Prune belly syndrome

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Prune belly syndrome | |
|---|---|
| |
| Synonyms | Eagle-Barrett syndrome, triad syndrome |
| Pronounce | |
| Specialty | Pediatrics, Urology |
| Symptoms | Abdominal muscle deficiency, urinary tract abnormalities, cryptorchidism |
| Complications | Urinary tract infection, chronic kidney disease, respiratory distress |
| Onset | Congenital |
| Duration | Lifelong |
| Types | N/A |
| Causes | Unknown, possibly genetic |
| Risks | Male sex, family history |
| Diagnosis | Ultrasound, X-ray, MRI |
| Differential diagnosis | Posterior urethral valves, Megacystis microcolon intestinal hypoperistalsis syndrome |
| Prevention | None |
| Treatment | Surgery, antibiotics, dialysis |
| Medication | Antibiotics |
| Prognosis | Variable, depends on severity |
| Frequency | 1 in 30,000 to 40,000 births |
| Deaths | |
Prune Belly Syndrome (PBS), also known as Eagle-Barrett syndrome, is a rare congenital disorder characterized by a triad of symptoms: a deficiency or absence of abdominal muscles, undescended testicles (cryptorchidism) in males, and urinary tract abnormalities. The syndrome primarily affects males, with a male-to-female ratio of approximately 20:1.
Signs and Symptoms[edit]
The primary features of Prune Belly Syndrome include:
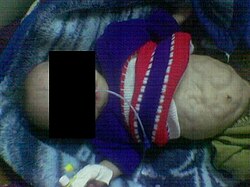
- Abdominal muscle deficiency: The absence or severe underdevelopment of abdominal muscles leads to a wrinkled appearance of the abdomen, resembling a prune, hence the name.
- Cryptorchidism: In males, the testicles fail to descend into the scrotum.
- Urinary tract abnormalities: These can include dilation of the ureters (megaureter), bladder, and urethra, leading to urinary tract infections and potential kidney damage.
Other associated symptoms may include:
- Pulmonary hypoplasia
- Gastrointestinal malformations
- Musculoskeletal abnormalities
Causes[edit]
The exact cause of Prune Belly Syndrome is not well understood. It is believed to result from a combination of genetic and environmental factors. Some cases have been linked to mutations in the CHRM3 gene, which plays a role in the development of the urinary tract.
Diagnosis[edit]
Diagnosis of Prune Belly Syndrome is typically made through a combination of prenatal ultrasound and postnatal physical examination. Prenatal ultrasound may reveal characteristic features such as a distended bladder and lack of abdominal muscles. Postnatal diagnosis involves a thorough physical examination and imaging studies such as ultrasound, X-ray, and MRI to assess the extent of urinary tract abnormalities.
Treatment[edit]
Treatment for Prune Belly Syndrome is tailored to the individual and may involve:
- Surgical correction of abdominal wall defects
- Orchiopexy to address cryptorchidism
- Management of urinary tract abnormalities, which may include surgical intervention to correct obstructions or reflux, and antibiotic prophylaxis to prevent infections
Prognosis[edit]
The prognosis for individuals with Prune Belly Syndrome varies widely depending on the severity of the condition and the presence of associated anomalies. Early diagnosis and appropriate management can improve outcomes, but some individuals may experience chronic kidney disease or other long-term complications.
See also[edit]
| Congenital malformations and deformations of musculoskeletal system / musculoskeletal abnormality | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Ad. Transform your life with W8MD's
GLP-1 weight loss injections special from $29.99 with insurance
|
WikiMD Medical Encyclopedia |
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian
