Dermatophytosis: Difference between revisions
m Text replacement - "Category:Wikipedia medicine articles ready to translate" to "" |
CSV import |
||
| Line 102: | Line 102: | ||
[[Category:Cat diseases]] | [[Category:Cat diseases]] | ||
<gallery> | |||
File:Yeartinfection.JPG|Dermatophytosis | |||
File:Fox_Plate_LXXXIX.jpg|Dermatophytosis | |||
File:Toplin_des_dieles_tiesse_vea.jpg|Dermatophytosis | |||
File:Dieles_åtoû_d'_l'_ouy_åmea.JPG|Dermatophytosis | |||
File:2_dieles_mashale.jpg|Dermatophytosis | |||
File:Viye_diele_did_près.JPG|Dermatophytosis | |||
File:Diele_vea_waerot.jpg|Dermatophytosis | |||
File:Dieles_cawî_åmea.JPG|Dermatophytosis | |||
</gallery> | |||
Revision as of 11:17, 18 February 2025
A common fungal infection of the stratum corneum of the skin, hair, or nails by a dermatophyte.
Other names
- Ringworm
- Tinea
- Athlete's foot (location specific)
Clinical features
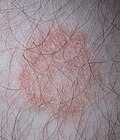
It is characterized by itching, inflammation, redness of the skin, small papular vesicles, central clearing, fissures, scaling, and/or hair loss in the affected area.
Cause
Ringworm is a common skin infection that is caused by fungus.
Areas of the body that can be affected by ringworm include:
- Feet (tinea pedis, commonly called “athlete’s foot”)
- Groin, inner thighs, or buttocks (tinea cruris, commonly called “jock itch”)
- Scalp (tinea capitis)
- Beard (tinea barbae)
- Hands (tinea manuum)
- Toenails or fingernails (tinea unguium, also called “onychomycosis”) Click here for more information about fungal nail infections.
- Other parts of the body such as arms or legs (tinea corporis)
Fungal species
- Approximately 40 different species of fungi can cause ringworm;
- The scientific names for the types of fungi that cause ringworm are Trichophyton, Microsporum, and Epidermophyton.
Diagnosis
Physical examination
- A thorough history and physical examination is often sufficient to diagnose tinea.
- The classic lesion is an erythematous, raised, scaly ring with central clearing.
- Multiple lesions may be present.
Microscopy
- Potassium hydroxide (KOH) stain a commonly-used method for diagnosing tinea because it is inexpensive, easy to perform, and has high sensitivity.
- Scrapings from the lesion(s) are placed in a drop of KOH and examined under a microscope for the presence of fungal hyphae.
Ultraviolet light (Wood’s lamp)
- Normally, ultraviolet light is not useful in the diagnosis of tinea with the exception of two species – Microsporum canis and audouinii.
- Although both species fluoresce blue-green under a Wood’s lamp, both species are uncommon causes of tinea infections.
- A Wood’s lamp may be useful to differentiate between erythrasma caused by Corynebacterium minutissimum (which fouresces coal-red) from tinea cruris, which is non-fluorescent.
Culture
- Fungal culture can be performed as a confirmatory test if results from a KOH stain are inconclusive.
- Hair and/or scrapings extracted from affected areas are placed on Sabouraud’s medium.
- Fungal culture is more specific than KOH stain, but it can take up to three weeks to become positive.
Treatment
- Some forms of ringworm can be treated with non-prescription (“over-the-counter”) antifungal creams, lotions, or powders.
- Other forms of ringworm need treatment with prescription antifungal medications depending on the type of fungus.
Tinea pedis: Athlete’s foot can usually be treated with over-the-counter topical antifungal products;
- terbinafine appears to be most effective, but other agents can also be used.
- Chronic or extensive tinea pedis may require treatment with oral antifungal agents such as terbinafine, itraconazole, or fluconazole.
- In addition, chronic tinea pedis may require adjunctive therapy such as foot powder or talcum powder to prevent skin maceration.
Tinea capitis: Treatment with systemic antifungal medication is required, as topical antifungal products are ineffective for treatment of tinea capitis.
- Many experts consider griseofulvin to be the drug of choice.
- Terbinafine is also FDA-approved for the treatment of tinea capitis in patients four years of age and older.
- Itraconazole and fluconazole have been shown to be safe and effective, but are not FDA-approved for this indication.
- Selenium sulfide shampoos can be used as adjunctive therapy.
Tinea corporis/Tinea cruris: Tinea corporis and tinea cruris can usually be treated with over-the-counter antifungal products.
- Patients who have tinea cruris should be advised to keep the groin area clean and dry and to wear cotton underwear.
- Persons who have extensive or recurrent infections may require systemic antifungal therapy.
Steroids should not be used
- People who have ringworm don’t always know what’s causing their rash, and people sometimes apply over-the-counter creams or ointments containing corticosteroids (or “steroids” for short) to their rash.
- Steroid creams don’t kill the fungus that causes ringworm.
- Steroid creams also can make ringworm worse because they weaken the skin’s defenses.
- In rare cases, steroid creams allow the fungus that causes ringworm to invade deeper into the skin and cause a more serious condition.
- Steroid creams can make ringworm infections spread to cover more of the body.
An Emerging International Problem in India
- Dermatologists in India have reported severe steroid-modified tinea associated with use of over-the-counter mid- to high-potency topical corticosteroids, which are commonly sold as fixed-dose combinations with an antifungal medication and one or two antibacterial medications.
- In India, a dermatophyte species often identified as Trichophyton mentagrophytes has been reported as the cause of these breakthrough infections.
-
Dermatophytosis 1
-
Dermatophytosis 2
-
Dermatophytosis 3
-
Dermatophytosis 4
-
Dermatophytosis 5
-
Dermatophytosis 6
-
Dermatophytosis 7
-
Athlete's foot
|
|
|
-
Dermatophytosis
-
Dermatophytosis
-
Dermatophytosis
-
Dermatophytosis
-
Dermatophytosis
-
Dermatophytosis
-
Dermatophytosis
-
Dermatophytosis