Posterior vitreous detachment: Difference between revisions
CSV import |
CSV import |
||
| Line 19: | Line 19: | ||
}} | }} | ||
[[File:PVD-CVD.jpg|left|thumb|Illustration of Posterior Vitreous Detachment]] | [[File:PVD-CVD.jpg|left|thumb|Illustration of Posterior Vitreous Detachment]] | ||
'''Posterior Vitreous Detachment''' (PVD) is an eye condition where the [[Vitreous body|vitreous membrane]] separates from the [[Retina|retina]]. It primarily occurs as a natural part of aging. | '''Posterior Vitreous Detachment''' (PVD) is an eye condition where the [[Vitreous body|vitreous membrane]] separates from the [[Retina|retina]]. It primarily occurs as a natural part of aging. | ||
== Pathophysiology == | == Pathophysiology == | ||
Latest revision as of 12:51, 12 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Posterior vitreous detachment | |
|---|---|
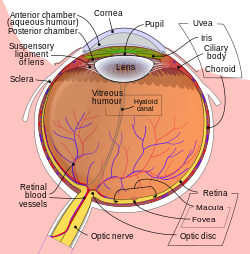
| |
| Synonyms | PVD |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Floaters, flashes of light, visual impairment |
| Complications | Retinal detachment, macular hole |
| Onset | Typically after age 50 |
| Duration | Permanent |
| Types | N/A |
| Causes | Aging, myopia, trauma |
| Risks | Age, myopia, eye surgery |
| Diagnosis | Ophthalmoscopy, ultrasound |
| Differential diagnosis | Retinal detachment, vitreous hemorrhage |
| Prevention | N/A |
| Treatment | Usually none, vitrectomy if complications occur |
| Medication | N/A |
| Prognosis | Generally good, but complications can occur |
| Frequency | Common in older adults |
| Deaths | N/A |

Posterior Vitreous Detachment (PVD) is an eye condition where the vitreous membrane separates from the retina. It primarily occurs as a natural part of aging.
Pathophysiology[edit]
PVD involves the separation of the posterior hyaloid membrane from the retina posterior to the vitreous base, a 3-4 mm attachment to the ora serrata. The process is often due to changes in the vitreous humor consistency and volume with age.
Epidemiology[edit]
- Prevalence in Older Adults
Over 75% of individuals over the age of 65 experience PVD. The condition becomes increasingly common with advancing age.
- Occurrence in Middle-Aged Individuals
While less frequent in people in their 40s and 50s, PVD is not uncommon in this age group.
- Gender Differences
Some studies indicate a higher prevalence of PVD in women compared to men.
Clinical Features[edit]
Symptoms of PVD can include:
- Floaters
- Flashes of light
- A ring-shaped floater, indicative of a Weiss ring
Diagnosis[edit]
Diagnosis of PVD is primarily based on patient history and a comprehensive eye examination, including:
- Ophthalmoscopy
- Slit lamp examination
- OCT scans in some cases
Management and Prognosis[edit]
Most cases of PVD are benign and do not require treatment. However, patients should be monitored for complications like:
Patient Education[edit]
Patients with PVD should be educated about symptoms of retinal detachment and the importance of timely ophthalmologic evaluation if these symptoms occur.
References[edit]
- Johnson, M. W. (2010). Posterior vitreous detachment: Evolution and complications of its early stages. American Journal of Ophthalmology, 149(3), 371-382.
- Hikichi, T., Yoshida, A., & Akiba, J. (1995). Rate of posterior vitreous detachment in women with idiopathic macular hole. Archives of Ophthalmology, 113(6), 724-728.


