High-grade serous carcinoma: Difference between revisions
CSV import Tags: mobile edit mobile web edit |
CSV import Tags: mobile edit mobile web edit |
||
| Line 1: | Line 1: | ||
[[ | {{SI}} | ||
{{Infobox medical condition | |||
| name = High-grade serous carcinoma | |||
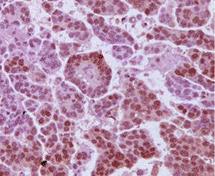
| image = [[File:Androgen_receptors_on_a_HGSC_tumour.jpg|250px]] | |||
| caption = Androgen receptors on a high-grade serous carcinoma tumor | |||
| field = [[Oncology]] | |||
| synonyms = HGSC | |||
| symptoms = [[Abdominal pain]], [[bloating]], [[urinary symptoms]], [[pelvic pain]] | |||
| complications = [[Metastasis]], [[ascites]], [[pleural effusion]] | |||
| onset = Typically in [[postmenopausal]] women | |||
| duration = Chronic | |||
| types = [[Ovarian cancer]], [[fallopian tube cancer]], [[primary peritoneal cancer]] | |||
| causes = [[Genetic mutations]] (e.g., [[BRCA1]], [[BRCA2]]) | |||
| risks = [[Family history]], [[genetic predisposition]], [[age]] | |||
| diagnosis = [[Pelvic examination]], [[transvaginal ultrasound]], [[CA-125 blood test]], [[biopsy]] | |||
| differential = [[Endometrioid carcinoma]], [[clear cell carcinoma]], [[mucinous carcinoma]] | |||
| prevention = [[Genetic counseling]], [[prophylactic oophorectomy]] | |||
| treatment = [[Surgery]], [[chemotherapy]], [[targeted therapy]] | |||
| medication = [[Carboplatin]], [[paclitaxel]], [[PARP inhibitors]] | |||
| prognosis = Variable, often poor | |||
| frequency = Most common type of [[ovarian cancer]] | |||
}} | |||
[[file:High_grade_serous_carcinoma_theories_of_origin_diagram.png|left|thumb]] '''High-grade serous carcinoma''' ('''HGSC''') is a type of [[epithelial ovarian cancer]] that is characterized by its aggressive nature and poor prognosis. It is the most common and lethal form of ovarian cancer, accounting for approximately 70% of all ovarian cancer cases. HGSC primarily affects the [[ovaries]], but it can also originate in the [[fallopian tubes]] and the [[peritoneum]]. | |||
== Pathophysiology == | == Pathophysiology == | ||
HGSC is believed to originate from the epithelial cells lining the fallopian tubes, specifically from the [[fimbriae]] at the distal end of the tubes. These cells undergo genetic mutations, most notably in the [[TP53]] gene, which is mutated in nearly all cases of HGSC. Other common genetic alterations include mutations in the [[BRCA1]] and [[BRCA2]] genes, which are also associated with an increased risk of [[breast cancer]]. | HGSC is believed to originate from the epithelial cells lining the fallopian tubes, specifically from the [[fimbriae]] at the distal end of the tubes. These cells undergo genetic mutations, most notably in the [[TP53]] gene, which is mutated in nearly all cases of HGSC. Other common genetic alterations include mutations in the [[BRCA1]] and [[BRCA2]] genes, which are also associated with an increased risk of [[breast cancer]]. | ||
== Clinical Presentation == | == Clinical Presentation == | ||
Patients with HGSC often present with non-specific symptoms, which can include [[abdominal pain]], [[bloating]], and changes in [[bowel habits]]. Due to the vague nature of these symptoms, HGSC is frequently diagnosed at an advanced stage, when the cancer has already spread to other parts of the abdomen and pelvis. | Patients with HGSC often present with non-specific symptoms, which can include [[abdominal pain]], [[bloating]], and changes in [[bowel habits]]. Due to the vague nature of these symptoms, HGSC is frequently diagnosed at an advanced stage, when the cancer has already spread to other parts of the abdomen and pelvis. | ||
== Diagnosis == | == Diagnosis == | ||
The diagnosis of HGSC typically involves a combination of [[pelvic examination]], [[imaging studies]] such as [[ultrasound]], [[CT scan]], or [[MRI]], and [[blood tests]] including the measurement of [[CA-125]] levels. Definitive diagnosis is made through [[histopathological examination]] of tissue obtained via [[biopsy]] or during [[surgery]]. | The diagnosis of HGSC typically involves a combination of [[pelvic examination]], [[imaging studies]] such as [[ultrasound]], [[CT scan]], or [[MRI]], and [[blood tests]] including the measurement of [[CA-125]] levels. Definitive diagnosis is made through [[histopathological examination]] of tissue obtained via [[biopsy]] or during [[surgery]]. | ||
== Treatment == | == Treatment == | ||
The primary treatment for HGSC involves a combination of [[surgery]] and [[chemotherapy]]. Surgical intervention aims to remove as much of the tumor as possible, a procedure known as [[cytoreductive surgery]] or [[debulking]]. This is usually followed by chemotherapy with [[platinum-based drugs]] such as [[cisplatin]] or [[carboplatin]], often in combination with [[paclitaxel]]. | The primary treatment for HGSC involves a combination of [[surgery]] and [[chemotherapy]]. Surgical intervention aims to remove as much of the tumor as possible, a procedure known as [[cytoreductive surgery]] or [[debulking]]. This is usually followed by chemotherapy with [[platinum-based drugs]] such as [[cisplatin]] or [[carboplatin]], often in combination with [[paclitaxel]]. | ||
== Prognosis == | == Prognosis == | ||
The prognosis for patients with HGSC is generally poor, with a five-year survival rate of less than 50%. The high recurrence rate and the development of [[chemoresistance]] contribute to the challenging nature of treating this disease. Ongoing research is focused on identifying new therapeutic targets and improving early detection methods. | The prognosis for patients with HGSC is generally poor, with a five-year survival rate of less than 50%. The high recurrence rate and the development of [[chemoresistance]] contribute to the challenging nature of treating this disease. Ongoing research is focused on identifying new therapeutic targets and improving early detection methods. | ||
== Research and Future Directions == | == Research and Future Directions == | ||
Current research in HGSC is exploring the role of [[PARP inhibitors]] in patients with [[BRCA mutations]], as well as the potential of [[immunotherapy]] and [[targeted therapy]] to improve outcomes. Efforts are also being made to develop better screening tools to detect HGSC at an earlier, more treatable stage. | Current research in HGSC is exploring the role of [[PARP inhibitors]] in patients with [[BRCA mutations]], as well as the potential of [[immunotherapy]] and [[targeted therapy]] to improve outcomes. Efforts are also being made to develop better screening tools to detect HGSC at an earlier, more treatable stage. | ||
== See Also == | == See Also == | ||
* [[Ovarian cancer]] | * [[Ovarian cancer]] | ||
| Line 26: | Line 41: | ||
* [[Chemotherapy]] | * [[Chemotherapy]] | ||
* [[Surgery]] | * [[Surgery]] | ||
== References == | == References == | ||
{{Reflist}} | {{Reflist}} | ||
== External Links == | == External Links == | ||
{{Commons category|High-grade serous carcinoma}} | {{Commons category|High-grade serous carcinoma}} | ||
[[Category:Ovarian cancer]] | [[Category:Ovarian cancer]] | ||
[[Category:Gynecologic oncology]] | [[Category:Gynecologic oncology]] | ||
[[Category:Carcinoma]] | [[Category:Carcinoma]] | ||
{{medicine-stub}} | {{medicine-stub}} | ||
Latest revision as of 04:00, 7 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD medical weight loss NYC and sleep center NYC
| High-grade serous carcinoma | |
|---|---|
| |
| Synonyms | HGSC |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Abdominal pain, bloating, urinary symptoms, pelvic pain |
| Complications | Metastasis, ascites, pleural effusion |
| Onset | Typically in postmenopausal women |
| Duration | Chronic |
| Types | Ovarian cancer, fallopian tube cancer, primary peritoneal cancer |
| Causes | Genetic mutations (e.g., BRCA1, BRCA2) |
| Risks | Family history, genetic predisposition, age |
| Diagnosis | Pelvic examination, transvaginal ultrasound, CA-125 blood test, biopsy |
| Differential diagnosis | Endometrioid carcinoma, clear cell carcinoma, mucinous carcinoma |
| Prevention | Genetic counseling, prophylactic oophorectomy |
| Treatment | Surgery, chemotherapy, targeted therapy |
| Medication | Carboplatin, paclitaxel, PARP inhibitors |
| Prognosis | Variable, often poor |
| Frequency | Most common type of ovarian cancer |
| Deaths | N/A |

High-grade serous carcinoma (HGSC) is a type of epithelial ovarian cancer that is characterized by its aggressive nature and poor prognosis. It is the most common and lethal form of ovarian cancer, accounting for approximately 70% of all ovarian cancer cases. HGSC primarily affects the ovaries, but it can also originate in the fallopian tubes and the peritoneum.
Pathophysiology[edit]
HGSC is believed to originate from the epithelial cells lining the fallopian tubes, specifically from the fimbriae at the distal end of the tubes. These cells undergo genetic mutations, most notably in the TP53 gene, which is mutated in nearly all cases of HGSC. Other common genetic alterations include mutations in the BRCA1 and BRCA2 genes, which are also associated with an increased risk of breast cancer.
Clinical Presentation[edit]
Patients with HGSC often present with non-specific symptoms, which can include abdominal pain, bloating, and changes in bowel habits. Due to the vague nature of these symptoms, HGSC is frequently diagnosed at an advanced stage, when the cancer has already spread to other parts of the abdomen and pelvis.
Diagnosis[edit]
The diagnosis of HGSC typically involves a combination of pelvic examination, imaging studies such as ultrasound, CT scan, or MRI, and blood tests including the measurement of CA-125 levels. Definitive diagnosis is made through histopathological examination of tissue obtained via biopsy or during surgery.
Treatment[edit]
The primary treatment for HGSC involves a combination of surgery and chemotherapy. Surgical intervention aims to remove as much of the tumor as possible, a procedure known as cytoreductive surgery or debulking. This is usually followed by chemotherapy with platinum-based drugs such as cisplatin or carboplatin, often in combination with paclitaxel.
Prognosis[edit]
The prognosis for patients with HGSC is generally poor, with a five-year survival rate of less than 50%. The high recurrence rate and the development of chemoresistance contribute to the challenging nature of treating this disease. Ongoing research is focused on identifying new therapeutic targets and improving early detection methods.
Research and Future Directions[edit]
Current research in HGSC is exploring the role of PARP inhibitors in patients with BRCA mutations, as well as the potential of immunotherapy and targeted therapy to improve outcomes. Efforts are also being made to develop better screening tools to detect HGSC at an earlier, more treatable stage.
See Also[edit]
References[edit]
<references group="" responsive="1"></references>
External Links[edit]
