Zygomycosis

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Zygomycosis | |
|---|---|
| |
| Synonyms | Mucormycosis, Phycomycosis |
| Pronounce | N/A |
| Specialty | N/A |
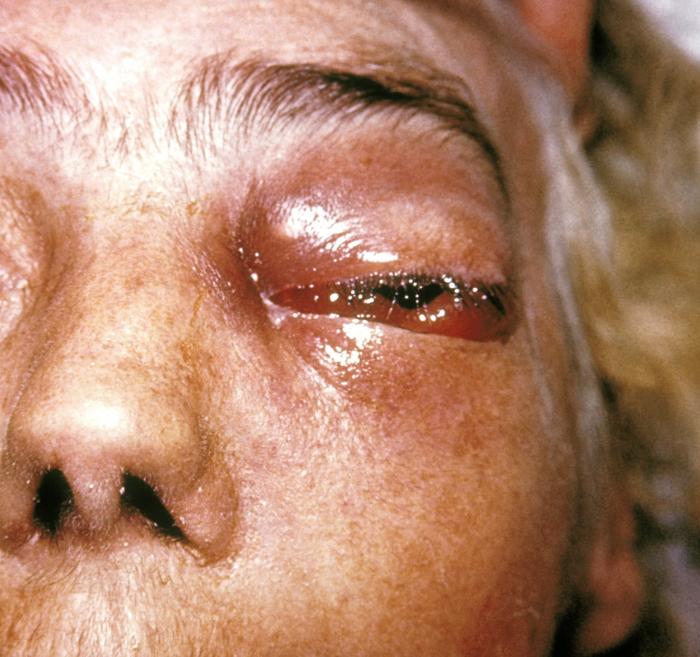
| Symptoms | Fever, headache, facial swelling, nasal congestion, black lesions on nasal bridge or upper inside of mouth |
| Complications | Tissue necrosis, blindness, cerebral infarction, death |
| Onset | Rapid |
| Duration | Variable |
| Types | N/A |
| Causes | Fungal infection by Mucorales |
| Risks | Diabetes mellitus, immunosuppression, iron overload, trauma, burns |
| Diagnosis | Biopsy, culture, imaging studies |
| Differential diagnosis | Bacterial sinusitis, aspergillosis, granulomatosis with polyangiitis |
| Prevention | N/A |
| Treatment | Antifungal medication, surgical debridement |
| Medication | Amphotericin B, posaconazole, isavuconazole |
| Prognosis | Poor if untreated |
| Frequency | Rare |
| Deaths | N/A |
Zygomycosis
Zygomycosis, also known as mucormycosis, is a serious fungal infection caused by fungi in the order Mucorales. This rare but potentially life-threatening condition primarily affects individuals with compromised immune systems, such as those with uncontrolled diabetes, cancer patients, organ transplant recipients, and individuals receiving immunosuppressive drugs.
Causes and Risk Factors[edit]
Zygomycosis is caused by the inhalation of fungal spores from the environment. The fungi responsible for this infection belong to several genera, most notably Rhizopus, Mucor, and Absidia. These fungi are ubiquitous in nature, found in soil, decaying organic matter, and even in the air. While these spores are commonly inhaled by people every day without causing infection, individuals with weakened immune systems are at a higher risk of developing zygomycosis.
Symptoms and Diagnosis[edit]
The symptoms of zygomycosis vary depending on the part of the body affected. The infection can manifest in several forms, including rhinocerebral, pulmonary, cutaneous, gastrointestinal, and disseminated zygomycosis. The most common form, rhinocerebral zygomycosis, begins with symptoms such as fever, nasal congestion, and headaches. As the infection progresses, it can lead to facial swelling, black lesions on the nasal bridge or upper inside of the mouth, and potentially, loss of vision or neurological deficits. Diagnosis of zygomycosis involves a combination of clinical assessment, imaging studies, and laboratory tests. Biopsy and culture of the affected tissues are crucial for confirming the presence of the fungi.
Treatment[edit]
Treatment of zygomycosis requires an aggressive approach that includes antifungal therapy, surgical debridement of infected tissue, and management of underlying conditions. The primary antifungal medication used is Amphotericin B, although newer agents like posaconazole and isavuconazole have also been used. Early diagnosis and treatment are critical for improving outcomes, as the infection can rapidly become fatal if not promptly addressed.
Prevention[edit]
Preventive measures for zygomycosis are primarily focused on individuals with high-risk conditions. These include controlling diabetes mellitus, reducing the use of immunosuppressive drugs when possible, and employing protective measures in environments with a high concentration of fungal spores.
Epidemiology[edit]
Zygomycosis is a rare infection, with its incidence increasing in recent years, possibly due to the growing number of individuals with compromised immune systems. It has a global distribution, with no specific geographic predilection.
Prognosis[edit]
The prognosis for individuals with zygomycosis depends on several factors, including the site of infection, the extent of disease, the patient's immune status, and the timeliness of treatment. Despite aggressive treatment, the mortality rate remains high, especially in cases of disseminated infection.
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian