Posterior vitreous detachment

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Posterior vitreous detachment | |
|---|---|
| |
| Synonyms | PVD |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Floaters, flashes of light, visual impairment |
| Complications | Retinal detachment, macular hole |
| Onset | Typically after age 50 |
| Duration | Permanent |
| Types | N/A |
| Causes | Aging, myopia, trauma |
| Risks | Age, myopia, eye surgery |
| Diagnosis | Ophthalmoscopy, ultrasound |
| Differential diagnosis | Retinal detachment, vitreous hemorrhage |
| Prevention | N/A |
| Treatment | Usually none, vitrectomy if complications occur |
| Medication | N/A |
| Prognosis | Generally good, but complications can occur |
| Frequency | Common in older adults |
| Deaths | N/A |
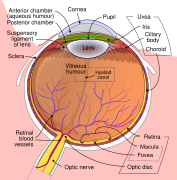
Posterior Vitreous Detachment (PVD) is an eye condition where the vitreous membrane separates from the retina. It primarily occurs as a natural part of aging.
Pathophysiology[edit]
PVD involves the separation of the posterior hyaloid membrane from the retina posterior to the vitreous base, a 3-4 mm attachment to the ora serrata. The process is often due to changes in the vitreous humor consistency and volume with age.
Epidemiology[edit]
- Prevalence in Older Adults
Over 75% of individuals over the age of 65 experience PVD. The condition becomes increasingly common with advancing age.
- Occurrence in Middle-Aged Individuals
While less frequent in people in their 40s and 50s, PVD is not uncommon in this age group.
- Gender Differences
Some studies indicate a higher prevalence of PVD in women compared to men.
Clinical Features[edit]
Symptoms of PVD can include:
- Floaters
- Flashes of light
- A ring-shaped floater, indicative of a Weiss ring
Diagnosis[edit]
Diagnosis of PVD is primarily based on patient history and a comprehensive eye examination, including:
- Ophthalmoscopy
- Slit lamp examination
- OCT scans in some cases
Management and Prognosis[edit]
Most cases of PVD are benign and do not require treatment. However, patients should be monitored for complications like:
Patient Education[edit]
Patients with PVD should be educated about symptoms of retinal detachment and the importance of timely ophthalmologic evaluation if these symptoms occur.
References[edit]
- Johnson, M. W. (2010). Posterior vitreous detachment: Evolution and complications of its early stages. American Journal of Ophthalmology, 149(3), 371-382.
- Hikichi, T., Yoshida, A., & Akiba, J. (1995). Rate of posterior vitreous detachment in women with idiopathic macular hole. Archives of Ophthalmology, 113(6), 724-728.
See Also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian