Amiodarone induced thyrotoxicosis

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
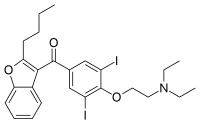
| Amiodarone-induced thyrotoxicosis | |
|---|---|
| |
| Synonyms | AIT |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Hyperthyroidism, weight loss, palpitations, tremor, anxiety, heat intolerance |
| Complications | Thyroid storm, heart failure, atrial fibrillation |
| Onset | Variable, often months after starting amiodarone |
| Duration | Can be prolonged, depending on treatment |
| Types | N/A |
| Causes | Amiodarone use |
| Risks | Pre-existing thyroid disease, high iodine intake |
| Diagnosis | Thyroid function tests, ultrasound, radioiodine uptake test |
| Differential diagnosis | Graves' disease, toxic multinodular goiter |
| Prevention | Monitoring thyroid function before and during amiodarone therapy |
| Treatment | Antithyroid drugs, corticosteroids, thyroidectomy |
| Medication | Methimazole, propylthiouracil, prednisone |
| Prognosis | N/A |
| Frequency | 10-20% of patients on amiodarone |
| Deaths | Rare, but can occur if untreated |
Amiodarone induced thyrotoxicosis (AIT) is a form of thyrotoxicosis that occurs as a result of treatment with the antiarrhythmic medication amiodarone. Amiodarone is commonly used to treat and prevent a variety of cardiac arrhythmias, but it can have significant effects on the thyroid gland due to its high iodine content and direct toxic effects on thyroid cells.
Pathophysiology[edit]
Amiodarone contains a large amount of iodine, approximately 37% by weight, which can lead to alterations in thyroid function. The drug can cause both hypothyroidism and thyrotoxicosis. AIT is classified into two main types:
- Type 1 AIT: This type occurs in patients with pre-existing thyroid abnormalities, such as nodular goiter or latent Graves' disease. The excess iodine from amiodarone leads to increased synthesis of thyroid hormones.
- Type 2 AIT: This type is a destructive thyroiditis, where amiodarone causes direct damage to thyroid follicular cells, leading to the release of preformed thyroid hormones into the circulation.
Clinical Features[edit]
Patients with AIT may present with symptoms of thyrotoxicosis, which can include:
The clinical presentation can vary depending on the type of AIT and the underlying cardiac condition being treated with amiodarone.
Diagnosis[edit]
The diagnosis of AIT is based on clinical suspicion, laboratory tests, and imaging studies. Key diagnostic steps include:
- Measurement of serum thyroid-stimulating hormone (TSH), free thyroxine (FT4), and free triiodothyronine (FT3) levels.
- Thyroid ultrasound to assess the gland's structure and identify nodules or goiter.
- Radioiodine uptake test to differentiate between Type 1 and Type 2 AIT, although this test is often limited by the iodine load from amiodarone.
Management[edit]
The management of AIT depends on the type and severity of the condition:
- Type 1 AIT: Treatment may involve the use of thionamides such as methimazole or propylthiouracil to reduce thyroid hormone synthesis. Potassium perchlorate may also be used to block iodine uptake.
- Type 2 AIT: Treatment typically involves the use of glucocorticoids, such as prednisone, to reduce inflammation and hormone release.
In some cases, discontinuation of amiodarone may be necessary, although this must be balanced against the risk of exacerbating the underlying cardiac condition.
Prognosis[edit]
The prognosis of AIT varies depending on the type and the patient's response to treatment. Type 2 AIT often resolves more quickly with appropriate therapy, while Type 1 AIT may require prolonged treatment and monitoring.
See Also[edit]
| Physiology of the endocrine system | ||||||||
|---|---|---|---|---|---|---|---|---|
|
0
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian