Metabolic dysfunction–associated steatotic liver disease

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Metabolic dysfunction–associated steatotic liver disease | |
|---|---|

| |
| Synonyms | MASLD |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Often asymptomatic, fatigue, right upper quadrant pain |
| Complications | Cirrhosis, liver cancer, cardiovascular disease |
| Onset | Typically in adulthood |
| Duration | Chronic |
| Types | N/A |
| Causes | Metabolic syndrome, obesity, type 2 diabetes, dyslipidemia |
| Risks | Insulin resistance, hypertension, sedentary lifestyle |
| Diagnosis | Liver function tests, ultrasound, liver biopsy |
| Differential diagnosis | Alcoholic liver disease, viral hepatitis, autoimmune hepatitis |
| Prevention | Weight loss, dietary changes, physical activity |
| Treatment | Lifestyle modification, medication, bariatric surgery |
| Medication | N/A |
| Prognosis | Variable, depends on stage and treatment |
| Frequency | Increasing worldwide, common in developed countries |
| Deaths | N/A |


Metabolic dysfunction–associated steatotic liver disease (MAFLD), previously known as non-alcoholic fatty liver disease (NAFLD), is a type of liver disease characterized by the accumulation of fat in the liver of people who drink little to no alcohol. It is closely associated with metabolic syndrome, which is why the name was changed to reflect its metabolic dysfunction origin.
Definition[edit]
MAFLD is defined by the presence of steatosis in patients who have overweight or obesity, type 2 diabetes mellitus, or evidence of metabolic dysregulation. The term MAFLD can be applied to both non-alcoholic fatty liver (NAFL) and non-alcoholic steatohepatitis (NASH).
Epidemiology[edit]
MAFLD is the most common liver disorder in Western countries, affecting about 25% of the population. It is also increasingly recognized in developing countries due to the global epidemic of obesity and type 2 diabetes.
Pathophysiology[edit]
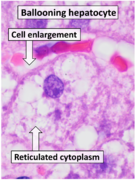
The pathogenesis of MAFLD is complex and involves multiple parallel hits, including insulin resistance, secretion of pro-inflammatory cytokines, oxidative stress, and mitochondrial dysfunction. The disease progresses from simple steatosis to steatohepatitis, fibrosis, and eventually cirrhosis and hepatocellular carcinoma.
Diagnosis[edit]
Diagnosis of MAFLD is usually made by imaging studies such as ultrasound, CT scan, or MRI, which can detect fat in the liver. Liver biopsy is the gold standard for diagnosing MAFLD, but it is invasive and has potential complications.
Treatment[edit]
The mainstay of treatment for MAFLD is lifestyle modification, including diet, exercise, and weight loss. Pharmacological therapies are also available, but their long-term efficacy and safety are still under investigation.
Prognosis[edit]
The prognosis of MAFLD varies depending on the stage of the disease. Patients with simple steatosis have a relatively benign course, while those with NASH, fibrosis, or cirrhosis have a higher risk of liver-related morbidity and mortality.
-
NASH stage 6
-
NASH stage 2
-
Histopathology of inflammatory foci in MASH
-
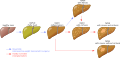
NAFLD liver progression
-
MRI Liver steatosis
-
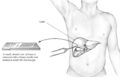
Human liver biopsy sample
-
Non-alcoholic fatty liver disease
-
Bariatric surgery in NAFLD
See also[edit]
| Liver diseases | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
This liver disease related article is a stub.
|
| Metabolic disorders | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
This metabolic disorder related article is a stub.
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian