Adrenoleukodystrophy
| Adrenoleukodystrophy | |
|---|---|
| |
| Synonyms | ALD, X-linked adrenoleukodystrophy |
| Pronounce | |
| Specialty | Neurology, Endocrinology |
| Symptoms | Seizures, hyperactivity, vision problems, hearing loss, adrenal insufficiency |
| Complications | N/A |
| Onset | Childhood, adulthood |
| Duration | Progressive |
| Types | Childhood cerebral, adrenomyeloneuropathy, Addison-only |
| Causes | Mutations in the ABCD1 gene |
| Risks | Family history |
| Diagnosis | Genetic testing, MRI, blood test for very long chain fatty acids |
| Differential diagnosis | Multiple sclerosis, metachromatic leukodystrophy, Zellweger syndrome |
| Prevention | N/A |
| Treatment | Lorenzo's oil, hematopoietic stem cell transplantation, adrenal hormone replacement |
| Medication | |
| Prognosis | Variable, depends on type and age of onset |
| Frequency | 1 in 20,000 to 50,000 people |
| Deaths | |
Genetic disorder affecting the nervous system and adrenal glands
Adrenoleukodystrophy (ALD) is a rare, genetic disorder characterized by the breakdown or loss of myelin, the fatty covering surrounding nerve cells in the brain, and progressive dysfunction of the adrenal glands. It is an X-linked disorder, meaning it predominantly affects males, although female carriers can also exhibit symptoms.
Genetics

ALD is caused by mutations in the ABCD1 gene located on the X chromosome. This gene encodes a protein that is part of the ATP-binding cassette (ABC) transporter family, which is involved in the transport of very long-chain fatty acids (VLCFAs) into peroxisomes for degradation. Mutations in the ABCD1 gene lead to the accumulation of VLCFAs in tissues, particularly affecting the nervous system and adrenal cortex.
Pathophysiology
The accumulation of VLCFAs in the central nervous system leads to the destruction of myelin, the protective sheath surrounding nerve fibers. This demyelination process disrupts the normal transmission of nerve impulses, resulting in neurological symptoms. In the adrenal glands, VLCFA accumulation impairs the production of adrenal hormones, leading to adrenal insufficiency.
Clinical Presentation

The clinical presentation of ALD can vary widely, but it is generally categorized into several phenotypes:
- Childhood cerebral ALD: This is the most severe form, typically presenting between ages 4 and 10. It is characterized by rapid neurological decline, including behavioral changes, vision and hearing loss, motor dysfunction, and eventually, severe disability or death.
- Adrenomyeloneuropathy (AMN): This adult-onset form presents with progressive stiffness and weakness in the legs, bladder dysfunction, and sexual dysfunction. It is less severe than the childhood form but can lead to significant disability.
- Addison-only phenotype: Some individuals present primarily with adrenal insufficiency without significant neurological symptoms.
Diagnosis
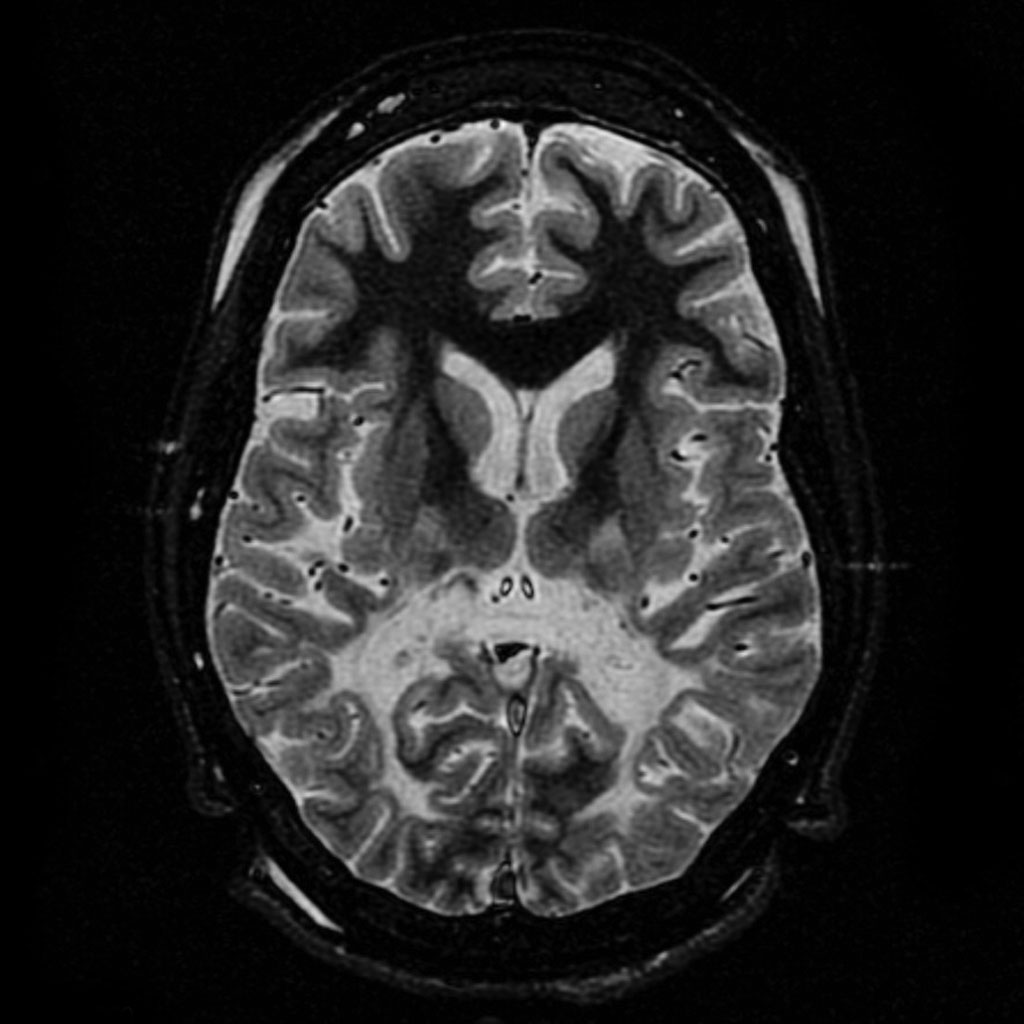
Diagnosis of ALD is based on clinical presentation, family history, and biochemical testing for elevated VLCFA levels in the blood. Genetic testing can confirm mutations in the ABCD1 gene. MRI imaging is used to assess the extent of demyelination in the brain.
Treatment
There is no cure for ALD, but treatment focuses on managing symptoms and slowing disease progression. Options include:
- Lorenzo's oil: A mixture of oleic and erucic acids that can reduce VLCFA levels in the blood.
- Hematopoietic stem cell transplantation (HSCT): This can be effective in early stages of cerebral ALD.
- Adrenal hormone replacement therapy: For those with adrenal insufficiency.
Prognosis
The prognosis of ALD varies depending on the phenotype and age of onset. Childhood cerebral ALD has a poor prognosis without treatment, while AMN progresses more slowly. Early diagnosis and intervention can improve outcomes.
Related pages
Ad. Transform your life with W8MD's
GLP-1 weight loss injections special from $29.99 with insurance
|
WikiMD Medical Encyclopedia |
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian