Bronchopulmonary dysplasia
Bronchopulmonary dysplasia (BPD; formerly chronic lung disease of infancy) is a chronic lung disease in which premature infants, usually those who were treated with supplemental oxygen, require long-term oxygen.<ref>Merck Manual, Professional Edition, Bronchopulmonary Dysplasia (BPD).</ref>The alveoli that are present tend to not be mature enough to function normal.<ref>
Bronchopulmonary Dysplasia(link). American Lung Association.
Accessed 2020-03-12.
</ref> It is more common in infants with low birth weight (LBW) and those who receive prolonged mechanical ventilation to treat respiratory distress syndrome (RDS). It results in significant morbidity and mortality. The definition of BPD has continued to evolve primarily due to changes in the population, such as more survivors at earlier gestational ages, and improved neonatal management including surfactant, antenatal glucocorticoid therapy, and less aggressive mechanical ventilation.<ref name="pmid5334613">Northway Jr, WH,
Pulmonary disease following respirator therapy of hyaline-membrane disease. Bronchopulmonary dysplasia., The New England Journal of Medicine, Vol. 276(Issue: 7), pp. 357–68, DOI: 10.1056/NEJM196702162760701, PMID: 5334613,</ref>
Currently the description of BPD includes the grading of its severity into mild, moderate and severe. This correlates with the infant's maturity, growth and overall severity of illness.<ref name="pmid15538399">Sahni, R,
Is the new definition of bronchopulmonary dysplasia more useful?, Journal of Perinatology, Vol. 25(Issue: 1), pp. 41–6, DOI: 10.1038/sj.jp.7211210, PMID: 15538399,</ref> The new system offers a better description of underlying pulmonary disease and its severity.<ref name="pmid16322158">Ehrenkranz, RA, Validation of the National Institutes of Health consensus definition of bronchopulmonary dysplasia, Pediatrics, Vol. 116(Issue: 6), pp. 1353–60, DOI: 10.1542/peds.2005-0249, PMID: 16322158,</ref>
Presentation
Complications
Feeding problems are common in infants with BPD, often due to prolonged intubation. Such infants often display oral-tactile hypersensitivity (also known as oral aversion).<ref>Gaining & Growing. "Bronchopulmonary dysplasia", Gaining & Growing, March 20, 2007. (Retrieved June 12, 2008.)</ref> Physical findings:
- hypoxemia;
- hypercapnia;
- crackles, wheezing, & decreased breath sounds;
- increased bronchial secretions;
- hyperinflation;
- frequent lower respiratory infections;
- delayed growth & development;
- cor pulmonale;
- CXR shows with hyperinflation, low diaphragm, atelectasis, cystic changes.
Cause
Prolonged high oxygen delivery in premature infants causes necrotizing bronchiolitis and alveolar septal injury, with inflammation and scarring. This results in hypoxemia. Today, with the advent of surfactant therapy and high frequency ventilation and oxygen supplementation, infants with BPD experience much milder injury without necrotizing bronchiolitis or alveolar septal fibrosis. Instead, there are usually uniformly dilated acini with thin alveolar septa and little or no interstitial fibrosis. It develops most commonly in the first 4 weeks after birth.
Diagnosis
Earlier criteria
The classic diagnosis of BPD may be assigned at 28 days of life if the following criteria are met:
- Positive pressure ventilation during the first 2 weeks of life for a minimum of 3 days.
- Clinical signs of abnormal respiratory function.
- Requirements for supplemental oxygen for longer than 28 days of age to maintain PaO2 above 50 mm Hg.
- Chest radiograph with diffuse abnormal findings characteristic of BPD.
Newer criteria
The newer National Institute of Health (US) criteria for BPD (for neonates treated with more than 21% oxygen for at least 28 days)<ref name="pmid16650652">Kinsella, JP,
Bronchopulmonary dysplasia, Lancet, Vol. 367(Issue: 9520), pp. 1421–31, DOI: 10.1016/S0140-6736(06)68615-7, PMID: 16650652,</ref> is as follows:,<ref>
Bronchopulmonary Dysplasia(link). {{{website}}}.
</ref><ref>,
Bronchopulmonary dysplasia, Am J Respir Crit Care Med, Vol. 163(Issue: 7), pp. 1723–9, DOI: 10.1164/ajrccm.163.7.2011060, PMID: 11401896,</ref>
- Mild
- Breathing room air at 36 weeks' post-menstrual age or discharge (whichever comes first) for babies born before 32 weeks, or
- breathing room air by 56 days' postnatal age, or discharge (whichever comes first) for babies born after 32 weeks' gestation.
- Moderate
- Need for <30% oxygen at 36 weeks' postmenstrual age, or discharge (whichever comes first) for babies born before 32 weeks, or
- need for <30% oxygen to 56 days' postnatal age, or discharge (whichever comes first) for babies born after 32 weeks' gestation.
- Severe
- Need for >30% oxygen, with or without positive pressure ventilation or continuous positive pressure at 36 weeks' postmenstrual age, or discharge (whichever comes first) for babies born before 32 weeks, or
- need for >30% oxygen with or without positive pressure ventilation or continuous positive pressure at 56 days' postnatal age, or discharge (whichever comes first) for babies born after 32 weeks' gestation.
Management
There is evidence to show that steroids given to babies less than 8 days old can prevent bronchopulmonary dysplasia.<ref name=":0">Doyle, Lex W,
Early (< 8 days) systemic postnatal corticosteroids for prevention of bronchopulmonary dysplasia in preterm infants, Cochrane Database of Systematic Reviews, Vol. 10, pp. CD001146, DOI: 10.1002/14651858.cd001146.pub5, PMID: 29063585, PMC: 6485683,</ref> However, the risks of neurodevelopmental sequelae may outweigh the benefits.<ref name=":0" /> It is unclear if starting steroids more than 7 days after birth is harmful or beneficial.<ref name=":1">Doyle, Lex W, Late (> 7 days) systemic postnatal corticosteroids for prevention of bronchopulmonary dysplasia in preterm infants, Cochrane Database of Systematic Reviews, Vol. 10, pp. CD001145, DOI: 10.1002/14651858.cd001145.pub4, PMID: 29063594, PMC: 6485440,</ref> It is thus recommended that they only be used in those who cannot be taken off of a ventilator.<ref name=":1" /> Evidence suggests that vitamin A in LBW babies is associated with a reduction in mortality and bronchopulmonary dysplasia.<ref>Guimarães, Hercília, Vitamin A in prevention of bronchopulmonary dysplasia, Current Pharmaceutical Design, Vol. 18(Issue: 21), pp. 3101–3113, DOI: 10.2174/1381612811209023101, PMID: 22564302,</ref>
Oxygen therapy at home is recommended in those with significant low oxygen levels.<ref>,
Home Oxygen Therapy for Children. An Official American Thoracic Society Clinical Practice Guideline., American Journal of Respiratory and Critical Care Medicine, Vol. 199(Issue: 3), pp. e5–e23, DOI: 10.1164/rccm.201812-2276ST, PMID: 30707039, PMC: 6802853,</ref>
Epidemiology
The rate of BPD varies among institutions, which may reflect neonatal risk factors, care practices (e.g., target levels for acceptable oxygen saturation), and differences in the clinical definitions of BPD.<ref name="pmid17306659">,
Trends in neonatal morbidity and mortality for very low birthweight infants, Am J Obstet Gynecol, 2007, Vol. 196(Issue: 2), pp. 147.e1–8, DOI: 10.1016/j.ajog.2006.09.014, PMID: 17306659,</ref><ref name="pmid10835057">, Do clinical markers of barotrauma and oxygen toxicity explain interhospital variation in rates of chronic lung disease? The Neonatology Committee for the Developmental Network, Pediatrics, 2000, Vol. 105(Issue: 6), pp. 1194–201, DOI: 10.1542/peds.105.6.1194, PMID: 10835057,</ref><ref name="pmid14726936">, Controversy surrounding the use of home oxygen for premature infants with bronchopulmonary dysplasia, J Perinatol, 2004, Vol. 24(Issue: 1), pp. 36–40, DOI: 10.1038/sj.jp.7211012, PMID: 14726936,</ref>
See also
References
Further reading
- Bhandari, A,
Bronchopulmonary dysplasia: an update, Indian Journal of Pediatrics, Vol. 74(Issue: 1), pp. 73–7, DOI: 10.1007/s12098-007-0032-z, PMID: 17264460, Full text,
- Bronchopulmonary Dysplasia on National Institutes of Health
External links
| Conditions originating in the perinatal period / fetal disease | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
|
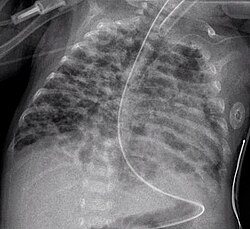
Bronchopulmonary dysplasia
-
Chest X-ray showing bronchopulmonary dysplasia
Ad. Transform your health with W8MD Weight Loss, Sleep & MedSpa

Tired of being overweight?
Special offer:
Budget GLP-1 weight loss medications
- Semaglutide starting from $29.99/week and up with insurance for visit of $59.99 and up per week self pay.
- Tirzepatide starting from $45.00/week and up (dose dependent) or $69.99/week and up self pay
✔ Same-week appointments, evenings & weekends
Learn more:
- GLP-1 weight loss clinic NYC
- W8MD's NYC medical weight loss
- W8MD Philadelphia GLP-1 shots
- Philadelphia GLP-1 injections
- Affordable GLP-1 shots NYC
|
WikiMD Medical Encyclopedia |
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian