Intrauterine hypoxia

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Intrauterine hypoxia | |
|---|---|
| File:Placental infarct - intermed mag.jpg | |
| Synonyms | Fetal hypoxia, fetal oxygen deprivation |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Fetal distress, abnormal heart rate, reduced fetal movements |
| Complications | Cerebral palsy, developmental delay, intrauterine growth restriction |
| Onset | During pregnancy |
| Duration | Variable |
| Types | N/A |
| Causes | Placental insufficiency, umbilical cord compression, maternal hypoxia |
| Risks | Maternal smoking, preeclampsia, diabetes mellitus |
| Diagnosis | Fetal heart rate monitoring, ultrasound, biophysical profile |
| Differential diagnosis | Fetal anemia, congenital heart defect |
| Prevention | Prenatal care, smoking cessation, management of maternal conditions |
| Treatment | Oxygen therapy, emergency cesarean section, intrauterine resuscitation |
| Medication | N/A |
| Prognosis | Depends on severity and duration |
| Frequency | Common |
| Deaths | N/A |
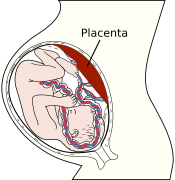
Intrauterine hypoxia is a medical condition that occurs when the fetus does not receive enough oxygen while in the womb. This can lead to a variety of complications, including birth defects, developmental delays, and stillbirth.
Causes[edit]
Intrauterine hypoxia can be caused by a number of factors, including:
- Placental insufficiency: This occurs when the placenta does not function properly, preventing the fetus from receiving enough oxygen.
- Umbilical cord complications: Problems with the umbilical cord, such as a knot or a cord that is wrapped around the baby's neck, can restrict oxygen flow.
- Maternal health problems: Conditions such as high blood pressure, diabetes, and heart disease can affect the amount of oxygen the fetus receives.
- Pregnancy complications: Complications during pregnancy, such as preeclampsia or gestational diabetes, can also lead to intrauterine hypoxia.
Symptoms[edit]
The symptoms of intrauterine hypoxia can vary depending on the severity of the condition. They may include:
- Reduced movements of the fetus
- Low heart rate in the fetus
- Abnormal heart rhythm in the fetus
- Poor growth in the womb
Diagnosis[edit]
Intrauterine hypoxia can be diagnosed through a variety of tests, including:
- Ultrasound: This imaging test can show if the fetus is moving less than normal or if there are problems with the placenta or umbilical cord.
- Fetal heart rate monitoring: This test measures the heart rate of the fetus and can show if it is lower than normal.
- Doppler ultrasound: This test can show if there is reduced blood flow to the fetus.
Treatment[edit]
The treatment for intrauterine hypoxia depends on the cause and severity of the condition. It may include:
- Delivery of the baby: If the baby is in distress, it may be necessary to deliver the baby early.
- Medication: In some cases, medication may be given to the mother to improve the flow of oxygen to the fetus.
- Monitoring: The baby may need to be closely monitored to ensure they are receiving enough oxygen.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian