Cystic hygroma: Difference between revisions
CSV import |
CSV import Tags: mobile edit mobile web edit |
||
| Line 1: | Line 1: | ||
[[file:Cystic_Hygroma_(cropped).jpg|thumb | {{SI}} | ||
{{Infobox medical condition | |||
| name = Cystic hygroma | |||
| image = [[File:Cystic_Hygroma_(cropped).jpg|250px]] | |||
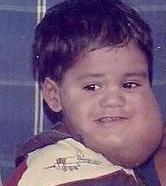
| caption = Cystic hygroma in a child | |||
| field = [[Medical genetics]], [[Pediatrics]] | |||
| synonyms = [[Lymphatic malformation]], [[Cystic lymphangioma]] | |||
| symptoms = Soft, painless swelling, usually in the neck or armpit | |||
| complications = [[Infection]], [[Airway obstruction]], [[Cosmetic deformity]] | |||
| onset = Congenital (present at birth) | |||
| duration = Persistent | |||
| causes = Abnormal development of the [[lymphatic system]] | |||
| risks = [[Turner syndrome]], [[Down syndrome]], [[Noonan syndrome]] | |||
| diagnosis = [[Ultrasound]], [[MRI]], [[CT scan]] | |||
| differential = [[Thyroglossal duct cyst]], [[Branchial cleft cyst]], [[Hemangioma]] | |||
| treatment = [[Surgical excision]], [[Sclerotherapy]] | |||
| prognosis = Variable, depending on size and location | |||
| frequency = Rare | |||
}} | |||
[[file:Cystic_Hygroma_(cropped).jpg|left|thumb]] [[file:Copy_of_Musculi_coli_base,_my_edits_for_tringles,_labeled_triangles,posterior.svg|left|thumb]] [[file:Newborn_infant_with_a_cystic_hygroma_(cropped).jpg|left|thumb]] [[file:Lymphangioma_After_7_Surgeries.jpg|left|thumb]] '''Cystic hygroma''' is a congenital malformation of the [[lymphatic system]], characterized by fluid-filled sacs, typically located in the [[neck]] and [[head]] region. These sacs, or cysts, are caused by blockages in the lymphatic system, leading to the accumulation of lymphatic fluid. | |||
==Presentation== | ==Presentation== | ||
Cystic hygromas are often present at birth, but they can also develop later in life. They are usually identified through prenatal [[ultrasound]] or during a physical examination after birth. The cysts can vary in size and may grow over time. Large cystic hygromas can cause complications by compressing nearby structures, such as the [[trachea]] and [[esophagus]], leading to difficulties in [[breathing]] and [[swallowing]]. | Cystic hygromas are often present at birth, but they can also develop later in life. They are usually identified through prenatal [[ultrasound]] or during a physical examination after birth. The cysts can vary in size and may grow over time. Large cystic hygromas can cause complications by compressing nearby structures, such as the [[trachea]] and [[esophagus]], leading to difficulties in [[breathing]] and [[swallowing]]. | ||
==Causes== | ==Causes== | ||
The exact cause of cystic hygroma is not well understood, but it is believed to result from abnormal development of the lymphatic system during embryonic growth. Genetic factors may play a role, and cystic hygromas are sometimes associated with chromosomal abnormalities such as [[Turner syndrome]], [[Down syndrome]], and [[Noonan syndrome]]. | The exact cause of cystic hygroma is not well understood, but it is believed to result from abnormal development of the lymphatic system during embryonic growth. Genetic factors may play a role, and cystic hygromas are sometimes associated with chromosomal abnormalities such as [[Turner syndrome]], [[Down syndrome]], and [[Noonan syndrome]]. | ||
==Diagnosis== | ==Diagnosis== | ||
Diagnosis of cystic hygroma is typically made through imaging studies. [[Ultrasound]] is the most common diagnostic tool used prenatally. Postnatally, [[magnetic resonance imaging]] (MRI) and [[computed tomography]] (CT) scans can provide detailed images of the cystic structures and their relationship to surrounding tissues. | Diagnosis of cystic hygroma is typically made through imaging studies. [[Ultrasound]] is the most common diagnostic tool used prenatally. Postnatally, [[magnetic resonance imaging]] (MRI) and [[computed tomography]] (CT) scans can provide detailed images of the cystic structures and their relationship to surrounding tissues. | ||
==Treatment== | ==Treatment== | ||
The treatment of cystic hygroma depends on the size and location of the cysts, as well as the presence of any complications. Small, asymptomatic cysts may not require immediate treatment and can be monitored over time. Larger cysts or those causing symptoms may require intervention. Treatment options include: | The treatment of cystic hygroma depends on the size and location of the cysts, as well as the presence of any complications. Small, asymptomatic cysts may not require immediate treatment and can be monitored over time. Larger cysts or those causing symptoms may require intervention. Treatment options include: | ||
* [[Surgical excision]]: Complete removal of the cystic hygroma is often the preferred treatment, especially if it is causing significant symptoms. | * [[Surgical excision]]: Complete removal of the cystic hygroma is often the preferred treatment, especially if it is causing significant symptoms. | ||
* [[Sclerotherapy]]: Injection of a sclerosing agent into the cyst to shrink it. | * [[Sclerotherapy]]: Injection of a sclerosing agent into the cyst to shrink it. | ||
* [[Laser therapy]]: Use of laser to reduce the size of the cyst. | * [[Laser therapy]]: Use of laser to reduce the size of the cyst. | ||
==Prognosis== | ==Prognosis== | ||
The prognosis for individuals with cystic hygroma varies depending on the size and location of the cysts and the presence of any associated anomalies. Early detection and appropriate treatment can improve outcomes. However, large cystic hygromas or those associated with genetic syndromes may have a more guarded prognosis. | The prognosis for individuals with cystic hygroma varies depending on the size and location of the cysts and the presence of any associated anomalies. Early detection and appropriate treatment can improve outcomes. However, large cystic hygromas or those associated with genetic syndromes may have a more guarded prognosis. | ||
==See also== | ==See also== | ||
* [[Lymphatic system]] | * [[Lymphatic system]] | ||
| Line 26: | Line 38: | ||
* [[Noonan syndrome]] | * [[Noonan syndrome]] | ||
* [[Congenital disorder]] | * [[Congenital disorder]] | ||
==References== | ==References== | ||
{{Reflist}} | {{Reflist}} | ||
==External links== | ==External links== | ||
{{Commons category|Cystic hygroma}} | {{Commons category|Cystic hygroma}} | ||
[[Category:Congenital disorders]] | [[Category:Congenital disorders]] | ||
[[Category:Lymphatic system]] | [[Category:Lymphatic system]] | ||
[[Category:Pediatrics]] | [[Category:Pediatrics]] | ||
[[Category:Medical conditions]] | [[Category:Medical conditions]] | ||
{{medicine-stub}} | {{medicine-stub}} | ||
Latest revision as of 13:48, 5 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Cystic hygroma | |
|---|---|
| |
| Synonyms | Lymphatic malformation, Cystic lymphangioma |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Soft, painless swelling, usually in the neck or armpit |
| Complications | Infection, Airway obstruction, Cosmetic deformity |
| Onset | Congenital (present at birth) |
| Duration | Persistent |
| Types | N/A |
| Causes | Abnormal development of the lymphatic system |
| Risks | Turner syndrome, Down syndrome, Noonan syndrome |
| Diagnosis | Ultrasound, MRI, CT scan |
| Differential diagnosis | Thyroglossal duct cyst, Branchial cleft cyst, Hemangioma |
| Prevention | N/A |
| Treatment | Surgical excision, Sclerotherapy |
| Medication | N/A |
| Prognosis | Variable, depending on size and location |
| Frequency | Rare |
| Deaths | N/A |



Cystic hygroma is a congenital malformation of the lymphatic system, characterized by fluid-filled sacs, typically located in the neck and head region. These sacs, or cysts, are caused by blockages in the lymphatic system, leading to the accumulation of lymphatic fluid.
Presentation[edit]
Cystic hygromas are often present at birth, but they can also develop later in life. They are usually identified through prenatal ultrasound or during a physical examination after birth. The cysts can vary in size and may grow over time. Large cystic hygromas can cause complications by compressing nearby structures, such as the trachea and esophagus, leading to difficulties in breathing and swallowing.
Causes[edit]
The exact cause of cystic hygroma is not well understood, but it is believed to result from abnormal development of the lymphatic system during embryonic growth. Genetic factors may play a role, and cystic hygromas are sometimes associated with chromosomal abnormalities such as Turner syndrome, Down syndrome, and Noonan syndrome.
Diagnosis[edit]
Diagnosis of cystic hygroma is typically made through imaging studies. Ultrasound is the most common diagnostic tool used prenatally. Postnatally, magnetic resonance imaging (MRI) and computed tomography (CT) scans can provide detailed images of the cystic structures and their relationship to surrounding tissues.
Treatment[edit]
The treatment of cystic hygroma depends on the size and location of the cysts, as well as the presence of any complications. Small, asymptomatic cysts may not require immediate treatment and can be monitored over time. Larger cysts or those causing symptoms may require intervention. Treatment options include:
- Surgical excision: Complete removal of the cystic hygroma is often the preferred treatment, especially if it is causing significant symptoms.
- Sclerotherapy: Injection of a sclerosing agent into the cyst to shrink it.
- Laser therapy: Use of laser to reduce the size of the cyst.
Prognosis[edit]
The prognosis for individuals with cystic hygroma varies depending on the size and location of the cysts and the presence of any associated anomalies. Early detection and appropriate treatment can improve outcomes. However, large cystic hygromas or those associated with genetic syndromes may have a more guarded prognosis.
See also[edit]
References[edit]
<references group="" responsive="1"></references>
External links[edit]
