Pelvic organ prolapse

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Pelvic organ prolapse | |
|---|---|

| |
| Synonyms | Pelvic floor dysfunction |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Urinary incontinence, fecal incontinence, pelvic pressure, vaginal bulge |
| Complications | Urinary tract infections, sexual dysfunction |
| Onset | More common after childbirth and menopause |
| Duration | Long-term |
| Types | N/A |
| Causes | Weakening of the pelvic floor muscles |
| Risks | Childbirth, obesity, hysterectomy, aging |
| Diagnosis | Pelvic examination, ultrasound, MRI |
| Differential diagnosis | Urinary tract infection, vaginal cyst |
| Prevention | Pelvic floor exercises, maintaining a healthy weight |
| Treatment | Pessary, pelvic floor physical therapy, surgery |
| Medication | Estrogen therapy |
| Prognosis | Varies; often manageable with treatment |
| Frequency | Common, especially in older women |
| Deaths | N/A |


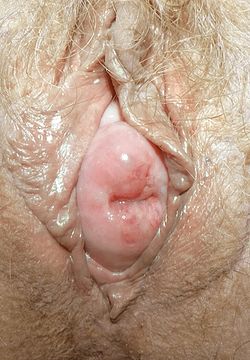
Pelvic Organ Prolapse (POP) is a medical condition characterized by the descent of pelvic organs from their normal anatomical positions. This condition can affect both men and women, although it is more commonly seen in women. Pelvic organ prolapse occurs when the pelvic floor, a complex structure of muscles, ligaments, and connective tissues that supports the pelvic organs, weakens or becomes damaged, leading to the displacement of one or more pelvic organs.
Causes and Risk Factors[edit]
The development of pelvic organ prolapse can be attributed to various factors:
- 1. Childbirth: In women, the strain and trauma experienced during vaginal childbirth can lead to damage to the pelvic floor muscles and connective tissues. This is one of the most common causes of POP.
- 2. Gynecological Surgery: Surgeries such as hysterectomy (removal of the uterus) or other gynecological procedures can weaken the pelvic support structures.
- 3. Heavy Lifting: Engaging in activities that involve heavy lifting or straining can contribute to the development of POP, particularly in men.
- 4. Chronic Constipation: Repeated straining during bowel movements can stress the pelvic floor.
- 5. Aging: The natural aging process can weaken the pelvic tissues, making them more susceptible to prolapse.
- 6. Genetic Predisposition: Some individuals may have a genetic predisposition to developing pelvic organ prolapse.
Types of Pelvic Organ Prolapse[edit]
Pelvic organ prolapse can involve different pelvic organs, resulting in distinct types:
- 1. Cystocele: Occurs when the bladder descends into the anterior vaginal wall, leading to urinary symptoms such as frequent urination or urinary incontinence.
- 2. Rectocele: Involves the bulging of the rectum into the posterior vaginal wall, often causing difficulty with bowel movements and discomfort.
- 3. Uterine prolapse: This occurs when the uterus drops into the vaginal canal, often seen in women who have given birth.
- 4. Vaginal vault prolapse: After a hysterectomy (removal of the uterus), the top of the vagina may prolapse.
Symptoms[edit]
The symptoms of pelvic organ prolapse can vary depending on the type and severity of the condition. Common symptoms include:
- 1. Pelvic Pressure: A sensation of fullness or pressure in the pelvis.
- 2. Vaginal Bulge: A noticeable protrusion from the vaginal opening.
- 3. Discomfort or Pain: Pelvic or vaginal discomfort, especially during activities like standing or walking.
- 4. Urinary and Bowel Issues: Frequent urination, urgency, stress urinary incontinence, constipation, or difficulty with bowel movements.
Diagnosis and Treatment[edit]
The diagnosis of pelvic organ prolapse involves a medical history review, pelvic examination, and, in some cases, additional tests like pelvic ultrasound or urodynamic studies. Treatment options for pelvic organ prolapse include:
- 1. Conservative Measures: Lifestyle modifications, including dietary and weight management, as well as pelvic floor exercises (Kegels), can help manage milder cases.
- 2. Physical Therapy: Pelvic floor physical therapy aims to strengthen and support the pelvic muscles.
- 3. Pessaries: These are vaginal support devices that can be fitted by a healthcare provider to help support the pelvic organs.
- 4. Medications: Medications may be prescribed to manage associated symptoms like urinary incontinence.
- 5. Surgery: Surgical procedures, such as vaginal or abdominal repair, may be necessary for severe cases.
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian