Transplant rejection: Difference between revisions
mNo edit summary |
CSV import |
||
| Line 1: | Line 1: | ||
{{SI}} | |||
{{Infobox medical condition | |||
| name = Transplant rejection | |||
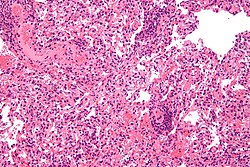
| image = [[File:Lung_transplant_rejection_-_high_mag.jpg|250px]] | |||
| caption = Histopathology of lung transplant rejection | |||
| field = [[Transplant surgery]], [[Immunology]] | |||
| symptoms = [[Fever]], [[graft dysfunction]], [[pain]] at transplant site | |||
| complications = [[Graft failure]], [[chronic rejection]] | |||
| onset = Varies (can be acute or chronic) | |||
| duration = Varies | |||
| types = [[Hyperacute rejection]], [[Acute rejection]], [[Chronic rejection]] | |||
| causes = [[Immune response]] against transplanted organ | |||
| risks = [[HLA mismatch]], [[non-adherence]] to immunosuppressive therapy | |||
| diagnosis = [[Biopsy]], [[blood tests]], [[imaging studies]] | |||
| treatment = [[Immunosuppressive drugs]], [[plasmapheresis]], [[antibody therapy]] | |||
| prognosis = Depends on type and severity | |||
| frequency = Common in transplant recipients | |||
}} | |||
== Introduction == | == Introduction == | ||
'''Transplant rejection''' is a physiological response wherein the recipient's immune system identifies and attacks the transplanted tissue or organ, perceiving it as a foreign entity. It is a common challenge in the field of [[transplantation medicine]] and can have severe implications for the recipient. | '''Transplant rejection''' is a physiological response wherein the recipient's immune system identifies and attacks the transplanted tissue or organ, perceiving it as a foreign entity. It is a common challenge in the field of [[transplantation medicine]] and can have severe implications for the recipient. | ||
[[File:Transplant glomerulopathy - very high mag.jpg|left|thumb|Illustration depicting the immune response during transplant rejection.]] | |||
[[File:Transplant glomerulopathy - very high mag.jpg|thumb | |||
== Understanding the Immune Response == | == Understanding the Immune Response == | ||
The human body has a robust immune system designed to ward off foreign invaders such as bacteria, viruses, and other pathogens. However, this system can also recognize transplanted organs or tissues as foreign, leading to rejection. | The human body has a robust immune system designed to ward off foreign invaders such as bacteria, viruses, and other pathogens. However, this system can also recognize transplanted organs or tissues as foreign, leading to rejection. | ||
=== Types of Rejection === | === Types of Rejection === | ||
Transplant rejection can be categorized into several types based on the onset and severity: | Transplant rejection can be categorized into several types based on the onset and severity: | ||
* '''Hyperacute Rejection:''' Occurs within minutes to hours post-transplant. It is primarily due to pre-existing antibodies in the recipient against the donor tissue. | * '''Hyperacute Rejection:''' Occurs within minutes to hours post-transplant. It is primarily due to pre-existing antibodies in the recipient against the donor tissue. | ||
* '''Acute Rejection:''' Emerges days to weeks after the transplant. It's the most common type and is mainly caused by T cells of the immune system. | * '''Acute Rejection:''' Emerges days to weeks after the transplant. It's the most common type and is mainly caused by T cells of the immune system. | ||
* '''Chronic Rejection:''' Manifests over months to years and is less understood. It is believed to be an antibody-mediated response leading to gradual loss of graft function. | * '''Chronic Rejection:''' Manifests over months to years and is less understood. It is believed to be an antibody-mediated response leading to gradual loss of graft function. | ||
== Reducing the Risk of Rejection == | == Reducing the Risk of Rejection == | ||
=== Molecular Compatibility === | === Molecular Compatibility === | ||
One of the primary strategies to reduce the risk of transplant rejection is to ensure molecular compatibility between the donor and the recipient. This is achieved through: | One of the primary strategies to reduce the risk of transplant rejection is to ensure molecular compatibility between the donor and the recipient. This is achieved through: | ||
* '''[[HLA Typing]]:''' A test that identifies the human leukocyte antigen (HLA) molecules on the cells of both donor and recipient. A close HLA match can significantly reduce the risk of rejection. | * '''[[HLA Typing]]:''' A test that identifies the human leukocyte antigen (HLA) molecules on the cells of both donor and recipient. A close HLA match can significantly reduce the risk of rejection. | ||
[[File:HLA-DQ0602.png|left|thumb|A depiction of HLA typing procedure.]] | |||
[[File:HLA-DQ0602.png|thumb | |||
=== Immunosuppressive Therapy === | === Immunosuppressive Therapy === | ||
Post-transplant, recipients are typically prescribed [[immunosuppressant drugs]]. These drugs: | Post-transplant, recipients are typically prescribed [[immunosuppressant drugs]]. These drugs: | ||
* Dampen the immune response, reducing the risk of rejection. | * Dampen the immune response, reducing the risk of rejection. | ||
* Require careful monitoring, as they can lead to increased susceptibility to infections and other side effects. | * Require careful monitoring, as they can lead to increased susceptibility to infections and other side effects. | ||
== Conclusion == | == Conclusion == | ||
Transplant rejection is a complex interplay between the graft and the recipient's immune system. With advancements in molecular testing and the development of effective immunosuppressants, the outcomes for transplant recipients have substantially improved over the years. Still, continuous research is vital to further understand the mechanisms of rejection and devise strategies to prevent it. | Transplant rejection is a complex interplay between the graft and the recipient's immune system. With advancements in molecular testing and the development of effective immunosuppressants, the outcomes for transplant recipients have substantially improved over the years. Still, continuous research is vital to further understand the mechanisms of rejection and devise strategies to prevent it. | ||
[[Category:Medical Conditions]] | [[Category:Medical Conditions]] | ||
[[Category:Immunology]] | [[Category:Immunology]] | ||
[[Category:Transplantation Medicine]] | [[Category:Transplantation Medicine]] | ||
{{stub}} | {{stub}} | ||
Latest revision as of 20:49, 8 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Transplant rejection | |
|---|---|
| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Fever, graft dysfunction, pain at transplant site |
| Complications | Graft failure, chronic rejection |
| Onset | Varies (can be acute or chronic) |
| Duration | Varies |
| Types | Hyperacute rejection, Acute rejection, Chronic rejection |
| Causes | Immune response against transplanted organ |
| Risks | HLA mismatch, non-adherence to immunosuppressive therapy |
| Diagnosis | Biopsy, blood tests, imaging studies |
| Differential diagnosis | N/A |
| Prevention | N/A |
| Treatment | Immunosuppressive drugs, plasmapheresis, antibody therapy |
| Medication | N/A |
| Prognosis | Depends on type and severity |
| Frequency | Common in transplant recipients |
| Deaths | N/A |
Introduction[edit]
Transplant rejection is a physiological response wherein the recipient's immune system identifies and attacks the transplanted tissue or organ, perceiving it as a foreign entity. It is a common challenge in the field of transplantation medicine and can have severe implications for the recipient.

Understanding the Immune Response[edit]
The human body has a robust immune system designed to ward off foreign invaders such as bacteria, viruses, and other pathogens. However, this system can also recognize transplanted organs or tissues as foreign, leading to rejection.
Types of Rejection[edit]
Transplant rejection can be categorized into several types based on the onset and severity:
- Hyperacute Rejection: Occurs within minutes to hours post-transplant. It is primarily due to pre-existing antibodies in the recipient against the donor tissue.
- Acute Rejection: Emerges days to weeks after the transplant. It's the most common type and is mainly caused by T cells of the immune system.
- Chronic Rejection: Manifests over months to years and is less understood. It is believed to be an antibody-mediated response leading to gradual loss of graft function.
Reducing the Risk of Rejection[edit]
Molecular Compatibility[edit]
One of the primary strategies to reduce the risk of transplant rejection is to ensure molecular compatibility between the donor and the recipient. This is achieved through:
- HLA Typing: A test that identifies the human leukocyte antigen (HLA) molecules on the cells of both donor and recipient. A close HLA match can significantly reduce the risk of rejection.

Immunosuppressive Therapy[edit]
Post-transplant, recipients are typically prescribed immunosuppressant drugs. These drugs:
- Dampen the immune response, reducing the risk of rejection.
- Require careful monitoring, as they can lead to increased susceptibility to infections and other side effects.
Conclusion[edit]
Transplant rejection is a complex interplay between the graft and the recipient's immune system. With advancements in molecular testing and the development of effective immunosuppressants, the outcomes for transplant recipients have substantially improved over the years. Still, continuous research is vital to further understand the mechanisms of rejection and devise strategies to prevent it.


