Pancreatic injury

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Pancreatic injury | |
|---|---|
| |
| Synonyms | Pancreatic trauma |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Abdominal pain, nausea, vomiting, abdominal distension |
| Complications | Pancreatitis, pancreatic fistula, infection, hemorrhage |
| Onset | Sudden, following trauma |
| Duration | Varies, depending on severity and treatment |
| Types | Blunt trauma, penetrating trauma |
| Causes | Blunt abdominal trauma, penetrating abdominal trauma |
| Risks | Motor vehicle collision, falls, sports injuries, assault |
| Diagnosis | CT scan, MRI, ultrasound, ERCP |
| Differential diagnosis | Acute pancreatitis, duodenal injury, liver injury |
| Prevention | Use of seat belts, protective gear in sports |
| Treatment | Surgical intervention, endoscopic procedures, conservative management |
| Medication | Analgesics, antibiotics |
| Prognosis | Depends on severity and promptness of treatment |
| Frequency | Rare |
| Deaths | Varies, depending on severity and complications |
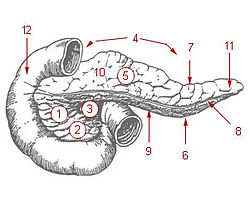
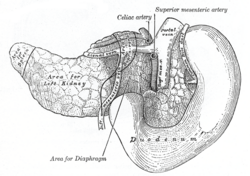
Pancreatic injury refers to any form of trauma sustained by the pancreas, which is a vital organ located in the abdomen. It plays a crucial role in the digestive system by producing enzymes that aid in the digestion of food, as well as hormones such as insulin, which regulates blood sugar levels. Due to its deep location in the abdomen, near the spine and behind the stomach, the pancreas is somewhat protected; however, it can still be damaged by blunt or penetrating trauma. Pancreatic injuries are relatively rare but can be life-threatening if not promptly and properly managed.
Causes[edit]
The most common causes of pancreatic injury include:
- Blunt abdominal trauma, often resulting from motor vehicle accidents, falls, or sports injuries.
- Penetrating trauma, such as stab wounds or gunshot wounds.
- Iatrogenic injury, which occurs as a result of medical or surgical procedures.
Classification[edit]
Pancreatic injuries can be classified based on the extent and type of damage:
- Grade I: Minor contusions or lacerations without duct injury.
- Grade II: Major contusions or lacerations without duct injury.
- Grade III: Distal transection or parenchymal injury with duct injury.
- Grade IV: Proximal transection or parenchymal injury involving the ampulla.
- Grade V: Massive disruption of the pancreatic head.
Symptoms[edit]
Symptoms of pancreatic injury may include:
- Abdominal pain
- Nausea and vomiting
- Tenderness or swelling in the abdominal area
- Signs of internal bleeding, such as dizziness or fainting
Diagnosis[edit]
Diagnosis of pancreatic injury typically involves:
- Medical history and physical examination
- Imaging tests, such as CT scans or MRI
- Laboratory tests, including amylase and lipase levels, which may be elevated in cases of pancreatic injury
Treatment[edit]
Treatment of pancreatic injury depends on the severity of the injury and may include:
- Non-operative management for minor injuries without duct involvement, focusing on rest, pain management, and monitoring.
- Surgical intervention for more severe injuries or those involving the pancreatic duct, which may involve repair of the duct, drainage of any collections, or even partial removal of the pancreas (pancreatectomy).
Complications[edit]
Complications of pancreatic injury can include:
- Pancreatitis, inflammation of the pancreas
- Pseudocyst formation, where fluid accumulates in a cyst-like structure around the pancreas
- Fistula formation, an abnormal connection between the pancreas and other organs
- Infection
- Hemorrhage
Prevention[edit]
Preventing pancreatic injury primarily involves taking general safety measures to avoid trauma, such as wearing seat belts, using protective gear during sports, and avoiding situations that could lead to falls or blows to the abdomen.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian