Acute pancreatitis: Difference between revisions
CSV import |
CSV import |
||
| Line 84: | Line 84: | ||
[[Category:Pancreatic disorders]] | [[Category:Pancreatic disorders]] | ||
<gallery> | |||
File:3D_Medical_Animation_Acute_Pancreatitis.jpg|3D Medical Animation of Acute Pancreatitis | |||
File:Illu_pancrease.svg|Illustration of the Pancreas | |||
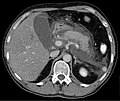
File:Akute_exsudative_Pankreatitis_-_CT_axial.jpg|CT Axial View of Acute Exudative Pancreatitis | |||
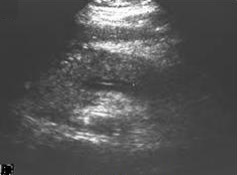
File:Ultrasonography_of_acute_pancreatitis.jpg|Ultrasonography of Acute Pancreatitis | |||
</gallery> | |||
Revision as of 05:02, 18 February 2025
Acute Pancreatitis

Acute pancreatitis is a sudden inflammation of the pancreas. It can be a mild, self-limiting condition or a severe, life-threatening illness. The pancreas is an organ located behind the stomach that plays a crucial role in digestion and blood sugar regulation.
Pathophysiology
Acute pancreatitis occurs when digestive enzymes produced by the pancreas become activated while still inside the organ, leading to autodigestion of pancreatic tissue. This process results in inflammation, edema, and in severe cases, necrosis of the pancreatic tissue. The release of these enzymes and inflammatory mediators can also affect other organs, leading to systemic complications.
Causes
The most common causes of acute pancreatitis include:
- Gallstones: These can block the bile duct, leading to pancreatic inflammation.
- Alcohol consumption: Heavy alcohol use is a significant risk factor.
- Hypertriglyceridemia: Elevated levels of triglycerides in the blood can precipitate pancreatitis.
- Medications: Certain drugs can induce pancreatitis as a side effect.
- Infections: Viral infections such as mumps can lead to pancreatitis.
Symptoms
The primary symptom of acute pancreatitis is severe abdominal pain, often described as a constant, dull, and boring pain that radiates to the back. Other symptoms may include:
- Nausea and vomiting
- Fever
- Tachycardia
- Abdominal tenderness
Diagnosis

Diagnosis of acute pancreatitis is based on clinical presentation, laboratory tests, and imaging studies. Key diagnostic criteria include:
- Elevated serum amylase and lipase levels
- Imaging studies such as CT scan or ultrasonography
Imaging

Imaging plays a crucial role in diagnosing and assessing the severity of acute pancreatitis. A CT scan can reveal pancreatic inflammation, necrosis, and complications such as pseudocysts. Ultrasonography is useful for detecting gallstones and assessing the biliary tree.
Treatment
The management of acute pancreatitis involves supportive care, including:
- Fluid resuscitation: To maintain adequate blood volume and prevent shock.
- Pain management: Using analgesics to control abdominal pain.
- Nutritional support: Initially, patients may be kept nil by mouth, with gradual reintroduction of oral intake as tolerated.
- Addressing the underlying cause: Such as removing gallstones or abstaining from alcohol.
Complications
Severe acute pancreatitis can lead to complications such as:
- Pancreatic necrosis
- Infection
- Pseudocyst formation
- Systemic inflammatory response syndrome (SIRS)
Prognosis
The prognosis of acute pancreatitis varies depending on the severity of the condition and the presence of complications. Mild cases often resolve with supportive care, while severe cases may require intensive medical intervention.
Related pages
Gallery
-
3D Medical Animation of Acute Pancreatitis
-
Illustration of the pancreas
-
CT scan showing acute exudative pancreatitis
-
Ultrasonography of acute pancreatitis
-
3D Medical Animation of Acute Pancreatitis
-
Illustration of the Pancreas
-
CT Axial View of Acute Exudative Pancreatitis
-
Ultrasonography of Acute Pancreatitis