Lamellar ichthyosis: Difference between revisions
CSV import Tag: Manual revert |
CSV import Tags: mobile edit mobile web edit |
||
| (2 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
'''Lamellar ichthyosis''' is a rare | {{SI}} | ||
{{Infobox medical condition | |||
== | | name = Lamellar ichthyosis | ||
The most common | | image = [[File:Riehl_Zumbusch_Tafel_LXV_(3).jpg]] | ||
| caption = Illustration of lamellar ichthyosis | |||
== | | synonyms = [[Nonbullous congenital ichthyosiform erythroderma]] | ||
Lamellar ichthyosis | | pronounce = | ||
| specialty = [[Dermatology]] | |||
== Diagnosis == | | symptoms = [[Dry skin]], [[scaling]], [[erythroderma]] | ||
Diagnosis of lamellar ichthyosis is | | complications = [[Overheating]], [[dehydration]], [[skin infections]] | ||
| onset = [[Birth]] | |||
== | | duration = [[Lifelong]] | ||
| types = | |||
| causes = [[Genetic mutation]] in [[TGM1]], [[ABCA12]], [[ALOX12B]], [[ALOXE3]], [[NIPAL4]] | |||
== See also == | | risks = | ||
| diagnosis = [[Clinical examination]], [[genetic testing]] | |||
| differential = [[Ichthyosis vulgaris]], [[X-linked ichthyosis]], [[Netherton syndrome]] | |||
| prevention = | |||
| treatment = [[Emollients]], [[keratolytics]], [[retinoids]] | |||
| medication = [[Acitretin]], [[isotretinoin]] | |||
| prognosis = [[Variable]], depends on severity | |||
| frequency = 1 in 200,000 to 300,000 | |||
}} | |||
{{Short description|A rare genetic skin disorder}} | |||
'''Lamellar ichthyosis''' is a rare genetic skin disorder characterized by the presence of large, dark, plate-like scales covering the body. It is one of the forms of [[ichthyosis]], a group of disorders that cause dry, scaly skin. Lamellar ichthyosis is present at birth and persists throughout life. | |||
==Pathophysiology== | |||
Lamellar ichthyosis is caused by mutations in genes responsible for skin barrier function. The most common gene associated with this condition is the [[TGM1 gene]], which encodes the enzyme transglutaminase 1. This enzyme is crucial for the formation of the cornified cell envelope, a structure that provides a barrier to water loss and protects against environmental damage. | |||
The defective enzyme leads to impaired skin barrier function, resulting in excessive water loss and the accumulation of scales. The scales are typically large, dark, and plate-like, giving the skin a rough texture. | |||
==Clinical Features== | |||
[[File:Ichthyosis_2.jpg|left|thumb|Lamellar ichthyosis showing large, dark scales on the skin.]] | |||
Individuals with lamellar ichthyosis are often born with a collodion membrane, a shiny, waxy layer of skin that sheds within the first few weeks of life. After the membrane is shed, the characteristic scaling becomes apparent. | |||
The scales are usually most prominent on the trunk, limbs, and scalp, but can affect the entire body. Other features may include: | |||
* Ectropion, or outward turning of the eyelids | |||
* Eclabium, or outward turning of the lips | |||
* Hypohidrosis, or reduced ability to sweat, leading to heat intolerance | |||
* Palmoplantar keratoderma, thickening of the skin on the palms and soles | |||
==Diagnosis== | |||
Diagnosis of lamellar ichthyosis is primarily clinical, based on the characteristic appearance of the skin. Genetic testing can confirm the diagnosis by identifying mutations in the TGM1 gene or other associated genes. | |||
==Management== | |||
Management of lamellar ichthyosis focuses on alleviating symptoms and improving skin barrier function. Treatment options include: | |||
* Regular use of emollients and moisturizers to hydrate the skin | |||
* Keratolytic agents, such as salicylic acid or urea, to help remove scales | |||
* Retinoids, which can reduce scaling and improve skin texture | |||
Patients should also take measures to avoid overheating due to impaired sweating. | |||
==Prognosis== | |||
Lamellar ichthyosis is a lifelong condition, but with appropriate management, individuals can lead normal lives. The severity of symptoms can vary, and some individuals may experience improvement with age. | |||
==See also== | |||
* [[Ichthyosis]] | * [[Ichthyosis]] | ||
* [[ | * [[Genodermatoses]] | ||
* [[TGM1]] | * [[TGM1 gene]] | ||
[[Category:Genetic disorders]] | [[Category:Genetic disorders]] | ||
[[Category: | [[Category:Dermatology]] | ||
Latest revision as of 22:00, 8 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Lamellar ichthyosis | |
|---|---|
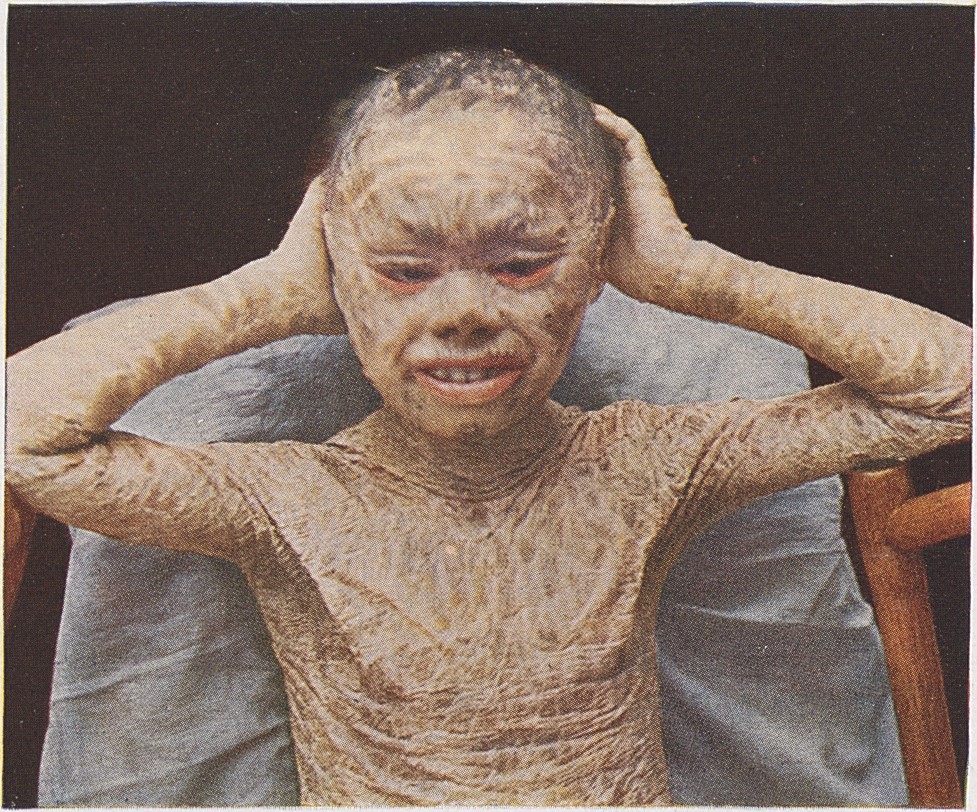
| |
| Synonyms | Nonbullous congenital ichthyosiform erythroderma |
| Pronounce | |
| Specialty | Dermatology |
| Symptoms | Dry skin, scaling, erythroderma |
| Complications | Overheating, dehydration, skin infections |
| Onset | Birth |
| Duration | Lifelong |
| Types | |
| Causes | Genetic mutation in TGM1, ABCA12, ALOX12B, ALOXE3, NIPAL4 |
| Risks | |
| Diagnosis | Clinical examination, genetic testing |
| Differential diagnosis | Ichthyosis vulgaris, X-linked ichthyosis, Netherton syndrome |
| Prevention | |
| Treatment | Emollients, keratolytics, retinoids |
| Medication | Acitretin, isotretinoin |
| Prognosis | Variable, depends on severity |
| Frequency | 1 in 200,000 to 300,000 |
| Deaths | N/A |
A rare genetic skin disorder
Lamellar ichthyosis is a rare genetic skin disorder characterized by the presence of large, dark, plate-like scales covering the body. It is one of the forms of ichthyosis, a group of disorders that cause dry, scaly skin. Lamellar ichthyosis is present at birth and persists throughout life.
Pathophysiology[edit]
Lamellar ichthyosis is caused by mutations in genes responsible for skin barrier function. The most common gene associated with this condition is the TGM1 gene, which encodes the enzyme transglutaminase 1. This enzyme is crucial for the formation of the cornified cell envelope, a structure that provides a barrier to water loss and protects against environmental damage. The defective enzyme leads to impaired skin barrier function, resulting in excessive water loss and the accumulation of scales. The scales are typically large, dark, and plate-like, giving the skin a rough texture.
Clinical Features[edit]

Individuals with lamellar ichthyosis are often born with a collodion membrane, a shiny, waxy layer of skin that sheds within the first few weeks of life. After the membrane is shed, the characteristic scaling becomes apparent. The scales are usually most prominent on the trunk, limbs, and scalp, but can affect the entire body. Other features may include:
- Ectropion, or outward turning of the eyelids
- Eclabium, or outward turning of the lips
- Hypohidrosis, or reduced ability to sweat, leading to heat intolerance
- Palmoplantar keratoderma, thickening of the skin on the palms and soles
Diagnosis[edit]
Diagnosis of lamellar ichthyosis is primarily clinical, based on the characteristic appearance of the skin. Genetic testing can confirm the diagnosis by identifying mutations in the TGM1 gene or other associated genes.
Management[edit]
Management of lamellar ichthyosis focuses on alleviating symptoms and improving skin barrier function. Treatment options include:
- Regular use of emollients and moisturizers to hydrate the skin
- Keratolytic agents, such as salicylic acid or urea, to help remove scales
- Retinoids, which can reduce scaling and improve skin texture
Patients should also take measures to avoid overheating due to impaired sweating.
Prognosis[edit]
Lamellar ichthyosis is a lifelong condition, but with appropriate management, individuals can lead normal lives. The severity of symptoms can vary, and some individuals may experience improvement with age.