Muir–Torre syndrome
| Muir–Torre syndrome | |
|---|---|
| |
| Synonyms | MTS |
| Pronounce | |
| Field | Oncology, Dermatology, Genetics |
| Symptoms | Sebaceous tumors, internal malignancies |
| Complications | Colorectal cancer, genitourinary cancers |
| Onset | Usually adulthood |
| Duration | Lifelong |
| Types | |
| Causes | Genetic mutations in MLH1, MSH2, MSH6 genes |
| Risks | Family history of Lynch syndrome |
| Diagnosis | Clinical presentation, genetic testing, immunohistochemistry |
| Differential diagnosis | Sporadic sebaceous tumors, other hereditary cancer syndromes |
| Prevention | Regular screening, genetic counseling |
| Treatment | Surgical excision, regular cancer surveillance |
| Medication | |
| Prognosis | Good with early detection and management |
| Frequency | Rare |
| Deaths | Usually related to complications from malignancies |
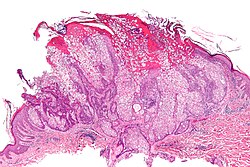
Muir–Torre syndrome (MTS) is a rare, hereditary autosomal dominant cancer syndrome, considered a subtype of Lynch syndrome (Hereditary Non-Polyposis Colorectal Cancer, HNPCC). Individuals with this syndrome have an increased susceptibility to cancers of the colon, genitourinary tract, and distinct skin lesions, including keratoacanthomas and sebaceous tumors such as sebaceous adenoma, sebaceous epithelioma, and sebaceous carcinoma.
Signs and Symptoms[edit]
Characteristic features include:
- Presence of at least one sebaceous gland tumor (adenoma, epithelioma, or carcinoma)
- Occurrence of at least one internal malignancy, commonly colorectal or genitourinary cancers
Genetics[edit]
Muir–Torre syndrome is caused primarily by mutations in the MLH1, MSH2, and more recently identified MSH6 genes. These genes are critical for the DNA mismatch repair pathway. Mutations result in defective DNA repair mechanisms, increasing the risk of developing cancers.
Diagnosis[edit]
Diagnosis typically involves:
- Clinical evaluation of sebaceous skin tumors and internal malignancies
- Genetic testing for mutations in DNA mismatch repair genes
- Immunohistochemical analysis for mismatch repair proteins
- Application of the Amsterdam criteria, widely used to diagnose Lynch syndrome and Muir–Torre syndrome, which include:
- At least three relatives affected by Lynch-associated cancers (colorectal, endometrial, small bowel, ureter, renal pelvis)
- Cancer affecting at least two successive generations
- At least one individual diagnosed before age 50
- Exclusion of familial adenomatous polyposis
The Mayo Muir–Torre risk score was developed to enhance diagnostic accuracy, distinguishing true cases from sporadic sebaceous tumors.
Management[edit]
Treatment strategies involve:
- Surgical removal of skin lesions
- Regular screening and surveillance for internal malignancies (colonoscopies, genitourinary screenings)
- Genetic counseling for patients and their families
Prognosis[edit]
With appropriate management and regular surveillance, the prognosis for individuals with Muir–Torre syndrome can be favorable. Early detection and treatment of malignancies significantly improve outcomes.
Prevention[edit]
Preventive measures focus on:
- Early genetic screening and counseling for at-risk families
- Frequent surveillance for early detection of malignancies
Muir–Torre syndrome remains a rare condition, requiring multidisciplinary care involving dermatologists, geneticists, oncologists, and surgeons.
Eponym[edit]
It is named for EG Muir and D Torre. A British physician, Muir noted a patient with many keratoacanthomas who went on to develop several internal malignancies at a young age. Torre presented his findings at a meeting of the New York Dermatologic Society.
See also[edit]
- List of cutaneous conditions
- List of cutaneous conditions associated with increased risk of nonmelanoma skin cancer
External links[edit]
| Tumors and associated structures | ||||||
|---|---|---|---|---|---|---|
|
| Metabolic disease: DNA replication and DNA repair-deficiency disorder | ||||
|---|---|---|---|---|
|
Ad. Transform your life with W8MD's
GLP-1 weight loss injections special from $29.99 with insurance
|
WikiMD Medical Encyclopedia |
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian


