Familial dysautonomia

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Familial dysautonomia | |
|---|---|

| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Hypotonia, feeding difficulties, autonomic crises, insensitivity to pain, dysautonomia |
| Complications | N/A |
| Onset | Infancy |
| Duration | Lifelong |
| Types | N/A |
| Causes | Genetic mutation in the IKBKAP gene |
| Risks | Ashkenazi Jewish descent |
| Diagnosis | Genetic testing, clinical evaluation |
| Differential diagnosis | Riley-Day syndrome, other hereditary sensory and autonomic neuropathies |
| Prevention | N/A |
| Treatment | Supportive care, symptomatic treatment |
| Medication | N/A |
| Prognosis | Variable, with improved outcomes due to early diagnosis and management |
| Frequency | Rare, primarily in individuals of Ashkenazi Jewish descent |
| Deaths | Historically high, but improving with advances in care |
A genetic disorder affecting the autonomic nervous system
Familial dysautonomia (FD), also known as Riley-Day syndrome, is a rare genetic disorder that affects the development and function of the autonomic nervous system and sensory nervous system. It is classified as a type of hereditary sensory and autonomic neuropathy (HSAN).
Genetics[edit]
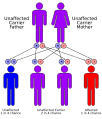
Familial dysautonomia is an autosomal recessive disorder, meaning that an individual must inherit two copies of the defective gene, one from each parent, to be affected. The disorder is caused by mutations in the IKBKAP gene, which is located on chromosome 9. This gene is responsible for producing a protein called IKAP, which is involved in the development and maintenance of nerve cells.
Symptoms[edit]
The symptoms of familial dysautonomia are varied and can affect multiple systems of the body. Common symptoms include:
- Poor muscle tone (hypotonia)
- Feeding difficulties
- Lack of tears (alacrima)
- Frequent lung infections
- Difficulty regulating body temperature
- Episodes of dysautonomic crisis, characterized by vomiting, sweating, and changes in blood pressure and heart rate
- Scoliosis
- Poor growth and delayed development
Diagnosis[edit]
Diagnosis of familial dysautonomia is typically based on clinical evaluation and genetic testing. A blood test can identify mutations in the IKBKAP gene, confirming the diagnosis. Prenatal testing is also available for families with a known history of the disorder.
Management[edit]
There is no cure for familial dysautonomia, but treatment focuses on managing symptoms and improving quality of life. Management strategies may include:
- Nutritional support, such as feeding tubes
- Medications to control blood pressure and heart rate
- Physical therapy to improve muscle tone and coordination
- Regular monitoring and treatment of lung infections
- Surgery to correct scoliosis or other skeletal abnormalities
Prognosis[edit]
The prognosis for individuals with familial dysautonomia varies. Advances in medical care have improved life expectancy and quality of life for many patients. However, the disorder remains serious and can lead to complications that affect daily living.
Epidemiology[edit]
Familial dysautonomia is most commonly found in individuals of Ashkenazi Jewish descent, with a carrier frequency of approximately 1 in 30 in this population. It is much rarer in other ethnic groups.
Familial dysautonomia images[edit]
-
No Tears Life With FD
-
Autorecessive
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian