Prolonged labor

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
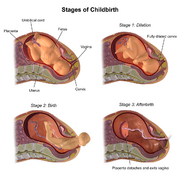
| Prolonged labor | |
|---|---|
| |
| Synonyms | Failure to progress, dystocia |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Labor lasting more than 20 hours for first-time mothers, or more than 14 hours for women who have given birth before |
| Complications | Fetal distress, infection, postpartum hemorrhage |
| Onset | During childbirth |
| Duration | More than 20 hours (first-time mothers), more than 14 hours (subsequent births) |
| Types | Prolonged latent phase, prolonged active phase |
| Causes | Cephalopelvic disproportion, malpresentation, ineffective uterine contractions |
| Risks | First-time pregnancy, epidural anesthesia, induction of labor |
| Diagnosis | Cervical dilation less than 1.2 cm per hour in first-time mothers, less than 1.5 cm per hour in women who have given birth before |
| Differential diagnosis | Braxton Hicks contractions, false labor |
| Prevention | Proper prenatal care, exercise, hydration |
| Treatment | Oxytocin, amniotomy, cesarean section |
| Medication | Oxytocin |
| Prognosis | Generally good with appropriate intervention |
| Frequency | Occurs in approximately 8% of all pregnancies |
| Deaths | Rare with modern medical care |
Prolonged labor, also known as failure to progress, is a term used in obstetrics to describe a labor that is taking longer than expected. This condition can occur during the first stage of labor, the second stage of labor, or both. Prolonged labor can pose risks to both the mother and the fetus, and it often requires medical intervention to ensure a safe delivery.
Causes[edit]
Several factors can contribute to prolonged labor, including:
- Cephalopelvic disproportion (CPD) - when the baby's head is too large to pass through the mother's pelvis.
- Malpresentation - abnormal positioning of the baby, such as breech or transverse lie.
- Uterine inertia - weak or uncoordinated uterine contractions.
- Maternal exhaustion - fatigue in the mother, which can slow down the labor process.
- Epidural anesthesia - while it provides pain relief, it can sometimes slow down labor.
Diagnosis[edit]
Prolonged labor is typically diagnosed through regular monitoring of the labor process. This includes:
- Cervical dilation - measuring the opening of the cervix.
- Effacement - thinning of the cervix.
- Fetal descent - the baby's movement down the birth canal.
- Contraction pattern - frequency, duration, and strength of uterine contractions.
Management[edit]
Management of prolonged labor depends on the underlying cause and the stage of labor. Common interventions include:
- Oxytocin - a hormone administered to stimulate stronger contractions.
- Amniotomy - artificially breaking the water to speed up labor.
- Assisted delivery - using tools like forceps or a vacuum extractor.
- Cesarean section - surgical delivery of the baby if vaginal delivery is not possible.
Risks and Complications[edit]
Prolonged labor can lead to several complications, such as:
- Maternal infection - increased risk of infection for the mother.
- Fetal distress - decreased oxygen supply to the baby.
- Postpartum hemorrhage - excessive bleeding after delivery.
- Uterine rupture - a rare but serious complication.
Prevention[edit]
While not all cases of prolonged labor can be prevented, certain measures can help reduce the risk:
- Regular prenatal care to monitor the health of the mother and baby.
- Proper management of maternal conditions like gestational diabetes and hypertension.
- Encouraging the mother to stay active and maintain a healthy diet during pregnancy.
See also[edit]
See also[edit]
| Obstetrics | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
This obstetrics-related article is a stub.
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian