Solid pseudopapillary tumour

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's weight loss doctor NYC
Philadelphia GLP-1 weight loss and GLP-1 clinic NYC
| Solid pseudopapillary tumour | |
|---|---|
| Synonyms | Solid pseudopapillary neoplasm, solid and papillary epithelial neoplasm, papillary cystic neoplasm |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Abdominal pain, palpable mass, nausea, vomiting |
| Complications | Metastasis, recurrence |
| Onset | Typically in young women |
| Duration | Variable |
| Types | |
| Causes | Unknown |
| Risks | Female gender, young age |
| Diagnosis | Imaging studies, biopsy |
| Differential diagnosis | Pancreatic neuroendocrine tumor, pancreatic adenocarcinoma, cystic pancreatic lesions |
| Prevention | None |
| Treatment | Surgical resection |
| Medication | |
| Prognosis | Generally favorable with treatment |
| Frequency | Rare |
| Deaths | N/A |
A rare type of pancreatic tumor
Solid pseudopapillary tumour (SPT), also known as solid pseudopapillary neoplasm (SPN), is a rare type of pancreatic neoplasm that primarily affects young women. It is characterized by its low malignant potential and distinctive histological features.
Epidemiology[edit]
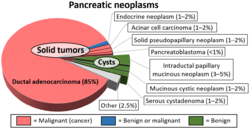
SPT accounts for approximately 1-2% of all pancreatic tumors. It predominantly occurs in young females, with a mean age of diagnosis around 30 years. Although rare, it can also occur in males and older individuals.]]
Pathophysiology[edit]
The exact pathogenesis of SPT is not well understood. However, it is believed to arise from the pancreatic ductal epithelium. Genetic studies have shown mutations in the CTNNB1 gene, which encodes for beta-catenin, a protein involved in the Wnt signaling pathway.
Histopathology[edit]
SPT is characterized by a combination of solid and pseudopapillary patterns. The tumor cells are typically arranged around blood vessels, forming pseudopapillae. The presence of these pseudopapillae is a hallmark of the tumor.]]
]]
Cytopathology[edit]
On cytological examination, SPT shows a mixture of solid and cystic areas. The cells are usually uniform with eosinophilic cytoplasm and round to oval nuclei. Nuclear grooves and intranuclear cytoplasmic inclusions may be present.]]
Immunohistochemistry[edit]
SPT typically shows positive staining for beta-catenin, vimentin, and CD10. The nuclear accumulation of beta-catenin is a characteristic finding.]]
Clinical Presentation[edit]
Patients with SPT often present with non-specific symptoms such as abdominal pain or a palpable abdominal mass. Due to its indolent nature, the tumor may grow to a large size before detection.
Diagnosis[edit]
Diagnosis of SPT is typically made through imaging studies such as CT scan or MRI, followed by histological examination of a biopsy or surgical specimen.
Treatment[edit]
The primary treatment for SPT is surgical resection. Due to its low malignant potential, complete surgical removal often results in a good prognosis. Recurrence is rare but can occur.
Prognosis[edit]
The prognosis for patients with SPT is generally favorable, with a high survival rate following complete surgical resection. Malignant transformation and metastasis are uncommon.
See also[edit]
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian