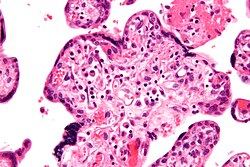
Villitis of unknown etiology

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Villitis of unknown etiology | |
|---|---|
 | |
| Synonyms | Chronic villitis |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Often asymptomatic, may be associated with intrauterine growth restriction |
| Complications | Recurrent pregnancy loss, fetal growth restriction |
| Onset | During pregnancy |
| Duration | Variable |
| Types | N/A |
| Causes | Unknown |
| Risks | Previous history of villitis, autoimmune disorders |
| Diagnosis | Histopathology of the placenta |
| Differential diagnosis | Infectious villitis, chronic histiocytic intervillositis |
| Prevention | None known |
| Treatment | None specific, management of pregnancy complications |
| Medication | N/A |
| Prognosis | Variable, depends on severity and recurrence |
| Frequency | Estimated in 5-15% of placentas |
| Deaths | N/A |
Villitis of unknown etiology (VUE) is a pathological condition affecting the placenta, specifically the chorionic villi, which are essential for nutrient and gas exchange between the mother and fetus. VUE is characterized by inflammation of the villi, and as the name suggests, its cause remains largely unknown. This condition can have significant implications for both maternal and fetal health, potentially leading to poor pregnancy outcomes such as fetal growth restriction, preterm birth, and stillbirth.
Etiology[edit]
The exact cause of VUE is not well understood, which is why it is termed "of unknown etiology." However, it is thought to be an immune-mediated process. Some researchers suggest that it may be related to maternal immune response to fetal antigens, possibly involving maternal-fetal HLA incompatibility. There is also speculation that undiagnosed or subclinical infections could play a role in its development.
Pathophysiology[edit]
In VUE, there is a chronic inflammatory infiltrate within the chorionic villi. This infiltrate is primarily composed of T lymphocytes, macrophages, and occasionally plasma cells. The inflammation can lead to villous damage and fibrosis, impairing the placenta's ability to support the growing fetus adequately. The exact mechanism by which this inflammation leads to adverse pregnancy outcomes is not fully understood but is believed to involve compromised placental function due to the inflammatory damage.
Clinical Presentation[edit]
VUE is typically asymptomatic and is most often diagnosed postpartum through histopathological examination of the placenta. In some cases, it may be associated with intrauterine growth restriction (IUGR), small for gestational age (SGA) infants, preterm birth, and increased risk of stillbirth. It is also associated with a higher incidence of preeclampsia and maternal vascular malperfusion.
Diagnosis[edit]
The diagnosis of VUE is made histologically by examining placental tissue, usually after delivery. The presence of inflammatory cells within the chorionic villi, along with associated villous damage and fibrosis, is indicative of the condition. There are no specific antenatal diagnostic tests available due to its asymptomatic nature in most cases.
Treatment and Management[edit]
There is no specific treatment for VUE. Management strategies are generally focused on monitoring and addressing any complications that may arise during the pregnancy. This includes close surveillance for fetal growth restriction and other signs of fetal distress. In some cases, early delivery may be considered to prevent adverse outcomes.
Prognosis[edit]
The prognosis for pregnancies affected by VUE varies. While some pregnancies may proceed without significant complications, others may be at increased risk for adverse outcomes such as fetal growth restriction, preterm birth, and stillbirth. The severity of the inflammation and the extent of placental involvement appear to be key factors influencing the prognosis.
Prevention[edit]
Given the unknown etiology of VUE, specific preventive measures are not well established. However, general good prenatal care and early detection of potential complications through routine antenatal visits may help in managing the risks associated with this condition.
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian