Thiamine responsive megaloblastic anemia syndrome

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Thiamine-responsive megaloblastic anemia syndrome | |
|---|---|
| |
| Synonyms | TRMA, Rogers syndrome |
| Pronounce | N/A |
| Specialty | Hematology, Genetics |
| Symptoms | Megaloblastic anemia, diabetes mellitus, sensorineural hearing loss |
| Complications | N/A |
| Onset | Childhood |
| Duration | Lifelong |
| Types | N/A |
| Causes | Mutations in the SLC19A2 gene |
| Risks | Family history of the condition |
| Diagnosis | Genetic testing, blood test |
| Differential diagnosis | Other causes of megaloblastic anemia |
| Prevention | N/A |
| Treatment | Thiamine supplementation |
| Medication | N/A |
| Prognosis | Good with treatment |
| Frequency | Rare |
| Deaths | Rare, if untreated |
Other Names: Thiamine-responsive anemia syndrome; TRMA; Megaloblastic anemia thiamine-responsive with diabetes mellitus and sensorineural deafness; Rogers syndrome; Thiamine-responsive myelodysplasia
Thiamine-responsive megaloblastic anemia syndrome is a very rare condition characterized by hearing loss, diabetes, and a blood disorder called megaloblastic anemia. Affected individuals begin to show symptoms of this condition between infancy and adolescence.
Epidemiology[edit]
Thiamine-responsive megaloblastic anemia syndrome has been reported in approximately 30 families worldwide. Its prevalence is unknown.
Cause[edit]
Mutations in the SLC19A2 gene cause thiamine-responsive megaloblastic anemia syndrome. This gene provides instructions for making a protein called thiamine transporter 1, which transports thiamine into cells. Thiamine is found in many different foods and is important for numerous body functions. Most mutations in the SLC19A2 gene lead to the production of an abnormally short, nonfunctional thiamine transporter 1. Other mutations change single protein building blocks (amino acids) in this protein. All of these mutations prevent thiamine transporter 1 from bringing thiamine into the cell. It remains unclear how the absence of this protein leads to the seemingly unrelated symptoms of megaloblastic anemia, diabetes, and hearing loss. Research suggests that an alternative method for transporting thiamine is present in all the cells of the body, except where blood cells and insulin are formed (in the bone marrow and pancreas, respectively) and cells in the inner ear.
Inheritance[edit]
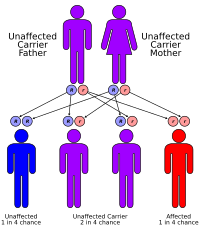
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Signs and symptoms[edit]
Megaloblastic anemia occurs when a person has a low number of red blood cells (anemia), and the remaining red blood cells are larger than normal (megaloblastic). The symptoms of this blood disorder may include decreased appetite, lack of energy, headaches, pale skin, diarrhea, and tingling or numbness in the hands and feet. Individuals with thiamine-responsive megaloblastic anemia syndrome begin to show symptoms of megaloblastic anemia between infancy and adolescence. This syndrome is called "thiamine-responsive" because the anemia can be treated with high doses of vitamin B1 (thiamine). People with thiamine-responsive megaloblastic anemia syndrome develop hearing loss caused by abnormalities of the inner ear (sensorineural hearing loss) during early childhood. It remains unclear whether thiamine treatment can improve hearing or prevent hearing loss. Diabetes becomes apparent in affected individuals sometime between infancy and adolescence. Although these individuals develop diabetes during childhood, they do not have the form of the disease that develops most often in children, called type 1 (autoimmune) diabetes. People with thiamine-responsive megaloblastic anemia syndrome usually require insulin to treat their diabetes. In some cases, treatment with thiamine can reduce the amount of insulin a person needs. Some individuals with thiamine-responsive megaloblastic anemia syndrome develop optic atrophy, which is the degeneration (atrophy) of the nerves that carry information from the eyes to the brain. Heart and blood vessel (cardiovascular) problems such as heart rhythm abnormalities and heart defects have also been reported in some people with this syndrome. For most diseases, symptoms will vary from person to person. People with the same disease may not have all the symptoms listed. 80%-99% of people have these symptoms
- Anorexia
- Diabetes mellitus
- Diarrhea(Watery stool)
- Headache(Headaches)
- Lethargy
- Megaloblastic anemia
- Pallor
- Paresthesia(Pins and needles feeling)
- Sensorineural hearing impairment
30%-79% of people have these symptoms
- Optic atrophy
- Thrombocytopenia(Low platelet count)
5%-29% of people have these symptoms
- Ataxia
- Atrial septal defect(An opening in the wall separating the top two chambers of the heart)
- Cardiac arrest(Heart stops beating)
- Cardiomyopathy(Disease of the heart muscle)
- Congestive heart failure(Cardiac failure)
- CryptorchidismUndescended testes
- Gastroesophageal reflux(Acid reflux)
- Global developmental delay
- Paroxysmal atrial tachycardia
- Retinal dystrophy(Breakdown of light-sensitive cells in back of eye)
- Seizure
- Short stature(Decreased body height)
- Situs inversus totalis(All organs on wrong side of body)
- Stroke
- Ventricular septal defect(Hole in heart wall separating two lower heart chambers)
- Visual loss(Loss of vision)
Diagnosis[edit]
Thiamine-responsive megaloblastic anemia syndrome (TRMA) should be suspected in individuals with the following triad of clinical features: Megaloblastic anemia occurring between infancy and adolescence:
- Examination of the bone marrow reveals megaloblastic changes with erythroblasts often containing iron-filled mitochondria (ringed sideroblasts).
- Vitamin B12/folic acid levels are normal
- The anemia is corrected with pharmacologic doses of thiamine (vitamin B1) (50-100 mg/day). However, the red cells remain macrocytic, suggesting a persistent erythropoietic abnormality ; anemia can recur when thiamine is withdrawn.
- Even without thiamine supplementation, serum thiamine concentrations are normal; there is no evidence of acidosis or aciduria.
- Progressive sensorineural deafness. Hearing loss is generally early and has been detected in toddlers. Whether hearing loss is congenital (prelingual) is unknown. Some affected individuals have signs of megaloblastic anemia and diabetes at an early age, but no hearing loss.
- Diabetes mellitus that is non-type I in nature, with age of onset from infancy to adolescence. Insulin secretion is present but defective.
Treatment[edit]
Lifelong use of pharmacologic doses (50-100 mg/day) of oral thiamine (vitamin B1) in affected individuals regardless of age. Red blood cell transfusion for severe anemia. Red blood cell transfusion for severe anemia is indicated.
NIH genetic and rare disease info[edit]
Thiamine responsive megaloblastic anemia syndrome is a rare disease.
| Rare and genetic diseases | ||||||
|---|---|---|---|---|---|---|
|
Rare diseases - Thiamine responsive megaloblastic anemia syndrome
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian