Usual interstitial pneumonia

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Usual interstitial pneumonia | |
|---|---|

| |
| Synonyms | UIP |
| Pronounce | N/A |
| Specialty | Pulmonology |
| Symptoms | Shortness of breath, dry cough, fatigue |
| Complications | Pulmonary hypertension, respiratory failure |
| Onset | Typically in adults over 50 |
| Duration | Chronic |
| Types | N/A |
| Causes | Idiopathic, connective tissue disease, asbestosis, chronic hypersensitivity pneumonitis |
| Risks | Smoking, environmental exposure, genetic predisposition |
| Diagnosis | HRCT, lung biopsy |
| Differential diagnosis | Nonspecific interstitial pneumonia, hypersensitivity pneumonitis, sarcoidosis |
| Prevention | N/A |
| Treatment | Antifibrotic therapy, oxygen therapy, lung transplantation |
| Medication | N/A |
| Prognosis | Variable, often poor |
| Frequency | Rare |
| Deaths | N/A |




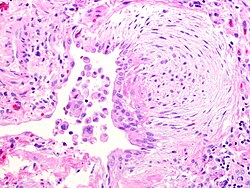
Usual interstitial pneumonia (UIP) is a specific form of lung disease characterized by progressive scarring of both lungs. It is the most common form of idiopathic pulmonary fibrosis (IPF), a type of interstitial lung disease.
Clinical Features[edit]
Patients with UIP typically present with dyspnea (shortness of breath) and a persistent dry cough. The disease is more common in older adults, particularly those over the age of 50. Physical examination may reveal clubbing of the fingers and crackles on lung auscultation.
Pathology[edit]
The hallmark of UIP is the presence of patchy interstitial fibrosis, which is most pronounced in the subpleural and basal regions of the lungs. Histologically, UIP is characterized by the presence of fibroblastic foci, honeycomb change, and temporal heterogeneity of fibrosis.
Diagnosis[edit]
Diagnosis of UIP is typically made through a combination of clinical, radiological, and pathological findings. High-resolution computed tomography (HRCT) scans of the chest are crucial for diagnosis, often showing a pattern of reticular opacities, traction bronchiectasis, and honeycombing. A lung biopsy may be performed to confirm the diagnosis.
Treatment[edit]
There is no cure for UIP, and treatment is primarily supportive. Antifibrotic medications such as pirfenidone and nintedanib may slow disease progression. Lung transplantation is an option for eligible patients with advanced disease.
Prognosis[edit]
The prognosis for patients with UIP is generally poor, with a median survival of 3 to 5 years after diagnosis. The disease course is variable, with some patients experiencing rapid progression and others having a more indolent course.
See also[edit]
| Pulmonology topics | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
This pulmonology-related article is a stub. You can help WikiMD by expanding it.
|
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian