Passive antibody therapy: Difference between revisions
CSV import |
CSV import |
||
| Line 27: | Line 27: | ||
[[Category:Therapy]] | [[Category:Therapy]] | ||
{{stub}} | {{stub}} | ||
== Passive_antibody_therapy == | |||
<gallery> | |||
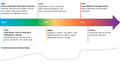
File:Passive_antibody_therapy_timeline_(1890-2020).png|Timeline of passive antibody therapy from 1890 to 2020 | |||
File:Monoclonal_antibodies_smaller.jpg|Illustration of monoclonal antibodies | |||
File:2212_Complement_Cascade_and_Function.jpg|Diagram of the complement cascade and its function | |||
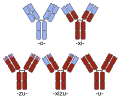
File:Chimeric_and_humanized_antibodies.svg|Chimeric and humanized antibodies | |||
File:Rituxima_Binding_to_CD20_on_a_B_Cell_Surface_(6830897205).jpg|Rituximab binding to CD20 on a B cell surface | |||
File:Antibody-drug_conjugate_structure.svg|Structure of an antibody-drug conjugate | |||
File:HIV_attachment.gif|HIV attachment process | |||
</gallery> | |||
Latest revision as of 11:36, 18 February 2025
Passive antibody therapy is a type of medical treatment that involves the administration of antibodies to a patient. These antibodies are typically produced outside the body and are given to the patient to help fight off infection or disease. This type of therapy is often used when the body's own immune system is not able to produce enough antibodies to effectively combat a disease.
History[edit]
The concept of passive antibody therapy dates back to the late 19th century, when Emil von Behring and Shibasaburo Kitasato discovered that they could treat diphtheria and tetanus by injecting patients with serum from animals that had been immunized against these diseases. This discovery earned von Behring the first Nobel Prize in Physiology or Medicine in 1901.
Mechanism of action[edit]
Passive antibody therapy works by introducing antibodies into the body that are specifically designed to target and neutralize a particular pathogen. These antibodies bind to the pathogen, marking it for destruction by the body's immune system. This can help to reduce the severity of the disease and speed up recovery.
Uses[edit]
Passive antibody therapy is used to treat a variety of diseases, including rabies, hepatitis B, and respiratory syncytial virus (RSV). It is also used as a preventative measure in individuals who are at high risk of infection, such as those with weakened immune systems.
Advantages and disadvantages[edit]
One of the main advantages of passive antibody therapy is that it provides immediate protection against disease, as the antibodies are ready to fight off the pathogen as soon as they are introduced into the body. This is in contrast to active immunization, which requires the body to produce its own antibodies in response to a vaccine, a process that can take several weeks.
However, passive antibody therapy also has some disadvantages. The protection it provides is temporary, as the antibodies are eventually broken down and removed from the body. In addition, there is a risk of adverse reactions, such as allergic reactions, especially when the antibodies are derived from animal sources.
Future directions[edit]
Research is ongoing into the use of passive antibody therapy for the treatment of other diseases, including cancer and HIV. There is also interest in developing synthetic antibodies, which could reduce the risk of adverse reactions and provide longer-lasting protection.
|
|
|
Passive_antibody_therapy[edit]
-
Timeline of passive antibody therapy from 1890 to 2020
-
Illustration of monoclonal antibodies
-
Diagram of the complement cascade and its function
-
Chimeric and humanized antibodies
-
Rituximab binding to CD20 on a B cell surface
-
Structure of an antibody-drug conjugate
-
HIV attachment process