Frontotemporal dementia

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Frontotemporal dementia | |
|---|---|
| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Behavioral changes, language difficulties, memory loss |
| Complications | N/A |
| Onset | Typically between ages 45 and 65 |
| Duration | Progressive |
| Types | Behavioral variant, Primary progressive aphasia |
| Causes | Genetic mutations, tau protein abnormalities |
| Risks | Family history, certain genetic mutations |
| Diagnosis | Neuroimaging, neuropsychological testing, genetic testing |
| Differential diagnosis | Alzheimer's disease, vascular dementia, psychiatric disorders |
| Prevention | N/A |
| Treatment | Supportive care, medications for symptoms |
| Medication | N/A |
| Prognosis | Progressive decline, variable life expectancy |
| Frequency | 15-22 per 100,000 people |
| Deaths | N/A |
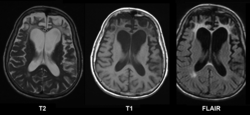
A type of dementia affecting the frontal and temporal lobes of the brain
Frontotemporal dementia (FTD) is a group of brain disorders caused by progressive cell degeneration in the brain's frontal lobes or its temporal lobes. These areas of the brain are generally associated with personality, behavior, and language.
Introduction
Frontotemporal dementia is characterized by a gradual, progressive decline in behavior and/or language. The symptoms can vary significantly from person to person, depending on which parts of the frontal and temporal lobes are affected. Unlike other forms of dementia, memory is often relatively preserved in the early stages of FTD.
Types of Frontotemporal Dementia
FTD is classified into several subtypes based on the symptoms and the areas of the brain affected:
Behavioral Variant FTD
This is the most common form of FTD, marked by changes in personality, behavior, and judgment. Patients may exhibit socially inappropriate behavior, apathy, or loss of empathy.
Primary Progressive Aphasia
This subtype affects language skills, including speaking, writing, and comprehension. It is further divided into:
- Semantic variant PPA: Characterized by loss of word meaning.
- Nonfluent/agrammatic variant PPA: Marked by difficulty in forming words and sentences.
FTD with Motor Neuron Disease
Some individuals with FTD also develop motor neuron disease, which affects movement and muscle function.
Pathophysiology
The underlying cause of FTD is the accumulation of abnormal proteins in the brain, such as tau or TDP-43. These proteins form clumps that disrupt normal cell function and lead to cell death. The specific pattern of protein accumulation can vary, leading to the different subtypes of FTD.
Diagnosis
Diagnosis of FTD is based on clinical evaluation, neuropsychological testing, and brain imaging. MRI and PET scans can help identify patterns of brain atrophy typical of FTD. Genetic testing may be recommended if there is a family history of the disease.
Management
There is currently no cure for FTD, and treatment focuses on managing symptoms. This may include medications to address behavioral symptoms, speech therapy for language difficulties, and supportive care to improve quality of life.
Prognosis
FTD is a progressive disease, and the rate of progression can vary. On average, individuals live 6 to 8 years after the onset of symptoms, but this can range from 2 to over 20 years.
See also
Ad. Transform your life with W8MD's
GLP-1 weight loss injections special from $29.99 with insurance
|
WikiMD Medical Encyclopedia |
Medical Disclaimer: WikiMD is for informational purposes only and is not a substitute for professional medical advice. Content may be inaccurate or outdated and should not be used for diagnosis or treatment. Always consult your healthcare provider for medical decisions. Verify information with trusted sources such as CDC.gov and NIH.gov. By using this site, you agree that WikiMD is not liable for any outcomes related to its content. See full disclaimer.
Credits:Most images are courtesy of Wikimedia commons, and templates, categories Wikipedia, licensed under CC BY SA or similar.
Translate this page: - East Asian
中文,
日本,
한국어,
South Asian
हिन्दी,
தமிழ்,
తెలుగు,
Urdu,
ಕನ್ನಡ,
Southeast Asian
Indonesian,
Vietnamese,
Thai,
မြန်မာဘာသာ,
বাংলা
European
español,
Deutsch,
français,
Greek,
português do Brasil,
polski,
română,
русский,
Nederlands,
norsk,
svenska,
suomi,
Italian
Middle Eastern & African
عربى,
Turkish,
Persian,
Hebrew,
Afrikaans,
isiZulu,
Kiswahili,
Other
Bulgarian,
Hungarian,
Czech,
Swedish,
മലയാളം,
मराठी,
ਪੰਜਾਬੀ,
ગુજરાતી,
Portuguese,
Ukrainian