Portal hypertensive gastropathy

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Portal hypertensive gastropathy | |
|---|---|
| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Gastrointestinal bleeding, anemia |
| Complications | Chronic blood loss, iron deficiency anemia |
| Onset | Often associated with portal hypertension |
| Duration | Chronic |
| Types | N/A |
| Causes | Portal hypertension |
| Risks | Cirrhosis, liver disease |
| Diagnosis | Endoscopy |
| Differential diagnosis | Gastric antral vascular ectasia, peptic ulcer disease |
| Prevention | N/A |
| Treatment | Beta blockers, endoscopic therapy |
| Medication | Non-selective beta blockers |
| Prognosis | N/A |
| Frequency | Common in patients with cirrhosis |
| Deaths | N/A |

Portal hypertensive gastropathy is a medical condition characterized by changes in the mucosa of the stomach due to portal hypertension. It is often associated with cirrhosis of the liver and is a common cause of gastrointestinal bleeding.
Etiology[edit]
The exact cause of portal hypertensive gastropathy is not fully understood. However, it is believed to be related to increased pressure in the portal vein system, which is often caused by cirrhosis of the liver. Other potential causes include congestive heart failure, hepatic vein thrombosis, and schistosomiasis.
Pathophysiology[edit]
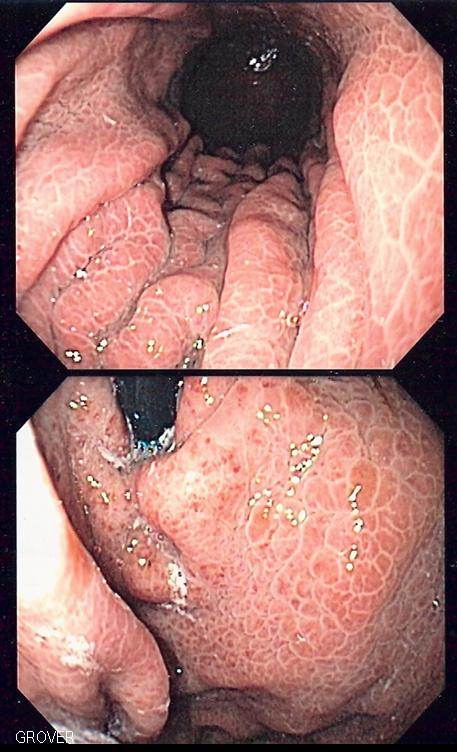
Portal hypertensive gastropathy is characterized by changes in the mucosa of the stomach. These changes include erythema, edema, and friability, as well as the presence of vascular ectasia and spider angiomata. The increased pressure in the portal vein system leads to dilation of the submucosal veins, which in turn leads to the characteristic changes in the mucosa.
Clinical Presentation[edit]
Patients with portal hypertensive gastropathy may present with a variety of symptoms, including anemia due to chronic gastrointestinal bleeding, melena, hematemesis, and epigastric pain. However, many patients are asymptomatic and the condition is often discovered incidentally during endoscopy.
Diagnosis[edit]
The diagnosis of portal hypertensive gastropathy is typically made via endoscopy, which allows for direct visualization of the characteristic changes in the mucosa. Other diagnostic tests may include laboratory tests to assess for anemia and liver function, as well as imaging studies to evaluate for cirrhosis and portal hypertension.
Treatment[edit]
The treatment of portal hypertensive gastropathy primarily involves managing the underlying cause of the portal hypertension. This may include treating the cirrhosis or congestive heart failure, or managing the hepatic vein thrombosis or schistosomiasis. In addition, patients may be treated with medications to reduce the pressure in the portal vein system and to manage the gastrointestinal bleeding.
Ad. Transform your health with W8MD Weight Loss, Sleep & MedSpa

Tired of being overweight?
Special offer:
Budget GLP-1 weight loss medications
- Semaglutide starting from $29.99/week and up with insurance for visit of $59.99 and up per week self pay.
- Tirzepatide starting from $45.00/week and up (dose dependent) or $69.99/week and up self pay
✔ Same-week appointments, evenings & weekends
Learn more:
- GLP-1 weight loss clinic NYC
- W8MD's NYC medical weight loss
- W8MD Philadelphia GLP-1 shots
- Philadelphia GLP-1 injections
- Affordable GLP-1 shots NYC
|
WikiMD Medical Encyclopedia |
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian
