Adenoid cystic carcinoma
| Adenoid cystic carcinoma | |
|---|---|
| Micrograph of adenoid cystic carcinoma | |
| Synonyms | ACC |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Pain, swelling, numbness, facial nerve paralysis |
| Complications | Metastasis, recurrence |
| Onset | Middle age |
| Duration | Long-term |
| Types | Cribriform, tubular, solid |
| Causes | Unknown |
| Risks | Radiation exposure, genetic predisposition |
| Diagnosis | Biopsy, imaging studies |
| Differential diagnosis | Pleomorphic adenoma, mucoepidermoid carcinoma |
| Prevention | None |
| Treatment | Surgery, radiation therapy, chemotherapy |
| Medication | Cisplatin, doxorubicin |
| Prognosis | Variable, often poor in advanced stages |
| Frequency | Rare |
| Deaths | Varies |
== Adenoid Cystic Carcinoma ==
Adenoid cystic carcinoma (ACC) is a rare type of cancer that most commonly arises in the salivary glands. It is known for its slow growth, tendency to invade surrounding nerves, and potential for distant metastasis.
Pathophysiology[edit]
Adenoid cystic carcinoma is characterized by its unique histological appearance, which includes cribriform, tubular, and solid patterns. The tumor is composed of small, basaloid cells that form pseudocystic spaces filled with hyaline material. ACC is notorious for its perineural invasion, which can lead to significant neurological symptoms.
Clinical Presentation[edit]
Patients with adenoid cystic carcinoma often present with a painless mass in the affected gland, most commonly the parotid gland or submandibular gland. Due to its propensity for perineural invasion, patients may also experience facial nerve paralysis or other cranial nerve deficits.
Diagnosis[edit]
Diagnosis of ACC is typically made through a combination of imaging studies and biopsy. MRI is particularly useful for assessing perineural spread, as seen in the images below:
-
Coronal MRI showing right parotid adenoid cystic carcinoma with perineural spread.
-
MRI showing perineural spread of adenoid cystic carcinoma along the facial nerve.
Histopathology[edit]
Histological examination reveals the characteristic cribriform pattern of ACC. Immunohistochemical staining, such as S-100, can aid in diagnosis:
-
Histological section of adenoid cystic carcinoma.
-
S-100 staining of adenoid cystic carcinoma.
-
Cytological image of adenoid cystic carcinoma.
-
Adenoid cystic carcinoma with comedonecrosis.
Treatment[edit]
The primary treatment for adenoid cystic carcinoma is surgical resection with clear margins. Due to the high risk of perineural invasion, adjuvant radiation therapy is often recommended. Chemotherapy is generally reserved for metastatic disease.
Prognosis[edit]
The prognosis for patients with adenoid cystic carcinoma varies depending on the stage and location of the tumor. While the tumor is slow-growing, it has a high rate of local recurrence and distant metastasis, particularly to the lungs.
Epidemiology[edit]
Adenoid cystic carcinoma accounts for approximately 1% of all head and neck malignancies. It is more common in women and typically presents in middle-aged adults.
-
Relative incidence of submandibular tumors.
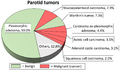
-
Relative incidence of parotid tumors.
Related Pages[edit]
-
Adenoid cystic carcinoma - intermediate magnification
-
Coronal MRI showing right parotid adenoid cystic carcinoma with perineural spread of tumor
-
MRI showing perineural spread of adenoid cystic carcinoma along the facial nerve
-
Adenoid cystic carcinoma
-
Adenoid cystic carcinoma (S-100)
-
Adenoid cystic carcinoma cytology
-
Adenoid cystic carcinoma with comedonecrosis
-
Relative incidence of submandibular tumors
-
Relative incidence of parotid tumors
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian