signs of [[optic nerve]] compression | |||
* [[Hormone panel]] – to evaluate other pituitary hormone levels | |||
* [[Colonoscopy]] – due to increased risk of [[colonic polyps]] and [[colorectal cancer]] | |||
== Differential diagnosis == | |||
Conditions that may resemble acromegaly include: | |||
* [[Paget’s disease of bone]] | |||
* [[Gigantism]] (in children and adolescents) | |||
* [[Hypothyroidism]] – may cause coarse features and soft tissue swelling | |||
* [[Polycystic ovary syndrome]] (PCOS) – can mimic some symptoms in women | |||
Accurate diagnosis requires correlation of clinical findings with biochemical and imaging studies. | |||
== How do doctors treat [[acromegaly]]? == | |||
Treatment for acromegaly focuses on: | |||
* Reducing or removing the tumor producing excess [[growth hormone]] | |||
* Normalizing levels of [[growth hormone]] and [[IGF-1]] | |||
* Alleviating [[symptoms]] | |||
* Preventing or managing [[complications]] | |||
The three main approaches are: | |||
* [[Surgery]] | |||
* [[Medications]] | |||
* [[Radiation therapy]] | |||
== Surgery == | |||
The first-line treatment for most cases of acromegaly caused by a [[pituitary adenoma]] is **surgical removal** of the tumor. The most commonly used approach is: | |||
=== Transsphenoidal surgery === | |||
This minimally invasive surgery involves removing the tumor through the [[nasal cavity]] and the [[sphenoid sinus]], located at the base of the skull. | |||
There are two main techniques: | |||
* **Microscopic transsphenoidal surgery** – uses a surgical microscope to guide tumor removal | |||
* **Endoscopic transsphenoidal surgery** – uses a tiny camera (endoscope) for real-time visualization | |||
[[File:Pituitary Tumor Removal.png|alt=Pituitary tumor removal|thumb|'''Transsphenoidal surgery''' is the standard method for removing pituitary adenomas.]] | |||
'''Success rates:''' | |||
* About 85% for small tumors (microadenomas) | |||
* 40–50% for larger tumors (macroadenomas) | |||
'''Potential risks:''' | |||
* [[Cerebrospinal fluid leak]] | |||
* [[Meningitis]] | |||
* [[Diabetes insipidus]] | |||
* Loss of pituitary function | |||
* [[Vision loss]] (rare) | |||
If the tumor cannot be completely removed or GH/IGF-1 levels remain elevated, further treatment with medications or repeat surgery may be required. | |||
== Medications == | |||
If surgery is not possible, not fully successful, or GH levels remain elevated, doctors may prescribe medications. These can reduce hormone levels, relieve symptoms, and shrink tumors. | |||
=== 1. Somatostatin analogs (SSAs) === | |||
These drugs mimic the action of [[somatostatin]], a hormone that suppresses GH release. | |||
Common SSAs: | |||
* [[Octreotide]] (Sandostatin®) | |||
* [[Lanreotide]] (Somatuline®) | |||
* [[Pasireotide]] (Signifor®) | |||
SSAs are typically given as long-acting injections every 4 weeks. | |||
'''Benefits:''' | |||
* Normalize GH/IGF-1 in ~60% of patients | |||
* May shrink tumor size in ~30–50% of cases | |||
'''Side effects:''' | |||
* [[Gastrointestinal]] issues – nausea, bloating, diarrhea | |||
* [[Gallstones]] | |||
* Rarely, [[hair loss]] or [[hyperglycemia]] | |||
=== 2. Dopamine agonists === | |||
These are oral medications that reduce GH secretion in some individuals. | |||
Examples: | |||
* [[Cabergoline]] | |||
* [[Bromocriptine]] | |||
'''Best for:''' | |||
* Patients with mild GH elevation | |||
* Patients with [[prolactin]]-secreting tumors (mixed adenomas) | |||
'''Side effects:''' | |||
* Nausea | |||
* [[Orthostatic hypotension]] | |||
* [[Mood changes]] | |||
=== 3. Growth hormone receptor antagonists === | |||
These drugs block GH action at the cellular level rather than decreasing GH production. | |||
Main agent: | |||
* [[Pegvisomant]] (Somavert®) | |||
Given as a daily subcutaneous injection, pegvisomant blocks GH from stimulating IGF-1 production. | |||
'''Benefits:''' | |||
* Normalizes IGF-1 in up to 90% of patients | |||
* Useful when other medications fail | |||
'''Side effects:''' | |||
* Liver function abnormalities | |||
* Does not reduce tumor size | |||
* Injection site reactions | |||
== Radiation therapy == | |||
Radiation therapy is used when surgery and medications are not fully effective. It is especially useful for residual or inoperable tumors. | |||
=== | === 1. Stereotactic radiosurgery (SRS) === | ||
* Delivers highly focused radiation in a single session | |||
* Minimal damage to surrounding tissue | |||
* Examples include Gamma Knife® or CyberKnife® | |||
* [[''' | === 2. Fractionated radiotherapy === | ||
* [[ | * Small doses delivered over several weeks | ||
* Used for large tumors or those close to [[optic structures]] | |||
[[File:Gamma Knife Graphic.jpg|Gamma Knife Graphic|thumb]] | |||
'''Considerations:''' | |||
* Slow onset – takes months to years for full effect | |||
* Up to 50% of patients may eventually need [[hormone replacement therapy]] | |||
* Rare risks include [[vision problems]], [[cognitive decline]], and secondary [[tumor formation]] | |||
== Post-treatment follow-up == | |||
After treatment, patients require: | |||
= | * Regular measurement of [[GH]] and [[IGF-1]] levels | ||
* Periodic [[MRI]] to monitor for tumor recurrence | |||
* Monitoring for [[pituitary insufficiency]] | |||
* Screening for [[cardiovascular disease]], [[diabetes]], and [[colon cancer]] | |||
Effective treatment and monitoring can significantly reduce complications and restore normal [[life expectancy]]. | |||
== What is the long-term outlook for people with [[acromegaly]]? == | |||
The prognosis for individuals with acromegaly has improved significantly with earlier diagnosis and advances in treatment. When diagnosed and treated effectively, many patients can achieve normal [[growth hormone]] and [[IGF-1]] levels, with substantial reduction in symptoms and improvement in [[quality of life]]. | |||
'''Without treatment''', acromegaly can result in: | |||
* Progressive [[organ enlargement]] | |||
* Severe [[cardiovascular complications]] | |||
* [[Sleep apnea]] | |||
* [[Arthropathy]] and [[mobility impairment]] | |||
* Increased risk of [[colon cancer]] and [[endocrine tumors]] | |||
* Reduced [[life expectancy]] by 5–10 years | |||
'''With treatment''', especially if started early: | |||
* Life expectancy often returns to normal | |||
* Symptoms such as [[headaches]], [[joint pain]], and [[soft tissue swelling]] typically improve | |||
* Secondary health risks, like [[diabetes mellitus]] and [[hypertension]], can be better managed | |||
== Are there genetic causes of acromegaly? == | |||
Most cases of acromegaly are sporadic, but some are linked to **genetic syndromes** involving mutations in specific genes: | |||
''' | * '''[[MEN1 gene]]''' – associated with [[Multiple Endocrine Neoplasia type 1]] | ||
* '''[[AIP gene]]''' – mutations found in familial isolated pituitary adenoma (FIPA) | |||
* '''[[GNAS gene]]''' – involved in McCune-Albright syndrome, which can feature GH-secreting tumors | |||
* '''X-linked acrogigantism (X-LAG) syndrome''' – caused by microduplications involving the [[GPR101]] gene | |||
In individuals diagnosed at a young age or with a family history of pituitary tumors, genetic counseling and testing may be appropriate. | |||
== How is acromegaly managed over time? == | |||
Lifelong monitoring is essential, even after successful treatment. Management includes: | |||
''' | '''Regular evaluations:''' | ||
[[ | * GH and IGF-1 blood tests every 6–12 months | ||
* [[Pituitary MRI]] to check for tumor recurrence | |||
* Periodic testing for [[diabetes]], [[hypertension]], and [[hyperlipidemia]] | |||
* [[Colonoscopy]] screening as recommended | |||
''' | '''Supportive care:''' | ||
* [[Endocrinologist]] supervision | |||
* [[Nutrition counseling]] for metabolic control | |||
* Treatment of joint pain, sleep apnea, or hormonal deficiencies as needed | |||
== Living with acromegaly == | |||
People with acromegaly may experience physical and emotional challenges due to changes in appearance, chronic pain, or fatigue. Support strategies include: | |||
* Joining [[patient support groups]] | |||
* Access to [[mental health services]] and [[counseling]] | |||
* Occupational therapy for joint and hand issues | |||
* Managing work/life adjustments due to symptoms | |||
Educating patients and families helps reduce stigma and encourages adherence to long-term management plans. | |||
== Current research and future directions == | |||
Research in acromegaly is ongoing, with promising developments in: | |||
* Long-acting oral [[somatostatin analogs]] | |||
* New [[GH receptor antagonists]] with improved side-effect profiles | |||
* Genetic therapies targeting tumor pathways | |||
* Personalized medicine using GH and IGF-1 response predictors | |||
* Improved imaging techniques for microadenoma detection | |||
* Quality-of-life metrics and psychosocial impact studies | |||
== Educational and cultural references == | |||
The condition has been portrayed in media and medical literature. Notable individuals with acromegaly include: | |||
* '''[[André the Giant]]''' – professional wrestler and actor | |||
* Historical illustrations in the '''Annals of Surgery''' and writings by early endocrinologists | |||
These portrayals have helped raise awareness of acromegaly's impact and fostered public interest in pituitary disorders. | |||
== See also == | |||
* [[Gigantism]] | |||
* [[Pituitary gland]] | |||
* [[Endocrinology]] | |||
* [[Growth hormone]] | |||
* [[Insulin-like growth factor 1]] | |||
* [[Hypothalamic–pituitary–adrenal axis]] | |||
* [[Multiple endocrine neoplasia]] | |||
* [[Neuroendocrinology]] | |||
{{stub}} | {{stub}} | ||
{{Pituitary disease}} | {{Pituitary disease}} | ||
| Line 155: | Line 327: | ||
[[Category:Neuroendocrinology]] | [[Category:Neuroendocrinology]] | ||
[[Category:Pituitary disorders]] | [[Category:Pituitary disorders]] | ||
[[Category:Rare diseases]] | |||
[[Category:Hormonal disorders]] | |||
[[Category:RTT]] | [[Category:RTT]] | ||
[[Category:RTTNEURO]] | [[Category:RTTNEURO]] | ||
Revision as of 03:35, 26 March 2025
What is Acromegaly?
Acromegaly is a rare endocrine disorder that occurs when the body produces excessive amounts of growth hormone (GH), usually due to a tumor in the pituitary gland. This leads to the overproduction of insulin-like growth factor 1 (IGF-1), a hormone that stimulates the abnormal growth of bones, cartilage, soft tissues, and internal organs.
In adults, acromegaly develops gradually and often goes unrecognized for years. Because the epiphyseal plates have already fused after puberty, the condition does not cause increased height (as in gigantism), but rather a characteristic coarsening of facial features and enlargement of the hands, feet, and other body parts.

How common is acromegaly?
Acromegaly is a rare condition, affecting an estimated 3 to 14 out of every 100,000 individuals globally. Because of its slow progression and non-specific symptoms, many cases remain undiagnosed for years, leading to a delay in treatment.
Who is more likely to develop acromegaly?
Acromegaly is most frequently diagnosed in middle-aged adults, typically between the ages of 30 and 50, although it can occur at any age. It affects both men and women equally.
In children and adolescents, excess GH secretion before the closure of the growth plates results in gigantism rather than acromegaly. Gigantism leads to rapid and excessive linear growth and can be associated with similar complications due to elevated IGF-1 levels.
What are the complications of acromegaly?
Without proper treatment, acromegaly can lead to serious comorbidities and even premature death due to its effects on multiple body systems.

Common complications include:
- Type 2 diabetes mellitus
- Hypertension (high blood pressure)
- Cardiomyopathy and other forms of heart disease
- Sleep apnea due to upper airway obstruction
- Osteoarthritis and joint pain
- Carpal tunnel syndrome
- Enlargement of internal organs such as the heart, liver, and kidneys
- Increased risk of colonic polyps and colorectal cancer
Some individuals may have genetic predispositions that result in multiple endocrine neoplasia or other tumor syndromes. Uncontrolled acromegaly increases morbidity and may reduce life expectancy if left untreated.
However, with appropriate treatment—whether surgical, medical, or radiation therapy—GH and IGF-1 levels can be normalized, symptoms improve significantly, and life expectancy can return to near-normal levels.
What are the symptoms of acromegaly?
Symptoms of acromegaly develop slowly and may not be noticed until years after GH overproduction begins. The condition affects both appearance and internal organ systems.
Common physical changes include:
- Enlargement of hands and feet – often noticed by a change in ring or shoe size
- Thickening of the skin, which becomes coarse and oily
- Prominent brow ridge, prognathism (protruding jaw), and increased spacing between the teeth
- Enlargement of the nose, lips, and tongue
- Deepening of the voice due to vocal cord thickening
- Presence of skin tags – small benign skin growths
- Excessive sweating and body odor due to overactive sebaceous glands
Other symptoms may include:
- Chronic headaches
- Joint pain and arthralgia
- Vision disturbances due to pressure on the optic chiasm
- General fatigue and muscle weakness
-
Acromegaly hands
-
Acromegaly facial features
-
Historical illustration of acromegaly
What causes acromegaly?
Acromegaly is caused by chronic overproduction of growth hormone (GH), which in turn stimulates the liver to produce insulin-like growth factor 1 (IGF-1). IGF-1 is responsible for the overgrowth of bones, soft tissues, and organs, as well as metabolic disturbances.
In over 90% of cases, the excess GH is produced by a pituitary adenoma, a benign (noncancerous) tumor in the pituitary gland. These tumors may grow slowly over time, often remaining undetected until symptoms become pronounced.
Pituitary tumors
A pituitary adenoma that secretes GH is the most common cause of acromegaly. These tumors can vary in size:
- Microadenomas – less than 10 mm in diameter
- Macroadenomas – 10 mm or larger; more likely to compress nearby structures
As the tumor enlarges, it may interfere with the function of the surrounding pituitary tissue, leading to reduced production of other pituitary hormones such as:
- Thyroid-stimulating hormone (TSH) – affecting metabolism
- Adrenocorticotropic hormone (ACTH) – influencing cortisol levels
- Luteinizing hormone (LH) and follicle-stimulating hormone (FSH) – impacting reproductive function
- Prolactin – which may be overproduced, especially in tumors that co-secrete both GH and prolactin

Tumors may also compress the optic chiasm, leading to:
- Bitemporal hemianopsia – loss of peripheral vision in both eyes
- Headaches and nausea
Nonpituitary tumors
In rare cases, acromegaly is caused by tumors located outside the pituitary gland, known as ectopic sources of GH or growth hormone-releasing hormone (GHRH). These may include:
- Pancreatic tumors
- Lung tumors
- Adrenal tumors
- Hypothalamic hamartomas – in or near the hypothalamus
These tumors may directly secrete GH or more commonly GHRH, which stimulates the pituitary to produce excess GH.
Pathophysiology
When GH levels remain elevated over time, the liver continuously secretes IGF-1, leading to:
- Hyperplasia of cartilage and connective tissue
- Increased osteoblastic activity and periosteal bone growth
- Soft tissue hypertrophy including the tongue, larynx, heart, and kidneys
- Altered metabolism of lipids and glucose, contributing to insulin resistance and type 2 diabetes mellitus
The changes are gradual but progressive, eventually affecting multiple organ systems.
How do doctors diagnose acromegaly?
The diagnosis of acromegaly is based on clinical evaluation, hormone testing, and imaging studies.
Blood tests
- IGF-1 test – Since GH levels fluctuate throughout the day, a more reliable marker is the measurement of IGF-1, which remains elevated in patients with acromegaly.
- Oral glucose tolerance test (OGTT) – Normally, ingestion of glucose suppresses GH secretion. In acromegaly, GH levels remain elevated despite the glucose load.
Imaging studies
- Magnetic resonance imaging (MRI) – The gold standard for identifying pituitary tumors. MRI provides high-resolution images of the sella turcica and surrounding structures.
- Computed tomography (CT) – Used when MRI is contraindicated (e.g., due to metallic implants or claustrophobia). CT can also help locate nonpituitary tumors in the chest, abdomen, or pelvis.

Additional tests
- Visual field testing – to assess for signs of optic nerve compression
- Hormone panel – to evaluate other pituitary hormone levels
- Colonoscopy – due to increased risk of colonic polyps and colorectal cancer
Differential diagnosis
Conditions that may resemble acromegaly include:
- Paget’s disease of bone
- Gigantism (in children and adolescents)
- Hypothyroidism – may cause coarse features and soft tissue swelling
- Polycystic ovary syndrome (PCOS) – can mimic some symptoms in women
Accurate diagnosis requires correlation of clinical findings with biochemical and imaging studies.
How do doctors treat acromegaly?
Treatment for acromegaly focuses on:
- Reducing or removing the tumor producing excess growth hormone
- Normalizing levels of growth hormone and IGF-1
- Alleviating symptoms
- Preventing or managing complications
The three main approaches are:
Surgery
The first-line treatment for most cases of acromegaly caused by a pituitary adenoma is **surgical removal** of the tumor. The most commonly used approach is:
Transsphenoidal surgery
This minimally invasive surgery involves removing the tumor through the nasal cavity and the sphenoid sinus, located at the base of the skull.
There are two main techniques:
- **Microscopic transsphenoidal surgery** – uses a surgical microscope to guide tumor removal
- **Endoscopic transsphenoidal surgery** – uses a tiny camera (endoscope) for real-time visualization

Success rates:
- About 85% for small tumors (microadenomas)
- 40–50% for larger tumors (macroadenomas)
Potential risks:
- Cerebrospinal fluid leak
- Meningitis
- Diabetes insipidus
- Loss of pituitary function
- Vision loss (rare)
If the tumor cannot be completely removed or GH/IGF-1 levels remain elevated, further treatment with medications or repeat surgery may be required.
Medications
If surgery is not possible, not fully successful, or GH levels remain elevated, doctors may prescribe medications. These can reduce hormone levels, relieve symptoms, and shrink tumors.
1. Somatostatin analogs (SSAs)
These drugs mimic the action of somatostatin, a hormone that suppresses GH release.
Common SSAs:
- Octreotide (Sandostatin®)
- Lanreotide (Somatuline®)
- Pasireotide (Signifor®)
SSAs are typically given as long-acting injections every 4 weeks.
Benefits:
- Normalize GH/IGF-1 in ~60% of patients
- May shrink tumor size in ~30–50% of cases
Side effects:
- Gastrointestinal issues – nausea, bloating, diarrhea
- Gallstones
- Rarely, hair loss or hyperglycemia
2. Dopamine agonists
These are oral medications that reduce GH secretion in some individuals.
Examples:
Best for:
- Patients with mild GH elevation
- Patients with prolactin-secreting tumors (mixed adenomas)
Side effects:
3. Growth hormone receptor antagonists
These drugs block GH action at the cellular level rather than decreasing GH production.
Main agent:
- Pegvisomant (Somavert®)
Given as a daily subcutaneous injection, pegvisomant blocks GH from stimulating IGF-1 production.
Benefits:
- Normalizes IGF-1 in up to 90% of patients
- Useful when other medications fail
Side effects:
- Liver function abnormalities
- Does not reduce tumor size
- Injection site reactions
Radiation therapy
Radiation therapy is used when surgery and medications are not fully effective. It is especially useful for residual or inoperable tumors.
1. Stereotactic radiosurgery (SRS)
- Delivers highly focused radiation in a single session
- Minimal damage to surrounding tissue
- Examples include Gamma Knife® or CyberKnife®
2. Fractionated radiotherapy
- Small doses delivered over several weeks
- Used for large tumors or those close to optic structures

Considerations:
- Slow onset – takes months to years for full effect
- Up to 50% of patients may eventually need hormone replacement therapy
- Rare risks include vision problems, cognitive decline, and secondary tumor formation
Post-treatment follow-up
After treatment, patients require:
- Regular measurement of GH and IGF-1 levels
- Periodic MRI to monitor for tumor recurrence
- Monitoring for pituitary insufficiency
- Screening for cardiovascular disease, diabetes, and colon cancer
Effective treatment and monitoring can significantly reduce complications and restore normal life expectancy.
What is the long-term outlook for people with acromegaly?
The prognosis for individuals with acromegaly has improved significantly with earlier diagnosis and advances in treatment. When diagnosed and treated effectively, many patients can achieve normal growth hormone and IGF-1 levels, with substantial reduction in symptoms and improvement in quality of life.
Without treatment, acromegaly can result in:
- Progressive organ enlargement
- Severe cardiovascular complications
- Sleep apnea
- Arthropathy and mobility impairment
- Increased risk of colon cancer and endocrine tumors
- Reduced life expectancy by 5–10 years
With treatment, especially if started early:
- Life expectancy often returns to normal
- Symptoms such as headaches, joint pain, and soft tissue swelling typically improve
- Secondary health risks, like diabetes mellitus and hypertension, can be better managed
Are there genetic causes of acromegaly?
Most cases of acromegaly are sporadic, but some are linked to **genetic syndromes** involving mutations in specific genes:
- MEN1 gene – associated with Multiple Endocrine Neoplasia type 1
- AIP gene – mutations found in familial isolated pituitary adenoma (FIPA)
- GNAS gene – involved in McCune-Albright syndrome, which can feature GH-secreting tumors
- X-linked acrogigantism (X-LAG) syndrome – caused by microduplications involving the GPR101 gene
In individuals diagnosed at a young age or with a family history of pituitary tumors, genetic counseling and testing may be appropriate.
How is acromegaly managed over time?
Lifelong monitoring is essential, even after successful treatment. Management includes:
Regular evaluations:
- GH and IGF-1 blood tests every 6–12 months
- Pituitary MRI to check for tumor recurrence
- Periodic testing for diabetes, hypertension, and hyperlipidemia
- Colonoscopy screening as recommended
Supportive care:
- Endocrinologist supervision
- Nutrition counseling for metabolic control
- Treatment of joint pain, sleep apnea, or hormonal deficiencies as needed
Living with acromegaly
People with acromegaly may experience physical and emotional challenges due to changes in appearance, chronic pain, or fatigue. Support strategies include:
- Joining patient support groups
- Access to mental health services and counseling
- Occupational therapy for joint and hand issues
- Managing work/life adjustments due to symptoms
Educating patients and families helps reduce stigma and encourages adherence to long-term management plans.
Current research and future directions
Research in acromegaly is ongoing, with promising developments in:
- Long-acting oral somatostatin analogs
- New GH receptor antagonists with improved side-effect profiles
- Genetic therapies targeting tumor pathways
- Personalized medicine using GH and IGF-1 response predictors
- Improved imaging techniques for microadenoma detection
- Quality-of-life metrics and psychosocial impact studies
Educational and cultural references
The condition has been portrayed in media and medical literature. Notable individuals with acromegaly include:
- André the Giant – professional wrestler and actor
- Historical illustrations in the Annals of Surgery and writings by early endocrinologists
These portrayals have helped raise awareness of acromegaly's impact and fostered public interest in pituitary disorders.
See also
- Gigantism
- Pituitary gland
- Endocrinology
- Growth hormone
- Insulin-like growth factor 1
- Hypothalamic–pituitary–adrenal axis
- Multiple endocrine neoplasia
- Neuroendocrinology
|
|
|
| Pituitary disease | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|