Hyper-IgM syndrome type 2

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Hyper-IgM syndrome type 2 | |
|---|---|
 | |
| Synonyms | HIGM2 |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Recurrent infections, low levels of IgG, IgA, and IgE |
| Complications | Increased risk of autoimmune diseases, liver disease |
| Onset | Childhood |
| Duration | Lifelong |
| Types | N/A |
| Causes | Genetic mutation in AICDA gene |
| Risks | Family history of the condition |
| Diagnosis | Genetic testing, measurement of immunoglobulin levels |
| Differential diagnosis | Other types of Hyper-IgM syndrome, Common variable immunodeficiency |
| Prevention | N/A |
| Treatment | Immunoglobulin replacement therapy, antibiotics for infections |
| Medication | N/A |
| Prognosis | Variable, depending on severity and treatment |
| Frequency | Rare |
| Deaths | N/A |
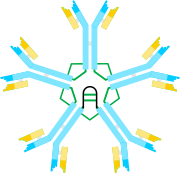
Hyper-IgM syndrome type 2 is a rare genetic disorder characterized by an immune system that is unable to respond effectively to certain infections. This condition primarily affects males.
Symptoms[edit]
The symptoms of Hyper-IgM syndrome type 2 typically become apparent in infancy or early childhood. These symptoms can include recurrent infections, particularly in the lungs, sinuses, and ears. Other symptoms can include diarrhea, pneumonia, and a failure to thrive.
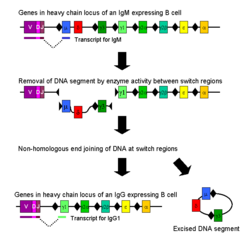
Causes[edit]
Hyper-IgM syndrome type 2 is caused by mutations in the AICDA gene. This gene provides instructions for making an enzyme that is essential for the immune system to function properly. Mutations in the AICDA gene disrupt the normal function of this enzyme, leading to the symptoms of Hyper-IgM syndrome type 2.
Diagnosis[edit]
The diagnosis of Hyper-IgM syndrome type 2 is typically made based on the presence of characteristic symptoms, a detailed patient history, a thorough clinical evaluation, and a variety of specialized tests.
Treatment[edit]
The treatment of Hyper-IgM syndrome type 2 is directed toward the specific symptoms that are apparent in each individual. Treatment may include the administration of antibiotics to treat infections, immunoglobulin therapy to boost the immune system, and in some cases, a bone marrow transplant.
Prognosis[edit]
The prognosis of Hyper-IgM syndrome type 2 varies among affected individuals. The disorder is typically chronic and can be life-threatening in severe cases. However, with appropriate treatment and management, individuals with Hyper-IgM syndrome type 2 can lead a normal life.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian