Crigler–Najjar syndrome

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Crigler–Najjar syndrome | |
|---|---|
| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Jaundice, kernicterus |
| Complications | Neurological damage |
| Onset | Neonatal |
| Duration | Lifelong |
| Types | Type I, Type II |
| Causes | Genetic mutation in the UGT1A1 gene |
| Risks | Consanguinity |
| Diagnosis | Genetic testing, liver function tests |
| Differential diagnosis | Gilbert's syndrome, Dubin-Johnson syndrome, Rotor syndrome |
| Prevention | N/A |
| Treatment | Phototherapy, liver transplantation, phenobarbital (Type II) |
| Medication | N/A |
| Prognosis | Variable, depends on type and treatment |
| Frequency | Rare |
| Deaths | Can be fatal if untreated |
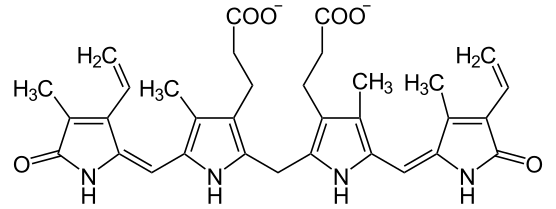
Crigler–Najjar syndrome is a rare genetic disorder characterized by a severe form of hyperbilirubinemia due to a deficiency in the enzyme UDP-glucuronosyltransferase (UGT1A1). This enzyme is crucial for the conjugation and subsequent excretion of bilirubin, a byproduct of hemoglobin breakdown. The syndrome is named after Dr. John Fielding Crigler and Dr. Victor Assad Najjar, who first described the condition in 1952.
Pathophysiology[edit]
Crigler–Najjar syndrome results from mutations in the UGT1A1 gene, leading to impaired bilirubin conjugation. This results in the accumulation of unconjugated bilirubin in the blood, causing jaundice and potentially leading to kernicterus, a form of brain damage.
Types[edit]
Crigler–Najjar syndrome is classified into two types:
Type I[edit]
Type I is the more severe form, characterized by a complete absence of UGT1A1 activity. Patients with Type I Crigler–Najjar syndrome have very high levels of unconjugated bilirubin and are at significant risk for kernicterus. This type does not respond to phenobarbital treatment.
Type II[edit]
Type II, also known as Arias syndrome, is less severe and results from partial UGT1A1 activity. Patients with Type II have lower levels of bilirubin and a reduced risk of kernicterus. This type often responds to phenobarbital, which can induce enzyme activity and lower bilirubin levels.
Clinical Presentation[edit]
The primary symptom of Crigler–Najjar syndrome is persistent jaundice, which is evident shortly after birth. In Type I, jaundice is severe and persistent, while in Type II, it may be milder.
Diagnosis[edit]
Diagnosis is based on clinical presentation, family history, and laboratory tests showing elevated levels of unconjugated bilirubin. Genetic testing can confirm mutations in the UGT1A1 gene.
Treatment[edit]
Type I[edit]
Management of Type I Crigler–Najjar syndrome includes aggressive phototherapy to reduce bilirubin levels and prevent kernicterus. Liver transplantation may be considered as a definitive treatment.
Type II[edit]
Type II can often be managed with phenobarbital, which helps to induce residual UGT1A1 activity and lower bilirubin levels.
Prognosis[edit]
The prognosis for Crigler–Najjar syndrome varies depending on the type. Type I has a high risk of neurological damage if not managed effectively, while Type II generally has a better prognosis with appropriate treatment.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian