Brugia timori: Difference between revisions
CSV import |
No edit summary |
||
| Line 24: | Line 24: | ||
[[Category:Nematodes]] | [[Category:Nematodes]] | ||
[[Category:Health in Indonesia]] | [[Category:Health in Indonesia]] | ||
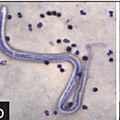
== Brugia timori == | == Brugia timori == | ||
<gallery> | <gallery> | ||
File:2-Figure2-1_(1).jpg|2-Figure2-1 (1) | File:2-Figure2-1_(1).jpg|2-Figure2-1 (1) | ||
</gallery> | </gallery> | ||
Revision as of 19:22, 16 March 2025
Brugia timori is a parasitic filarial nematode (roundworm) and one of the causative agents of lymphatic filariasis in humans. It is primarily found in certain parts of Indonesia, including the Lesser Sunda Islands. This parasite is transmitted to humans through the bites of infected mosquitoes, particularly those belonging to the genus Anopheles. The disease caused by Brugia timori is similar to that caused by the more widely known filarial parasites, Wuchereria bancrofti and Brugia malayi, which are responsible for the majority of lymphatic filariasis cases worldwide.
Life Cycle
The life cycle of Brugia timori involves two hosts: humans, where the adult worms reside, and mosquitoes, which act as vectors. When an infected mosquito bites a human, it injects the larvae, known as microfilariae, into the bloodstream. These microfilariae mature into adult worms within the human lymphatic system, where they can live for several years. The adult worms produce millions of microfilariae, which circulate in the blood and can be ingested by mosquitoes during a blood meal, thus continuing the cycle.
Symptoms and Diagnosis
In the early stages of infection, individuals may not exhibit symptoms. However, as the disease progresses, it can lead to a condition known as lymphatic filariasis, characterized by severe swelling (lymphedema) and thickening of the skin and underlying tissues, often in the legs and genitals, a condition known as elephantiasis. Acute episodes of local inflammation involving skin, lymph nodes, and lymphatic vessels often occur and can be debilitating.
Diagnosis of Brugia timori infection is typically made by detecting microfilariae in peripheral blood smears. Blood samples are usually collected at night, coinciding with the nocturnal periodicity of the microfilariae. Molecular diagnostic tools, such as PCR, can also be used to detect parasite DNA in blood samples.
Treatment and Prevention
The treatment for Brugia timori infection involves antifilarial medications, such as diethylcarbamazine (DEC), which can kill the microfilariae and some adult worms. Preventive measures focus on controlling mosquito populations and preventing bites. This includes using insecticide-treated bed nets, applying mosquito repellents, and eliminating mosquito breeding sites.
Mass drug administration (MDA) of antifilarial drugs to at-risk populations is a key strategy in the global effort to eliminate lymphatic filariasis. However, Brugia timori has been less studied than Wuchereria bancrofti and Brugia malayi, and specific strategies for its control and elimination may require further research.
Epidemiology
Brugia timori is endemic to a limited geographical area in Southeast Asia, particularly the Lesser Sunda Islands of Indonesia. Its distribution is more localized compared to Wuchereria bancrofti and Brugia malayi, which have a broader global distribution. The restricted range of Brugia timori may offer opportunities for targeted control measures and eventual elimination in its endemic areas.
Research and Future Directions
Research on Brugia timori is ongoing, with studies focusing on its epidemiology, life cycle, and interactions with the human immune system. Understanding the genetic diversity of Brugia timori and its mosquito vectors may provide insights into the transmission dynamics and potential resistance to treatments. Efforts to develop vaccines against lymphatic filariasis could also benefit from a better understanding of Brugia timori and its pathogenesis.
Brugia timori
-
2-Figure2-1 (1)