Fetal thrombotic vasculopathy

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Fetal thrombotic vasculopathy | |
|---|---|

| |
| Synonyms | Fetal thrombotic vasculopathy (FTV) |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | N/A |
| Complications | Intrauterine growth restriction, Stillbirth, Cerebral palsy |
| Onset | Prenatal |
| Duration | Chronic |
| Types | N/A |
| Causes | Thrombosis in the fetal circulation |
| Risks | Maternal diabetes, Thrombophilia, Placental insufficiency |
| Diagnosis | Histopathology of the placenta |
| Differential diagnosis | Villitis of unknown etiology, Chorioamnionitis |
| Prevention | Management of maternal risk factors |
| Treatment | None specific; supportive care |
| Medication | N/A |
| Prognosis | Variable, depends on severity and associated conditions |
| Frequency | Unknown, considered rare |
| Deaths | N/A |

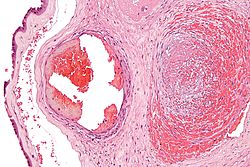
File:Fetal thrombotic vasculopathy - very high mag.jpg Fetal Thrombotic Vasculopathy (FTV) is a pathological condition affecting the placenta that can have significant implications for fetal development and outcomes. It is characterized by the presence of thrombosis (blood clots) within the fetal vessels of the placenta, leading to compromised blood flow and oxygen delivery to the fetus. This condition is associated with a range of adverse fetal outcomes, including intrauterine growth restriction (IUGR), fetal distress, and in severe cases, stillbirth.
Etiology[edit]
The exact cause of Fetal Thrombotic Vasculopathy is not fully understood, but it is believed to be multifactorial. Factors that may contribute to the development of FTV include maternal conditions such as diabetes mellitus, hypertension, and antiphospholipid syndrome, as well as fetal factors like genetic thrombophilias. Infections and placental insufficiency have also been implicated in the pathogenesis of FTV.
Pathophysiology[edit]
FTV involves the formation of blood clots within the small blood vessels of the placenta, particularly affecting the villous capillaries and stem vessels. This leads to reduced blood flow and oxygen exchange between the maternal and fetal circulations. The resultant hypoxia and ischemia can cause necrosis of placental tissue and impact fetal development. The condition can be focal, affecting limited areas of the placenta, or widespread, leading to significant placental dysfunction.
Clinical Features and Diagnosis[edit]
FTV is often asymptomatic and may only be diagnosed postnatally through histopathological examination of the placenta. In some cases, signs of fetal distress or IUGR may prompt further investigation. Ultrasound and Doppler studies can suggest placental insufficiency, but definitive diagnosis requires placental pathology.
Management and Prognosis[edit]
Management of Fetal Thrombotic Vasculopathy primarily focuses on monitoring and addressing any underlying maternal conditions. Close surveillance of fetal well-being through non-stress tests, biophysical profiles, and Doppler ultrasound assessments is crucial. In severe cases, early delivery may be considered to prevent adverse outcomes. The prognosis of FTV depends on the extent of placental involvement and the presence of any underlying maternal or fetal conditions. Early detection and management are key to improving outcomes.
Prevention[edit]
Preventive strategies for Fetal Thrombotic Vasculopathy include optimal management of maternal health conditions, such as control of diabetes and hypertension, and treatment of any identified thrombophilias with anticoagulation therapy. Prenatal care and regular monitoring of high-risk pregnancies are essential for early detection and intervention.
Images[edit]
-
Fetal thrombotic vasculopathy - low magnification
-
Fetal thrombotic vasculopathy - high magnification
-
Fetal thrombotic vasculopathy - very high magnification
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian

