Tucker syndrome: Difference between revisions
CSV import |
CSV import |
||
| Line 1: | Line 1: | ||
{{SI}} | |||
{{Infobox medical condition | |||
| name = Tucker syndrome | |||
| image = [[File:Recurrent_laryngeal_nerve.svg|250px]] | |||
| image_size = 250px | |||
| alt = Diagram showing the recurrent laryngeal nerve | |||
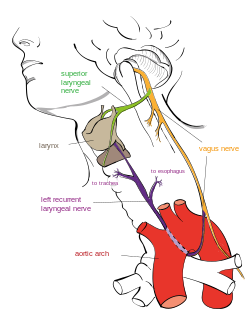
| caption = Diagram of the recurrent laryngeal nerve, which may be affected in Tucker syndrome | |||
| field = [[Otolaryngology]] | |||
| symptoms = [[Hoarseness]], [[dysphagia]], [[stridor]] | |||
| complications = [[Respiratory distress]], [[aspiration pneumonia]] | |||
| onset = Congenital or acquired | |||
| duration = Chronic | |||
| causes = Genetic mutation, [[trauma]], [[surgery]] | |||
| risks = Family history, [[neck surgery]] | |||
| diagnosis = [[Laryngoscopy]], [[CT scan]], [[genetic testing]] | |||
| differential = [[Vocal cord paralysis]], [[laryngeal cancer]] | |||
| prevention = Avoidance of neck trauma, genetic counseling | |||
| treatment = [[Speech therapy]], [[surgical intervention]] | |||
| medication = [[Corticosteroids]], [[antibiotics]] | |||
| prognosis = Variable, depending on severity | |||
| frequency = Rare | |||
}} | |||
{{Short description|A rare neurological disorder affecting the recurrent laryngeal nerve}} | {{Short description|A rare neurological disorder affecting the recurrent laryngeal nerve}} | ||
'''Tucker syndrome''' is a rare neurological disorder characterized by dysfunction of the [[recurrent laryngeal nerve]], which can lead to vocal cord paralysis and other associated symptoms. This condition is named after the physician who first described it. | '''Tucker syndrome''' is a rare neurological disorder characterized by dysfunction of the [[recurrent laryngeal nerve]], which can lead to vocal cord paralysis and other associated symptoms. This condition is named after the physician who first described it. | ||
== Pathophysiology == | == Pathophysiology == | ||
The [[recurrent laryngeal nerve]] is a branch of the [[vagus nerve]] that supplies motor function and sensation to the larynx. In Tucker syndrome, this nerve is affected, leading to impaired movement of the vocal cords. The exact etiology of the nerve dysfunction in Tucker syndrome is not well understood, but it may involve genetic, autoimmune, or idiopathic factors. | The [[recurrent laryngeal nerve]] is a branch of the [[vagus nerve]] that supplies motor function and sensation to the larynx. In Tucker syndrome, this nerve is affected, leading to impaired movement of the vocal cords. The exact etiology of the nerve dysfunction in Tucker syndrome is not well understood, but it may involve genetic, autoimmune, or idiopathic factors. | ||
== Clinical Presentation == | == Clinical Presentation == | ||
Patients with Tucker syndrome typically present with symptoms related to vocal cord paralysis, including: | Patients with Tucker syndrome typically present with symptoms related to vocal cord paralysis, including: | ||
| Line 14: | Line 32: | ||
* [[Stridor]] | * [[Stridor]] | ||
* [[Dyspnea]] | * [[Dyspnea]] | ||
The severity of symptoms can vary depending on the extent of nerve involvement and whether one or both vocal cords are affected. | The severity of symptoms can vary depending on the extent of nerve involvement and whether one or both vocal cords are affected. | ||
== Diagnosis == | == Diagnosis == | ||
The diagnosis of Tucker syndrome is primarily clinical, based on the characteristic symptoms and the exclusion of other causes of recurrent laryngeal nerve palsy. Diagnostic tools may include: | The diagnosis of Tucker syndrome is primarily clinical, based on the characteristic symptoms and the exclusion of other causes of recurrent laryngeal nerve palsy. Diagnostic tools may include: | ||
| Line 22: | Line 38: | ||
* [[Electromyography]] (EMG) to assess nerve function | * [[Electromyography]] (EMG) to assess nerve function | ||
* Imaging studies such as [[MRI]] or [[CT scan]] to rule out structural causes | * Imaging studies such as [[MRI]] or [[CT scan]] to rule out structural causes | ||
== Management == | == Management == | ||
Treatment of Tucker syndrome focuses on managing symptoms and improving quality of life. Options may include: | Treatment of Tucker syndrome focuses on managing symptoms and improving quality of life. Options may include: | ||
| Line 28: | Line 43: | ||
* Surgical interventions such as [[medialization thyroplasty]] | * Surgical interventions such as [[medialization thyroplasty]] | ||
* Use of [[botulinum toxin]] injections to reduce muscle spasms | * Use of [[botulinum toxin]] injections to reduce muscle spasms | ||
== Prognosis == | == Prognosis == | ||
The prognosis for individuals with Tucker syndrome varies. Some patients may experience spontaneous recovery of nerve function, while others may have persistent symptoms requiring ongoing management. | The prognosis for individuals with Tucker syndrome varies. Some patients may experience spontaneous recovery of nerve function, while others may have persistent symptoms requiring ongoing management. | ||
== See Also == | |||
== | |||
* [[Recurrent laryngeal nerve]] | * [[Recurrent laryngeal nerve]] | ||
* [[Vocal cord paralysis]] | * [[Vocal cord paralysis]] | ||
* [[Vagus nerve]] | * [[Vagus nerve]] | ||
[[Category:Neurological disorders]] | [[Category:Neurological disorders]] | ||
[[Category:Rare diseases]] | [[Category:Rare diseases]] | ||
Latest revision as of 07:44, 6 April 2025

Editor-In-Chief: Prab R Tumpati, MD
Obesity, Sleep & Internal medicine
Founder, WikiMD Wellnesspedia &
W8MD's medical weight loss NYC, sleep center NYC
Philadelphia medical weight loss and Philadelphia sleep clinics
| Tucker syndrome | |
|---|---|
| |
| Synonyms | N/A |
| Pronounce | N/A |
| Specialty | N/A |
| Symptoms | Hoarseness, dysphagia, stridor |
| Complications | Respiratory distress, aspiration pneumonia |
| Onset | Congenital or acquired |
| Duration | Chronic |
| Types | N/A |
| Causes | Genetic mutation, trauma, surgery |
| Risks | Family history, neck surgery |
| Diagnosis | Laryngoscopy, CT scan, genetic testing |
| Differential diagnosis | Vocal cord paralysis, laryngeal cancer |
| Prevention | Avoidance of neck trauma, genetic counseling |
| Treatment | Speech therapy, surgical intervention |
| Medication | Corticosteroids, antibiotics |
| Prognosis | Variable, depending on severity |
| Frequency | Rare |
| Deaths | N/A |
A rare neurological disorder affecting the recurrent laryngeal nerve
Tucker syndrome is a rare neurological disorder characterized by dysfunction of the recurrent laryngeal nerve, which can lead to vocal cord paralysis and other associated symptoms. This condition is named after the physician who first described it.
Pathophysiology[edit]
The recurrent laryngeal nerve is a branch of the vagus nerve that supplies motor function and sensation to the larynx. In Tucker syndrome, this nerve is affected, leading to impaired movement of the vocal cords. The exact etiology of the nerve dysfunction in Tucker syndrome is not well understood, but it may involve genetic, autoimmune, or idiopathic factors.
Clinical Presentation[edit]
Patients with Tucker syndrome typically present with symptoms related to vocal cord paralysis, including:
The severity of symptoms can vary depending on the extent of nerve involvement and whether one or both vocal cords are affected.
Diagnosis[edit]
The diagnosis of Tucker syndrome is primarily clinical, based on the characteristic symptoms and the exclusion of other causes of recurrent laryngeal nerve palsy. Diagnostic tools may include:
- Laryngoscopy to visualize vocal cord movement
- Electromyography (EMG) to assess nerve function
- Imaging studies such as MRI or CT scan to rule out structural causes
Management[edit]
Treatment of Tucker syndrome focuses on managing symptoms and improving quality of life. Options may include:
- Voice therapy with a speech-language pathologist
- Surgical interventions such as medialization thyroplasty
- Use of botulinum toxin injections to reduce muscle spasms
Prognosis[edit]
The prognosis for individuals with Tucker syndrome varies. Some patients may experience spontaneous recovery of nerve function, while others may have persistent symptoms requiring ongoing management.