Long-chain 3-hydroxyacyl-coenzyme A dehydrogenase deficiency

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Long-chain 3-hydroxyacyl-coenzyme A dehydrogenase deficiency | |
|---|---|
| |
| Synonyms | LCHAD deficiency |
| Pronounce | |
| Specialty | Medical genetics |
| Symptoms | Hypoglycemia, cardiomyopathy, muscle weakness, liver dysfunction |
| Complications | N/A |
| Onset | Infancy |
| Duration | Lifelong |
| Types | N/A |
| Causes | Mutations in the HADHA gene |
| Risks | |
| Diagnosis | Genetic testing, newborn screening |
| Differential diagnosis | Medium-chain acyl-CoA dehydrogenase deficiency, trifunctional protein deficiency |
| Prevention | |
| Treatment | Dietary management, medium-chain triglycerides |
| Medication | |
| Prognosis | Variable, can be life-threatening if untreated |
| Frequency | Rare |
| Deaths | |
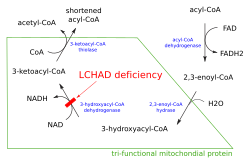
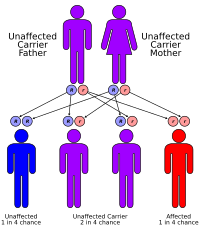
Long-chain 3-hydroxyacyl-coenzyme A dehydrogenase deficiency (LCHAD deficiency) is a rare genetic disorder that affects the breakdown of certain fats in the body. It is classified as a fatty acid oxidation disorder (FAOD) and is caused by mutations in the HADHA gene, which provides instructions for making an enzyme called long-chain 3-hydroxyacyl-coenzyme A dehydrogenase.
Symptoms[edit]
Individuals with LCHAD deficiency may experience a range of symptoms, which can vary in severity. Common symptoms include:
- Muscle weakness
- Low blood sugar
- Enlarged liver
- Heart problems
- Vision problems
- Developmental delays
- Neurological abnormalities
Diagnosis[edit]
Diagnosing LCHAD deficiency involves a combination of clinical evaluation, biochemical testing, and genetic testing. Blood tests can reveal elevated levels of certain fatty acids and organic acids, which can help in the diagnosis. Genetic testing can confirm the presence of mutations in the HADHA gene.
Treatment[edit]
There is currently no cure for LCHAD deficiency, but treatment focuses on managing symptoms and preventing complications. This may involve:
- Dietary modifications: Individuals with LCHAD deficiency may need to follow a special diet that is low in long-chain fatty acids and high in carbohydrates. This can help prevent the buildup of toxic byproducts and provide alternative energy sources for the body.
- Supplementation: Some individuals may require specific supplements, such as carnitine or medium-chain triglycerides, to support their metabolism and overall health.
- Monitoring and support: Regular monitoring of blood markers and close medical supervision are essential to manage the condition effectively. Supportive therapies, such as physical therapy and occupational therapy, may also be beneficial.
Prognosis[edit]
The prognosis for individuals with LCHAD deficiency can vary depending on the severity of the condition and the age of onset. Early diagnosis and appropriate management can significantly improve outcomes. However, some individuals may experience long-term complications, such as heart problems or neurological impairments.
Research[edit]
Ongoing research is focused on understanding the underlying mechanisms of LCHAD deficiency and developing new treatment strategies. This includes investigating potential gene therapies, enzyme replacement therapies, and targeted drug interventions.