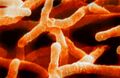
Actinomyces israelii
Actinomyces israelii[edit]
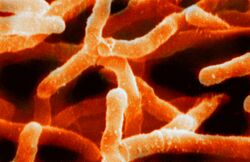
Actinomyces israelii is a species of bacteria in the genus Actinomyces. It is a gram-positive, non-acid-fast, anaerobic to microaerophilic organism. Actinomyces israelii is known for causing the disease actinomycosis, which is characterized by the formation of abscesses in the mouth, lungs, or gastrointestinal tract.
Characteristics[edit]
Actinomyces israelii is a filamentous bacterium that is part of the normal flora of the human oral cavity, gastrointestinal tract, and female genital tract. It is an obligate anaerobe, meaning it thrives in environments devoid of oxygen, although it can tolerate low levels of oxygen (microaerophilic conditions).
The bacterium is known for its ability to form sulfur granules, which are colonies of bacteria surrounded by a proteinaceous matrix. These granules are often found in the pus of actinomycosis lesions and are a key diagnostic feature.
Pathogenesis[edit]
Actinomyces israelii is an opportunistic pathogen. It typically causes infection when the mucosal barrier is disrupted, allowing the bacteria to invade deeper tissues. This can occur due to dental procedures, trauma, or surgery.
The infection progresses slowly and can lead to chronic granulomatous inflammation. The most common form of actinomycosis is cervicofacial actinomycosis, often referred to as "lumpy jaw," which affects the jaw and neck region.
Clinical Manifestations[edit]
The clinical manifestations of actinomycosis depend on the site of infection. Common forms include:
- Cervicofacial actinomycosis: Characterized by swelling, abscess formation, and draining sinuses in the jaw and neck area.
- Thoracic actinomycosis: Involves the lungs and can mimic tuberculosis or lung cancer.
- Abdominal actinomycosis: Affects the gastrointestinal tract and can present as a mass or abscess in the abdomen.
- Pelvic actinomycosis: Often associated with the use of intrauterine devices (IUDs) and can cause pelvic inflammatory disease.
Diagnosis[edit]
Diagnosis of actinomycosis is challenging due to its nonspecific symptoms and slow progression. It is often confirmed by:
- Microscopic examination of pus or tissue samples, revealing sulfur granules.
- Culture of the organism, although this can be difficult due to its slow growth and anaerobic nature.
- Imaging studies, such as CT scans or MRI, to assess the extent of the infection.
Treatment[edit]
The treatment of actinomycosis involves prolonged antibiotic therapy, typically with penicillin. In cases of penicillin allergy, doxycycline or clindamycin may be used. Surgical intervention may be necessary to drain abscesses or remove infected tissue.
Prevention[edit]
Preventive measures include maintaining good oral hygiene and seeking prompt treatment for dental infections. Avoiding unnecessary trauma to the mucosal surfaces can also reduce the risk of infection.
Related pages[edit]
Gallery[edit]
-
Actinomyces israelii under a microscope
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian