Pancreatic mucinous cystic neoplasm

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Pancreatic mucinous cystic neoplasm | |
|---|---|
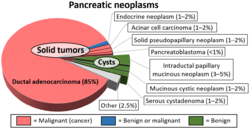
| |
| Synonyms | Mucinous cystic neoplasm of the pancreas |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Abdominal pain, nausea, vomiting, weight loss |
| Complications | Pancreatic cancer |
| Onset | Typically in middle-aged women |
| Duration | Variable |
| Types | Mucinous cystadenoma, Mucinous cystadenocarcinoma |
| Causes | Unknown |
| Risks | Smoking, obesity, family history of pancreatic conditions |
| Diagnosis | CT scan, MRI, Endoscopic ultrasound, Biopsy |
| Differential diagnosis | Serous cystadenoma, Intraductal papillary mucinous neoplasm, Pseudocyst |
| Prevention | Regular monitoring for those at risk |
| Treatment | Surgical resection |
| Medication | None specific |
| Prognosis | Generally good if benign; variable if malignant |
| Frequency | Rare |
| Deaths | N/A |
Pancreatic mucinous cystic neoplasm (PMCN) is a type of cyst that develops in the pancreas. These cysts are filled with a thick, sticky fluid known as mucin. PMCNs are considered premalignant lesions, which means they have the potential to develop into cancer if left untreated.
Overview[edit]
PMCNs are rare, accounting for only 1% to 2% of all pancreatic neoplasms. They are most commonly found in middle-aged women and are typically located in the body or tail of the pancreas. The size of PMCNs can vary greatly, ranging from a few millimeters to several centimeters in diameter.
Symptoms[edit]
Most PMCNs are asymptomatic, meaning they do not cause any symptoms. However, if the cyst grows large enough, it can cause abdominal pain, nausea, vomiting, and weight loss. In rare cases, a PMCN can lead to pancreatitis, a serious condition that causes inflammation of the pancreas.
Diagnosis[edit]
PMCNs are typically discovered during imaging tests, such as computed tomography (CT) scans or magnetic resonance imaging (MRI), that are performed for other reasons. Once a cyst is found, a biopsy may be performed to determine whether it is a PMCN. This involves removing a small sample of tissue from the cyst and examining it under a microscope.
Treatment[edit]
The treatment for PMCNs depends on the size and location of the cyst, as well as the patient's overall health. Small cysts that are not causing symptoms may be monitored with regular imaging tests. Larger cysts, or those that are causing symptoms, may need to be removed surgically. In some cases, the entire pancreas may need to be removed.
Prognosis[edit]
The prognosis for PMCNs is generally good, especially if the cyst is discovered and treated early. However, if a PMCN develops into cancer, the prognosis can be poor. Regular monitoring and early treatment are key to preventing this from happening.