Acute intermittent porphyria
| Acute intermittent porphyria | |
|---|---|
 | |
| Synonyms | AIP |
| Pronounce | |
| Specialty | Hematology, Genetics |
| Symptoms | Abdominal pain, vomiting, neuropathy, constipation, confusion |
| Complications | N/A |
| Onset | Typically after puberty |
| Duration | Episodic |
| Types | N/A |
| Causes | Genetic mutation in the HMBS gene |
| Risks | Hormonal changes, medications, alcohol, fasting |
| Diagnosis | Urine test for porphobilinogen |
| Differential diagnosis | Lead poisoning, Guillain–Barré syndrome, appendicitis |
| Prevention | N/A |
| Treatment | Intravenous glucose, heme arginate |
| Medication | Hemin |
| Prognosis | Variable, can be life-threatening if untreated |
| Frequency | 5-10 per 100,000 people |
| Deaths | Rare with treatment |
Other Names: AIP; Porphobilinogen deaminase deficiency; PBGD deficiency; Uroporphyrinogen synthase deficiency; UPS deficiency; Porphyria, Swedish type; Hydroxymethylbilane synthase deficiency; HMBS deficiency
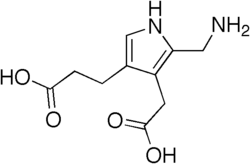
Acute intermittent porphyria (AIP) is one of the liver (hepatic) porphyrias. AIP is caused by low levels of porphobilinogen deaminase (PBGD), an enzyme also often called hydroxymethylbilane synthase. The low levels of PBGD are generally not sufficient to cause symptoms; however, activating factors such as hormones, drugs, and dietary changes may trigger symptoms. Although most individuals with AIP never develop symptoms, symptomatic individuals typically present with abdominal pain with nausea.
Cause [edit]
AIP is caused by the deficiency of an enzyme  called porphobilinogen deaminase (PBGD), also known as hydroxymethylbilane synthase (HMBS) and formerly known as uroporphyrinogen I-synthase. The deficiency of PBGD is caused by a mutation in the ''HMBS''gene . The HMBS gene is the only gene known to be associated with AIP. However, the deficiency of PBGD alone is not enough to cause AIP. Other activating factors (e.g.,harmones, drugs, dietary changes) must also be present.
Inheritance[edit]

AIP is inherited in an autosomal dominant fashion, which means only one of the two ''HMBS''genes needs to have a disease-causing mutation  to decrease enzyme activity and cause symptoms.
Diagnosis[edit]
Diagnosis of AIP is suspected in individuals with otherwise unexplained severe, acute abdominal pain without physical signs. The finding of increased levels of delta-aminolevulinic acid (ALA) and porphobilinogen (PBG) in urine establishes that one of the acute porphyrias is present. If PBGD is deficient in normal red blod cells, the diagnosis of AIP is established. The diagnosis is confirmed in individuals with a disease-causing mutation in the HMBSgene , the only gene known to be associated with AIP, which encodes the erythrocyte hydroxymethylbilane synthase .
Molecular genetic testing of the HMBS gene detects more than 98% of affected individuals and is available in clinical laboratories.
Treatment[edit]
Treatment of AIP may vary based on the trigger of the attack and the symptoms present. Treatment may include stopping medications that cause or worsen the symptoms, treating any infections which may be present, administration of pain medication, monitoring fluid balance and/or correcting electrolyte disturbances, monitoring neurologic status and administering respiratory support. Mild attacks can be manged with increased caloric intake and fluid replacement. Recurrent acute attacks should be managed by a porphyria specialist. Hospitalization is often necessary.
Panhematin, an intravenous medication used to correct heme deficiency, may also be prescribed.
The medication(s) listed below have been approved by the Food and Drug Administration (FDA) as orphan products for treatment of this condition.
- Hemin (Brand name: Panhematin)
External links[edit]
| Heme metabolism disorders | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
NIH genetic and rare disease info[edit]
Acute intermittent porphyria is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Acute intermittent porphyria
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian