Gitelman syndrome: Difference between revisions
mNo edit summary |
CSV import |
||
| Line 1: | Line 1: | ||
== Gitelman syndrome == | {{SI}} | ||
{{Infobox medical condition | |||
Other Names:[[ Potassium and magnesium depletion]]; [[Hypomagnesemia-hypokalemia]], primary renotubular, with hypocalciuria; Familial hypokalemia-hypomagnesemia; Gitelman's syndrome | | name = Gitelman syndrome | ||
| image = [[File:Gitelman_syndrome.jpg|alt=Gitelman syndrome]] | |||
| caption = | |||
| synonyms = Familial hypokalemia-hypomagnesemia | |||
| pronounce = | |||
| specialty = [[Nephrology]] | |||
| symptoms = [[Muscle weakness]], [[cramps]], [[fatigue]], [[tetany]], [[numbness]] | |||
| complications = [[Cardiac arrhythmias]], [[chondrocalcinosis]] | |||
| onset = Childhood or early adulthood | |||
| duration = Lifelong | |||
| types = | |||
| causes = [[Genetic mutation]] in the [[SLC12A3]] gene | |||
| risks = | |||
| diagnosis = [[Blood test]], [[urine test]], [[genetic testing]] | |||
| differential = [[Bartter syndrome]], [[Liddle syndrome]], [[diuretic use]] | |||
| prevention = | |||
| treatment = [[Oral supplementation]] of [[magnesium]] and [[potassium]] | |||
| medication = [[Potassium-sparing diuretics]] | |||
| prognosis = Generally good with treatment | |||
| frequency = 1 in 40,000 | |||
| deaths = Rare | |||
}} | |||
Other Names:[[ Potassium and magnesium depletion]]; [[Hypomagnesemia-hypokalemia]], primary renotubular, with hypocalciuria; Familial hypokalemia-hypomagnesemia; Gitelman's syndrome | |||
Gitelman syndrome is a [[kidney disorder]] that causes an imbalance of charged atoms (ions) in the body, including ions of potassium, magnesium, and calcium. | Gitelman syndrome is a [[kidney disorder]] that causes an imbalance of charged atoms (ions) in the body, including ions of potassium, magnesium, and calcium. | ||
<youtube> | <youtube> | ||
title='''{{PAGENAME}}''' | title='''{{PAGENAME}}''' | ||
| Line 16: | Line 35: | ||
height=600 | height=600 | ||
</youtube> | </youtube> | ||
=='''Onset'''== | =='''Onset'''== | ||
The signs and symptoms of Gitelman syndrome usually appear in late childhood or [[adolescence]]. | The signs and symptoms of Gitelman syndrome usually appear in late childhood or [[adolescence]]. | ||
=='''Epidemiology'''== | =='''Epidemiology'''== | ||
Gitelman syndrome affects an estimated 1 in 40,000 people worldwide. | Gitelman syndrome affects an estimated 1 in 40,000 people worldwide. | ||
=='''Cause'''== | =='''Cause'''== | ||
Gitelman syndrome is usually caused by mutations in the '''[[SLC12A3 gene]]'''. Less often, the condition results from mutations in the''' [[CLCNKB gene]]'''. '''The proteins produced from these genes are involved in the kidneys' reabsorption of salt (sodium chloride or NaCl) from urine back into the [[bloodstream]].''' Mutations in either gene impair the''' kidneys' ability to reabsorb salt, leading to the loss of excess salt in the urine (salt wasting).''' Abnormalities of salt transport also affect the reabsorption of other ions, including ions of potassium, magnesium, and calcium. The resulting imbalance of ions in the body underlies the major features of Gitelman syndrome. | Gitelman syndrome is usually caused by mutations in the '''[[SLC12A3 gene]]'''. Less often, the condition results from mutations in the''' [[CLCNKB gene]]'''. '''The proteins produced from these genes are involved in the kidneys' reabsorption of salt (sodium chloride or NaCl) from urine back into the [[bloodstream]].''' Mutations in either gene impair the''' kidneys' ability to reabsorb salt, leading to the loss of excess salt in the urine (salt wasting).''' Abnormalities of salt transport also affect the reabsorption of other ions, including ions of potassium, magnesium, and calcium. The resulting imbalance of ions in the body underlies the major features of Gitelman syndrome. | ||
=='''Inheritance'''== | |||
This condition is inherited in an [[autosomal recessive]] pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the [[mutated gene]], but they typically do not show signs and symptoms of the condition. | This condition is inherited in an [[autosomal recessive]] pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the [[mutated gene]], but they typically do not show signs and symptoms of the condition. | ||
=='''Signs and symptoms'''== | =='''Signs and symptoms'''== | ||
Signs and symptoms of Gitelman syndrome tend to present in [[adolescents]] and adults, but occasionally present in infants and young children. Signs and symptoms in children and adults vary, but may include: | Signs and symptoms of Gitelman syndrome tend to present in [[adolescents]] and adults, but occasionally present in infants and young children. Signs and symptoms in children and adults vary, but may include: | ||
A preference for salty foods (salt craving) | A preference for salty foods (salt craving) | ||
*Muscle weakness | *Muscle weakness | ||
*[[Fatigue]] | *[[Fatigue]] | ||
| Line 46: | Line 59: | ||
*Excessive thirst | *Excessive thirst | ||
*Abdominal pain | *Abdominal pain | ||
Adults with Gitelman syndrome may also experience dizziness, [[vertigo]], excessive amount of urine, urinating more at night, heart [[palpitations]], joint pain, and vision problems. | Adults with Gitelman syndrome may also experience dizziness, [[vertigo]], excessive amount of urine, urinating more at night, heart [[palpitations]], joint pain, and vision problems. | ||
Other possible symptoms include low blood pressure, a painful joint condition called, [[chondrocalcinosis]], prolonged [[QT interval]] (a rare heart problem that may cause irregular heartbeat, fainting, or sudden death), episodes of elevated body temperature, vomiting, constipation, bed wetting, and [[paralysis]]. Additional rare symptoms have been described in single cases. | Other possible symptoms include low blood pressure, a painful joint condition called, [[chondrocalcinosis]], prolonged [[QT interval]] (a rare heart problem that may cause irregular heartbeat, fainting, or sudden death), episodes of elevated body temperature, vomiting, constipation, bed wetting, and [[paralysis]]. Additional rare symptoms have been described in single cases. | ||
=='''Diagnosis'''== | =='''Diagnosis'''== | ||
A diagnosis of Gitelman syndrome may be suspected in children and adults with characteristic symptoms. A number of blood and urine tests aid in the diagnosis of Gitelman syndrome, such as: | A diagnosis of Gitelman syndrome may be suspected in children and adults with characteristic symptoms. A number of blood and urine tests aid in the diagnosis of Gitelman syndrome, such as: | ||
*[[Potassium urine test]] | *[[Potassium urine test]] | ||
*[[Blood gases]] | *[[Blood gases]] | ||
*Blood tests to measure magnesium, aldosterone, and renin | *Blood tests to measure magnesium, aldosterone, and renin | ||
*Urine analysis for sodium, potassium, and calcium | *Urine analysis for sodium, potassium, and calcium | ||
Common blood and urine abnormalities found in Gitelman syndrome, include: | |||
Common blood and urine abnormalities found in Gitelman syndrome, include: | |||
*Low levels of potassium in the blood (hypokalemia) | *Low levels of potassium in the blood (hypokalemia) | ||
*Metabolic alkalosis (too much base in the body) | *Metabolic alkalosis (too much base in the body) | ||
*Low magnesium in the blood (hypomagnesemia) | *Low magnesium in the blood (hypomagnesemia) | ||
*Low levels of calcium in the urine (hypocalciuria) | *Low levels of calcium in the urine (hypocalciuria) | ||
[[Anorexia]], [[bulimia]], [[chronic diarrhea]], [[vomiting]], and long term use of [[laxatives]] or [[diuretics]] can cause similar signs and symptoms. Before a diagnosis of Gitelman syndrome is made these conditions must be ruled out. A careful review of the patient and family health histories, as well as renal ultrasound findings can be helpful in ruling out other causes. | |||
[[Anorexia]], [[bulimia]], [[chronic diarrhea]], [[vomiting]], and long term use of [[laxatives]] or [[diuretics]] can cause similar signs and symptoms. Before a diagnosis of Gitelman syndrome is made these conditions must be ruled out. A careful review of the patient and family health histories, as well as renal ultrasound findings can be helpful in ruling out other causes. | |||
[[Genetic testing]] can confirm a diagnosis of Gitelman syndrome. Tools for finding genetic testing for Gitelman syndrome are available below. | [[Genetic testing]] can confirm a diagnosis of Gitelman syndrome. Tools for finding genetic testing for Gitelman syndrome are available below. | ||
=='''Treatment'''== | =='''Treatment'''== | ||
The mainstay treatment of Gitelman syndrome involves careful monitoring, [[high-sodium and potassium diet]], and [[oral potassium and magnesium supplements]]. [[Intravenous magnesium and/or potassium]] may be needed if symptoms are severe. People who have low potassium levels despite supplementation and diet, may benefit from potassium-sparing diuretics, renin angiotensin system blockers, pain medications, and/or [[nonsteroidal anti-inflammatory drugs]] (NSAIDs). | The mainstay treatment of Gitelman syndrome involves careful monitoring, [[high-sodium and potassium diet]], and [[oral potassium and magnesium supplements]]. [[Intravenous magnesium and/or potassium]] may be needed if symptoms are severe. People who have low potassium levels despite supplementation and diet, may benefit from potassium-sparing diuretics, renin angiotensin system blockers, pain medications, and/or [[nonsteroidal anti-inflammatory drugs]] (NSAIDs). | ||
The Blanchard A et al., 2017 consensus guideline offers detailed treatment information, including information on drug selection, dosing recommendations, and a listing of drugs that can cause adverse effects in people with Gitelman syndrome. | |||
The Blanchard A et al., 2017 consensus guideline offers detailed treatment information, including information on drug selection, dosing recommendations, and a listing of drugs that can cause adverse effects in people with Gitelman syndrome. | Lastly, people with Gitelman syndrome should have a thorough heart work-up. People with Gitelman syndrome and a prolonged [[QT interval]] should avoid drugs that prolong the QT interval. | ||
Lastly, people with Gitelman syndrome should have a thorough heart work-up. People with Gitelman syndrome and a prolonged [[QT interval]] should avoid drugs that prolong the QT interval. | |||
=='''Prognosis'''== | =='''Prognosis'''== | ||
The long-term outlook (prognosis) for people with Gitelman syndrome is generally very good. However, the symptoms and severity can vary from person to person. Some people do not develop any symptoms, while others develop chronic issues that can impact their quality of life. Weakness, [[fatigue]] and [[muscle cramping]] can affect daily activities in some people with Gitelman syndrome. In general, while the underlying condition does not appear to be progressive, complications can arise, especially if care recommendations are not followed. | The long-term outlook (prognosis) for people with Gitelman syndrome is generally very good. However, the symptoms and severity can vary from person to person. Some people do not develop any symptoms, while others develop chronic issues that can impact their quality of life. Weakness, [[fatigue]] and [[muscle cramping]] can affect daily activities in some people with Gitelman syndrome. In general, while the underlying condition does not appear to be progressive, complications can arise, especially if care recommendations are not followed. | ||
Progressive [[renal insufficiency]] is extremely rare. [[Renal function]] is usually maintained despite long-term [[hypokalemia]] (low potassium), but progression to chronic renal insufficiency has rarely been reported. | Progressive [[renal insufficiency]] is extremely rare. [[Renal function]] is usually maintained despite long-term [[hypokalemia]] (low potassium), but progression to chronic renal insufficiency has rarely been reported. | ||
Some people with Gitelman syndrome may be at risk of developing cardiac [[arrhythmias]]. Those with severe hypokalemia are more susceptible to cardiac arrhythmias, which can be life-threatening when joined with severe [[hypomagnesemia]] (low magnesium) and [[alkalosis]]. Therefore, an in-depth cardiac work-up is strongly recommended to identify which people with Gitelman syndrome may be at risk. Competitive sports should be avoided because sudden death can be precipitated by intense physical activity that induces potassium and magnesium loss by [[sweating]]. | Some people with Gitelman syndrome may be at risk of developing cardiac [[arrhythmias]]. Those with severe hypokalemia are more susceptible to cardiac arrhythmias, which can be life-threatening when joined with severe [[hypomagnesemia]] (low magnesium) and [[alkalosis]]. Therefore, an in-depth cardiac work-up is strongly recommended to identify which people with Gitelman syndrome may be at risk. Competitive sports should be avoided because sudden death can be precipitated by intense physical activity that induces potassium and magnesium loss by [[sweating]]. | ||
{{Nephrology}} | {{Nephrology}} | ||
{{Membrane transport protein disorders}} | {{Membrane transport protein disorders}} | ||
{{DEFAULTSORT:Gitelman Syndrome}} | {{DEFAULTSORT:Gitelman Syndrome}} | ||
[[Category:Autosomal recessive disorders]] | [[Category:Autosomal recessive disorders]] | ||
Latest revision as of 02:19, 7 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Gitelman syndrome | |
|---|---|
| |
| Synonyms | Familial hypokalemia-hypomagnesemia |
| Pronounce | |
| Specialty | Nephrology |
| Symptoms | Muscle weakness, cramps, fatigue, tetany, numbness |
| Complications | Cardiac arrhythmias, chondrocalcinosis |
| Onset | Childhood or early adulthood |
| Duration | Lifelong |
| Types | |
| Causes | Genetic mutation in the SLC12A3 gene |
| Risks | |
| Diagnosis | Blood test, urine test, genetic testing |
| Differential diagnosis | Bartter syndrome, Liddle syndrome, diuretic use |
| Prevention | |
| Treatment | Oral supplementation of magnesium and potassium |
| Medication | Potassium-sparing diuretics |
| Prognosis | Generally good with treatment |
| Frequency | 1 in 40,000 |
| Deaths | Rare |
Other Names:Potassium and magnesium depletion; Hypomagnesemia-hypokalemia, primary renotubular, with hypocalciuria; Familial hypokalemia-hypomagnesemia; Gitelman's syndrome
Gitelman syndrome is a kidney disorder that causes an imbalance of charged atoms (ions) in the body, including ions of potassium, magnesium, and calcium.
Onset[edit]
The signs and symptoms of Gitelman syndrome usually appear in late childhood or adolescence.
Epidemiology[edit]
Gitelman syndrome affects an estimated 1 in 40,000 people worldwide.
Cause[edit]
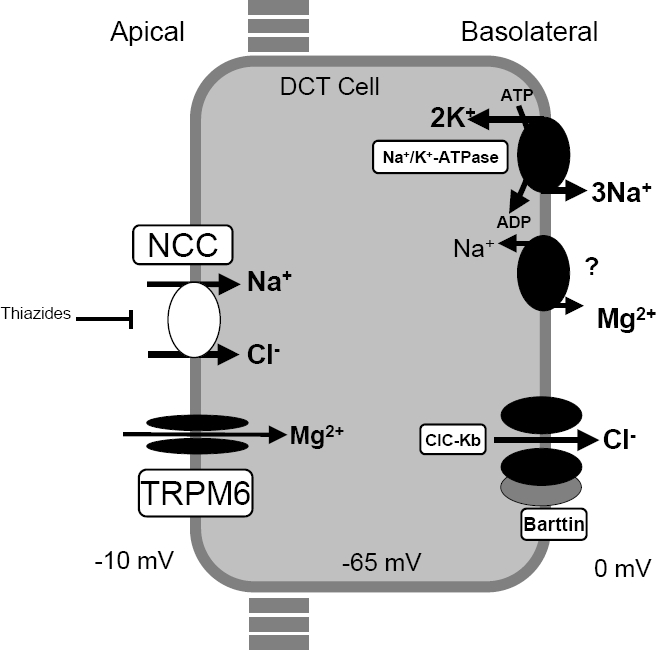
Gitelman syndrome is usually caused by mutations in the SLC12A3 gene. Less often, the condition results from mutations in the CLCNKB gene. The proteins produced from these genes are involved in the kidneys' reabsorption of salt (sodium chloride or NaCl) from urine back into the bloodstream. Mutations in either gene impair the kidneys' ability to reabsorb salt, leading to the loss of excess salt in the urine (salt wasting). Abnormalities of salt transport also affect the reabsorption of other ions, including ions of potassium, magnesium, and calcium. The resulting imbalance of ions in the body underlies the major features of Gitelman syndrome.
Inheritance[edit]
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Signs and symptoms[edit]
Signs and symptoms of Gitelman syndrome tend to present in adolescents and adults, but occasionally present in infants and young children. Signs and symptoms in children and adults vary, but may include: A preference for salty foods (salt craving)
- Muscle weakness
- Fatigue
- Limited sports performance or endurance
- Episodes of fainting
- Cramps
- Muscle spasms
- Numbness or tingling (such as of the face)
- Growth delay
- Delayed puberty
- Short stature
- Excessive thirst
- Abdominal pain
Adults with Gitelman syndrome may also experience dizziness, vertigo, excessive amount of urine, urinating more at night, heart palpitations, joint pain, and vision problems. Other possible symptoms include low blood pressure, a painful joint condition called, chondrocalcinosis, prolonged QT interval (a rare heart problem that may cause irregular heartbeat, fainting, or sudden death), episodes of elevated body temperature, vomiting, constipation, bed wetting, and paralysis. Additional rare symptoms have been described in single cases.
Diagnosis[edit]
A diagnosis of Gitelman syndrome may be suspected in children and adults with characteristic symptoms. A number of blood and urine tests aid in the diagnosis of Gitelman syndrome, such as:
- Potassium urine test
- Blood gases
- Blood tests to measure magnesium, aldosterone, and renin
- Urine analysis for sodium, potassium, and calcium
Common blood and urine abnormalities found in Gitelman syndrome, include:
- Low levels of potassium in the blood (hypokalemia)
- Metabolic alkalosis (too much base in the body)
- Low magnesium in the blood (hypomagnesemia)
- Low levels of calcium in the urine (hypocalciuria)
Anorexia, bulimia, chronic diarrhea, vomiting, and long term use of laxatives or diuretics can cause similar signs and symptoms. Before a diagnosis of Gitelman syndrome is made these conditions must be ruled out. A careful review of the patient and family health histories, as well as renal ultrasound findings can be helpful in ruling out other causes. Genetic testing can confirm a diagnosis of Gitelman syndrome. Tools for finding genetic testing for Gitelman syndrome are available below.
Treatment[edit]
The mainstay treatment of Gitelman syndrome involves careful monitoring, high-sodium and potassium diet, and oral potassium and magnesium supplements. Intravenous magnesium and/or potassium may be needed if symptoms are severe. People who have low potassium levels despite supplementation and diet, may benefit from potassium-sparing diuretics, renin angiotensin system blockers, pain medications, and/or nonsteroidal anti-inflammatory drugs (NSAIDs). The Blanchard A et al., 2017 consensus guideline offers detailed treatment information, including information on drug selection, dosing recommendations, and a listing of drugs that can cause adverse effects in people with Gitelman syndrome. Lastly, people with Gitelman syndrome should have a thorough heart work-up. People with Gitelman syndrome and a prolonged QT interval should avoid drugs that prolong the QT interval.
Prognosis[edit]
The long-term outlook (prognosis) for people with Gitelman syndrome is generally very good. However, the symptoms and severity can vary from person to person. Some people do not develop any symptoms, while others develop chronic issues that can impact their quality of life. Weakness, fatigue and muscle cramping can affect daily activities in some people with Gitelman syndrome. In general, while the underlying condition does not appear to be progressive, complications can arise, especially if care recommendations are not followed. Progressive renal insufficiency is extremely rare. Renal function is usually maintained despite long-term hypokalemia (low potassium), but progression to chronic renal insufficiency has rarely been reported. Some people with Gitelman syndrome may be at risk of developing cardiac arrhythmias. Those with severe hypokalemia are more susceptible to cardiac arrhythmias, which can be life-threatening when joined with severe hypomagnesemia (low magnesium) and alkalosis. Therefore, an in-depth cardiac work-up is strongly recommended to identify which people with Gitelman syndrome may be at risk. Competitive sports should be avoided because sudden death can be precipitated by intense physical activity that induces potassium and magnesium loss by sweating.
| Genetic disorder, membrane: Solute carrier disorders | ||||||||
|---|---|---|---|---|---|---|---|---|
see also solute carrier family
|
NIH genetic and rare disease info[edit]
Gitelman syndrome is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Gitelman syndrome
|


