Hormonal intrauterine device: Difference between revisions
CSV import |
CSV import |
||
| Line 32: | Line 32: | ||
{{Medicine-stub}} | {{Medicine-stub}} | ||
==Hormonal_intrauterine_device== | |||
<gallery> | |||
File:Mirena_IUD_2011.jpg|Mirena IUD 2011 | |||
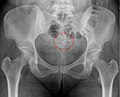
File:Mirena_IUD_-_Roe_Becken_ap.jpg|Mirena IUD - Roe Becken AP | |||
File:Mirena_in_optimal_place_-_schematic.png|Mirena in optimal place - schematic | |||
File:Mirena_in_optimal_place_-_ultrasound.jpg|Mirena in optimal place - ultrasound | |||
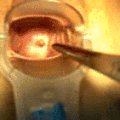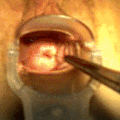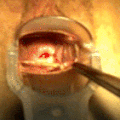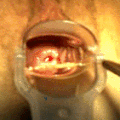
File:Mirena_intrauterine_device_insertion.jpg|Mirena intrauterine device insertion | |||
File:Removal_of_IUD_with_progestogen.gif|Removal of IUD with progestogen | |||
</gallery> | |||
Revision as of 11:09, 18 February 2025
Hormonal Intrauterine Device
The Hormonal Intrauterine Device (IUD), also known as a levonorgestrel intrauterine system (LNG-IUS), is a form of reversible long-acting contraception that releases the hormone Levonorgestrel directly into the uterus. Its primary function is to prevent pregnancy, and it is one of the most effective forms of birth control available, with a first-year failure rate around 0.1-0.4%. The device is a small T-shaped piece of plastic that is inserted into the uterus by a healthcare provider. It can remain in place for 3 to 7 years, depending on the specific product.
Mechanism of Action
The hormonal IUD works by releasing levonorgestrel, which thickens the cervical mucus, preventing sperm from reaching an egg. It also thins the lining of the uterus (endometrium), making it less suitable for a fertilized egg to implant and develop. In some cases, it can also inhibit the release of eggs from the ovaries (ovulation), but this is not its primary mechanism of action.
Types
Several brands of hormonal IUDs are available, including Mirena, Kyleena, Skyla, and Liletta. Each brand has a different amount of levonorgestrel and duration of effectiveness.
Benefits
Beyond contraception, hormonal IUDs offer several health benefits. They are used to treat heavy menstrual bleeding, reduce menstrual cramps, and, in some cases, treat symptoms of Endometriosis. Additionally, they can decrease the risk of Endometrial Cancer.
Side Effects
Common side effects include irregular bleeding, spotting between periods, and decreased menstrual flow or cessation of periods altogether. Some users may experience hormonal side effects such as headaches, acne, breast tenderness, and mood changes. Serious but rare side effects include uterine perforation and pelvic inflammatory disease.
Insertion and Removal
The insertion of a hormonal IUD is a medical procedure that should be performed by a trained healthcare provider. The process typically takes a few minutes and can cause discomfort or pain, for which pain relief can be provided. Removal is simpler and usually less painful, requiring a healthcare provider to gently pull on the strings attached to the IUD.
Contraindications
Not everyone is a suitable candidate for a hormonal IUD. Contraindications include pregnancy, unexplained vaginal bleeding, cervical or uterine cancer, liver disease, or a history of Pelvic Inflammatory Disease (PID).
Comparison with Other Methods
Compared to other forms of contraception, the hormonal IUD is more effective than Birth Control Pills, patches, and vaginal rings, mainly because it eliminates the possibility of user error. However, unlike Condoms, it does not provide protection against Sexually Transmitted Infections (STIs).
Conclusion
The hormonal intrauterine device is a highly effective, long-term contraceptive option that offers several benefits beyond birth control. However, it is important for individuals to consult with a healthcare provider to determine if it is the right choice for them, considering potential side effects and contraindications.
Hormonal_intrauterine_device
-
Mirena IUD 2011
-
Mirena IUD - Roe Becken AP
-
Mirena in optimal place - schematic
-
Mirena in optimal place - ultrasound
-
Mirena intrauterine device insertion
-
Removal of IUD with progestogen