Bullous pemphigoid: Difference between revisions
mNo edit summary |
CSV import |
||
| Line 1: | Line 1: | ||
{{SI}} | |||
[[File:Bullous pemphigoid new image.jpg|thumb|Bullous pemphigoid new image]] | {{Infobox medical condition | ||
| name = Bullous pemphigoid | |||
| image = [[File:Legs_Bullous_Pemphigoid.jpg|alt=Legs with bullous pemphigoid]] | |||
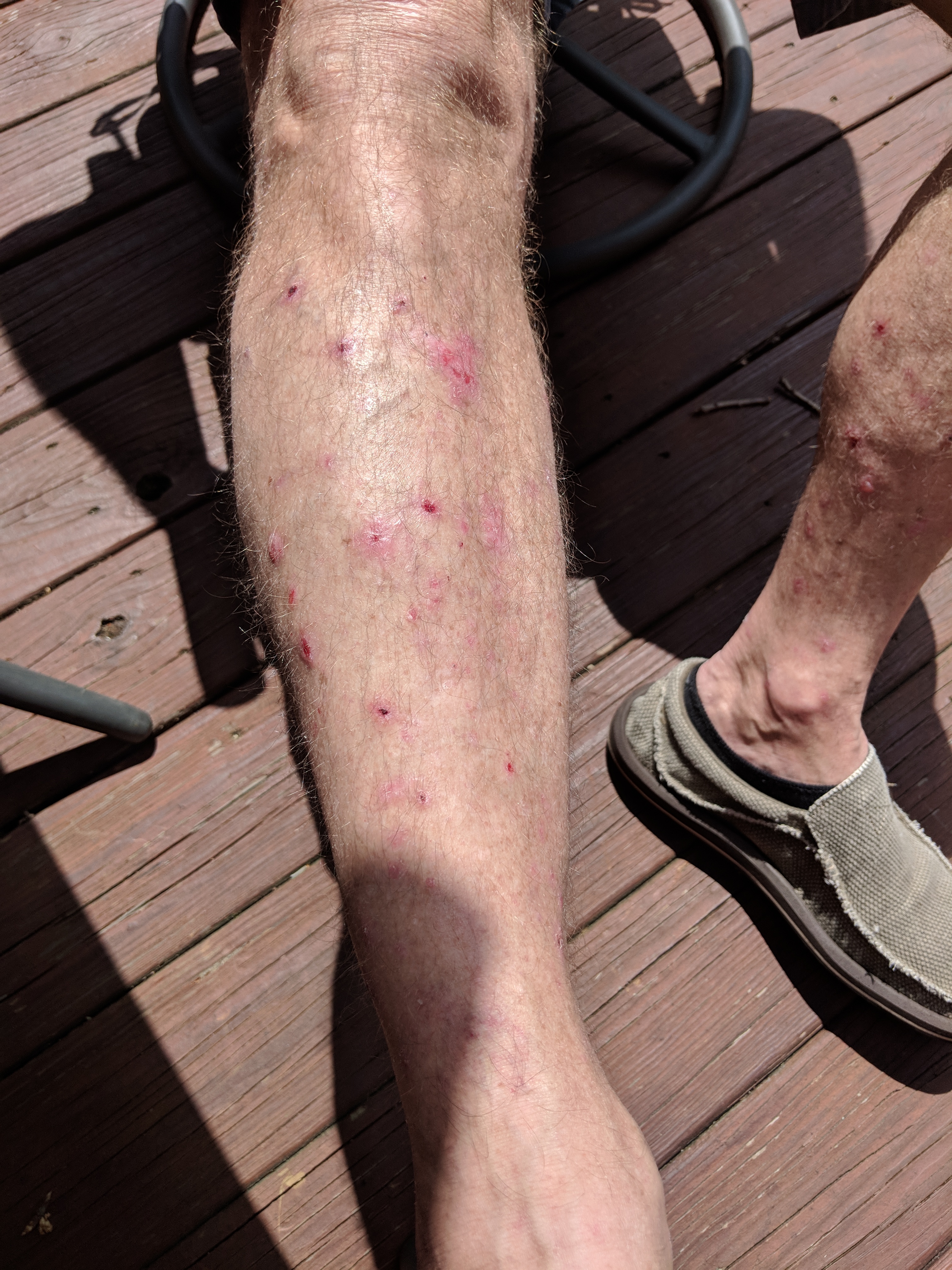
| caption = Legs affected by bullous pemphigoid | |||
| synonyms = | |||
| pronounce = | |||
| specialty = [[Dermatology]] | |||
| symptoms = [[Blister]]s, [[itching]], [[rash]] | |||
| complications = [[Infection]], [[scarring]] | |||
| onset = Typically in older adults | |||
| duration = Chronic | |||
| causes = [[Autoimmune disease]] | |||
| risks = Age, [[genetic predisposition]], certain [[medications]] | |||
| diagnosis = [[Skin biopsy]], [[direct immunofluorescence]] | |||
| differential = [[Pemphigus vulgaris]], [[dermatitis herpetiformis]], [[epidermolysis bullosa]] | |||
| prevention = | |||
| treatment = [[Corticosteroids]], [[immunosuppressants]] | |||
| medication = [[Prednisone]], [[azathioprine]], [[methotrexate]] | |||
| prognosis = Generally good with treatment | |||
| frequency = Rare | |||
}} | |||
[[File:Bullous pemphigoid new image.jpg|left|thumb|Bullous pemphigoid new image]] | |||
'''Bullous Pemphigoid''' is a chronic [[autoimmune disease]] that primarily affects the skin, causing the formation of large, tense blisters. It is most common in older adults and is characterized by periods of remission and relapse. | '''Bullous Pemphigoid''' is a chronic [[autoimmune disease]] that primarily affects the skin, causing the formation of large, tense blisters. It is most common in older adults and is characterized by periods of remission and relapse. | ||
==Etiology== | ==Etiology== | ||
The exact cause of bullous pemphigoid is unknown, but it is believed to be an autoimmune response. The body's immune system produces [[antibodies]] that attack the skin's basement membrane, a thin layer of tissue that separates the outer skin from the underlying tissues. This attack results in inflammation and the formation of blisters. | The exact cause of bullous pemphigoid is unknown, but it is believed to be an autoimmune response. The body's immune system produces [[antibodies]] that attack the skin's basement membrane, a thin layer of tissue that separates the outer skin from the underlying tissues. This attack results in inflammation and the formation of blisters. | ||
<youtube> | <youtube> | ||
title='''{{PAGENAME}}''' | title='''{{PAGENAME}}''' | ||
| Line 17: | Line 35: | ||
height=600 | height=600 | ||
</youtube> | </youtube> | ||
==Symptoms== | ==Symptoms== | ||
The primary symptom of bullous pemphigoid is the appearance of large, tense blisters on the skin. These blisters are usually filled with clear fluid and can appear anywhere on the body, but are most common on the arms, legs, and trunk. Other symptoms may include itching, redness, and hives. | The primary symptom of bullous pemphigoid is the appearance of large, tense blisters on the skin. These blisters are usually filled with clear fluid and can appear anywhere on the body, but are most common on the arms, legs, and trunk. Other symptoms may include itching, redness, and hives. | ||
==Diagnosis== | ==Diagnosis== | ||
Diagnosis of bullous pemphigoid is typically made through a combination of clinical examination, [[skin biopsy]], and blood tests. The skin biopsy can reveal the presence of the characteristic blisters and the blood tests can detect the presence of the specific antibodies associated with the disease. | Diagnosis of bullous pemphigoid is typically made through a combination of clinical examination, [[skin biopsy]], and blood tests. The skin biopsy can reveal the presence of the characteristic blisters and the blood tests can detect the presence of the specific antibodies associated with the disease. | ||
==Treatment== | ==Treatment== | ||
Treatment for bullous pemphigoid primarily involves managing the symptoms and preventing complications. This may include the use of topical or oral [[corticosteroids]] to reduce inflammation and suppress the immune response. In severe cases, other immunosuppressive drugs may be used. | Treatment for bullous pemphigoid primarily involves managing the symptoms and preventing complications. This may include the use of topical or oral [[corticosteroids]] to reduce inflammation and suppress the immune response. In severe cases, other immunosuppressive drugs may be used. | ||
==Prognosis== | ==Prognosis== | ||
The prognosis for bullous pemphigoid varies. Some individuals may experience periods of remission, while others may have persistent symptoms. With treatment, most individuals can manage their symptoms and maintain a good quality of life. | The prognosis for bullous pemphigoid varies. Some individuals may experience periods of remission, while others may have persistent symptoms. With treatment, most individuals can manage their symptoms and maintain a good quality of life. | ||
==See Also== | ==See Also== | ||
* [[Dermatology]] | * [[Dermatology]] | ||
* [[Autoimmune diseases]] | * [[Autoimmune diseases]] | ||
* [[Corticosteroids]] | * [[Corticosteroids]] | ||
[[Category:Medicine]] | [[Category:Medicine]] | ||
[[Category:Dermatology]] | [[Category:Dermatology]] | ||
[[Category:Autoimmune diseases]] | [[Category:Autoimmune diseases]] | ||
{{medicine-stub}} | {{medicine-stub}} | ||
{{dermatology-stub}} | {{dermatology-stub}} | ||
{{autoimmune diseases-stub}} | {{autoimmune diseases-stub}} | ||
Latest revision as of 19:20, 4 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Bullous pemphigoid | |
|---|---|
| |
| Synonyms | |
| Pronounce | |
| Specialty | Dermatology |
| Symptoms | Blisters, itching, rash |
| Complications | Infection, scarring |
| Onset | Typically in older adults |
| Duration | Chronic |
| Types | N/A |
| Causes | Autoimmune disease |
| Risks | Age, genetic predisposition, certain medications |
| Diagnosis | Skin biopsy, direct immunofluorescence |
| Differential diagnosis | Pemphigus vulgaris, dermatitis herpetiformis, epidermolysis bullosa |
| Prevention | |
| Treatment | Corticosteroids, immunosuppressants |
| Medication | Prednisone, azathioprine, methotrexate |
| Prognosis | Generally good with treatment |
| Frequency | Rare |
| Deaths | N/A |

Bullous Pemphigoid is a chronic autoimmune disease that primarily affects the skin, causing the formation of large, tense blisters. It is most common in older adults and is characterized by periods of remission and relapse.
Etiology[edit]
The exact cause of bullous pemphigoid is unknown, but it is believed to be an autoimmune response. The body's immune system produces antibodies that attack the skin's basement membrane, a thin layer of tissue that separates the outer skin from the underlying tissues. This attack results in inflammation and the formation of blisters.
Symptoms[edit]
The primary symptom of bullous pemphigoid is the appearance of large, tense blisters on the skin. These blisters are usually filled with clear fluid and can appear anywhere on the body, but are most common on the arms, legs, and trunk. Other symptoms may include itching, redness, and hives.
Diagnosis[edit]
Diagnosis of bullous pemphigoid is typically made through a combination of clinical examination, skin biopsy, and blood tests. The skin biopsy can reveal the presence of the characteristic blisters and the blood tests can detect the presence of the specific antibodies associated with the disease.
Treatment[edit]
Treatment for bullous pemphigoid primarily involves managing the symptoms and preventing complications. This may include the use of topical or oral corticosteroids to reduce inflammation and suppress the immune response. In severe cases, other immunosuppressive drugs may be used.
Prognosis[edit]
The prognosis for bullous pemphigoid varies. Some individuals may experience periods of remission, while others may have persistent symptoms. With treatment, most individuals can manage their symptoms and maintain a good quality of life.
See Also[edit]

This article is a dermatology stub. You can help WikiMD by expanding it!
This article is a Autoimmune disease-related stub. You can help WikiMD by expanding it!
