Bariatric surgery




Bariatric surgery refers to a variety of surgical procedures performed to facilitate weight loss in individuals with severe obesity. These procedures alter the digestive system to either restrict food intake, reduce nutrient absorption, or both. Bariatric surgery is an effective treatment for obesity-related conditions such as type 2 diabetes, hypertension, and obstructive sleep apnea.
Indications
Bariatric surgery is recommended for patients who meet the following criteria:
- Body Mass Index (BMI) ≥40 kg/m², or
- BMI ≥35 kg/m² with obesity-related comorbidities, such as:
- Type 2 diabetes mellitus
- Hypertension
- Dyslipidemia
- Obstructive sleep apnea
- Non-alcoholic fatty liver disease (NAFLD)
- Failure of non-surgical weight loss methods, including diet, exercise, and pharmacotherapy.
Types of Bariatric Surgery
Bariatric procedures can be classified into restrictive, malabsorptive, and combined techniques.
1. Restrictive Procedures
These surgeries limit the stomach’s capacity, reducing food intake.
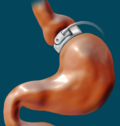
- Laparoscopic Adjustable Gastric Banding (LAGB):
- A silicone band is placed around the upper stomach, creating a small pouch.
- Adjustability allows modification of restriction over time.
- Pros: Reversible, adjustable, minimally invasive.
- Cons: Risk of band slippage, erosion, and less weight loss compared to other procedures.
- Sleeve Gastrectomy (SG):
- Approximately 80% of the stomach is removed, leaving a tubular gastric remnant.
- Reduces ghrelin secretion, leading to decreased appetite.
- Pros: No foreign body, no malabsorption, effective weight loss.
- Cons: Irreversible, risk of leakage, vitamin deficiencies.
2. Malabsorptive Procedures
These surgeries bypass part of the small intestine, reducing calorie and nutrient absorption.
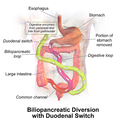
- Biliopancreatic Diversion with Duodenal Switch (BPD/DS):
- A portion of the stomach is removed, and the small intestine is rerouted.
- Pros: Significant weight loss, high resolution of metabolic diseases.
- Cons: High risk of nutritional deficiencies, malabsorption, and diarrhea.
3. Combination Procedures
These involve both restriction and malabsorption mechanisms.
- Roux-en-Y Gastric Bypass (RYGB):
- Creates a small gastric pouch that bypasses most of the stomach and the proximal small intestine.
- Pros: High long-term weight loss, improvement in metabolic conditions.
- Cons: Risk of dumping syndrome, micronutrient deficiencies, and marginal ulcers.
Mechanisms of Action
Bariatric surgery leads to weight loss and metabolic improvement via:
- Caloric restriction – Reduced stomach volume limits intake.
- Malabsorption – Decreased absorption of nutrients in the small intestine.
- Hormonal changes – Altered secretion of ghrelin, GLP-1, and PYY, leading to improved insulin sensitivity and appetite suppression.
- Gut microbiota modification – Changes in intestinal flora contribute to metabolic benefits.
Benefits
Bariatric surgery results in multiple health improvements:
- Weight loss – 50-80% excess weight loss within 2 years.
- Remission of Type 2 Diabetes – Many patients experience complete resolution of diabetes.
- Reduction in Cardiovascular Risk – Lower blood pressure and cholesterol levels.
- Improved Quality of Life – Enhanced mobility, mental health, and self-esteem.
- Lower Mortality Rate – Reduced long-term risk of obesity-related deaths.
Risks and Complications
Despite its benefits, bariatric surgery carries risks:
- Early postoperative complications:
- Anastomotic leak
- Bleeding
- Deep vein thrombosis (DVT) and pulmonary embolism (PE)
- Long-term complications:
- Malnutrition (Vitamin B12, Iron, Calcium, Folate deficiencies)
- Dumping syndrome (rapid gastric emptying leading to nausea, diarrhea, hypoglycemia)
- Gallstones due to rapid weight loss
- Marginal ulcers
Preoperative Evaluation
A thorough preoperative assessment is required to optimize patient outcomes:
- Medical Evaluation – Assess comorbidities and nutritional status.
- Psychological Assessment – Screen for eating disorders and mental health conditions.
- Nutritional Counseling – Education on dietary changes post-surgery.
- Lifestyle Modifications – Encouragement of physical activity and behavioral therapy.
Postoperative Care
- Dietary Phases:
- Phase 1: Clear liquids (first few days)
- Phase 2: Pureed foods (weeks 1-2)
- Phase 3: Soft foods (weeks 3-4)
- Phase 4: Regular diet (after 4-6 weeks)
- Nutritional Supplements:
- Lifelong vitamin and mineral supplementation (B12, iron, calcium, vitamin D).
- Regular Follow-ups:
- Monitor weight loss, nutritional deficiencies, and comorbidities.
Contraindications
Bariatric surgery is not recommended for:
- Severe, untreated psychiatric disorders.
- Active substance abuse.
- Inability to comply with lifelong dietary changes.
- Uncontrolled medical conditions making surgery unsafe.
Emerging Trends in Bariatric Surgery
- Endoscopic Bariatric Procedures – Less invasive alternatives such as gastric balloons.
- Metabolic Surgery – Bariatric surgery for diabetes control, even in non-obese patients.
- Robotic-Assisted Surgery – Improves precision and reduces complications.
Gallery
-
Bariatric surgery
-
Bariatric surgery
-
Bariatric surgery
See Also
| Surgery | ||||
|---|---|---|---|---|
|
Ad. Transform your life with W8MD's
GLP-1 weight loss injections special from $29.99 with insurance
|
WikiMD Medical Encyclopedia |
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian