Histidinemia

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Histidinemia | |
|---|---|
 | |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Usually asymptomatic, may include developmental delay, speech disorder |
| Complications | N/A |
| Onset | Neonatal |
| Duration | Lifelong |
| Types | N/A |
| Causes | Genetic mutation in the HAL gene |
| Risks | Consanguinity |
| Diagnosis | Newborn screening, urine test, blood test |
| Differential diagnosis | Phenylketonuria, Maple syrup urine disease |
| Prevention | N/A |
| Treatment | Dietary management, amino acid restriction |
| Medication | N/A |
| Prognosis | Generally good with management |
| Frequency | 1 in 10,000 to 1 in 100,000 |
| Deaths | Rare |
Other Names: Histidase deficiency; HIS deficiency; HAL deficiency; Histidine ammonia-lyase deficiency
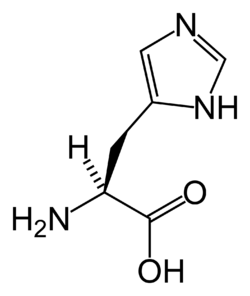
Histidinemia is an inherited metabolic condition characterized by elevated levels of the amino acid histidine in blood, urine, and cerebrospinal fluid.
Epidemiology[edit]
Estimates of the incidence of histidinemia vary widely, ranging between 1 in 8,600 to 1 in 90,000 people.
Cause[edit]
Histidinemia is caused by mutations in the HAL gene, which provides instructions for making an enzyme called histidase. Histidase breaks down histidine to a molecule called urocanic acid. Histidase is active (expressed) primarily in the liver and the skin. HAL gene mutations lead to the production of a histidase enzyme that cannot break down histidine, which results in elevated levels of histidine in the blood and urine. These increased levels of histidine do not appear to have any negative effects on the body.
Inheritance[edit]
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Signs and symptoms[edit]
In most cases, people with this condition have no health problems and may not even know that they are affected. Individuals with histidinemia who also experience a medical complication during or shortly after birth (such as a temporary lack of oxygen), may be at an increased risk of developing intellectual disability, behavioral problems, or learning disabilities. For most diseases, symptoms will vary from person to person. People with the same disease may not have all the symptoms listed. 100% of people have these symptoms
- Histidinuria(High urine histidine levels)
- Hyperhistidinemia(High blood histidine level)
5%-29% of people have these symptoms
- Behavioral abnormality(Behavioral changes)
- Neurological speech impairment(Speech impairment)
1%-4% of people have these symptoms
- Hyperactivity(More active than typical)
- Intellectual disability(Mental deficiency)
- Moderate global developmental delay
- Specific learning disability
Diagnosis[edit]
Histidenemia is characterized by increased levels of histidine, histamine and imidazole in blood, urine and cerebrospinal fluid. This also results in decreased levels of the metabolite urocanic acid in blood, urine, and skin cells. In Japan, neonatal screening was previously performed on infants within 1 month of birth; infants demonstrating a blood histidine level of 6 mg/dl or more underwent careful testing as suspected histidinemia cases. A typical characteristic of histidinemia is an increase in the blood histidine levels from normal levels (70-120 μM) to an elevated level (290-1420 μM). Further testing includes: observing histidine as well as imidazolepyruvic acid metabolites in the urine. However, neonatal urine testing has been discontinued in most places, with the exception of Quebec.
Treatment[edit]
Because there are no symptoms associated with this condition, treatment is not necessary. It has been suggested that a possible method of treatment for histidinemia is through the adoption of a diet that is low in histidine intake. However, the requirement for such dietary restrictions is typically unnecessary for 99% of all cases of histidinemia.
| Inborn error of amino acid metabolism | ||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
NIH genetic and rare disease info[edit]
Histidinemia is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Histidinemia
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian